Why Does My Gum Hurt in One Spot? Reasons & Fixes 2026
Why Does My Gum Hurt in One Spot? This is one of the most common dental complaints people search for in 2026.
Localized gum pain can range from a mild, dull ache to a sharp, throbbing sensation that makes eating and brushing uncomfortable.
Unlike general gum soreness, pain in a single area usually points to one specific cause.
The good news is that most reasons are treatable, especially when caught early.
This guide covers every major cause, how to fix it at home, and when you must see a dentist.
What Does It Mean When Your Gum Hurts in Just One Spot?
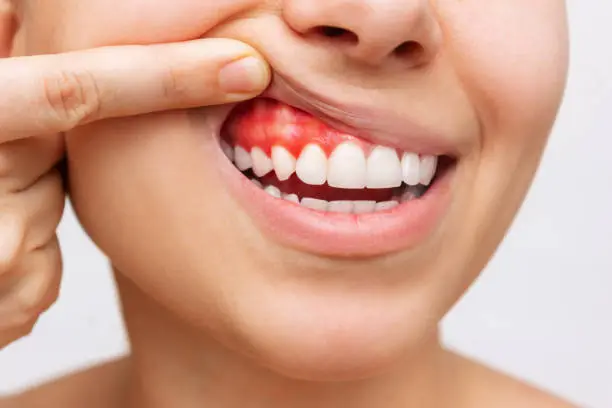
When pain is limited to one area of your gums, it almost always means something local is irritating or infecting that specific tissue.
Unlike widespread gum soreness caused by hormonal shifts or illness, localized pain points to a targeted problem — trapped food, an injury, an infection, or an early dental issue in that exact zone.
Paying close attention to where the pain is, how long it lasts, and what makes it worse will help you narrow down the cause quickly.
Common Reasons Why Your Gum Hurts in One Spot
1. Trapped Food or Debris Between Teeth
One of the most frequent causes of gum pain in a single spot is food lodged between the tooth and gum.
Popcorn kernels, seeds, small chips, or meat fibers can press into the gum tissue and create pressure, swelling, and sharp pain.
If left there, trapped debris becomes a breeding ground for bacteria, which can lead to a minor infection fast.
Fix: Floss gently around the sore spot and rinse with warm saltwater. Never use toothpicks or sharp objects to dig out debris.
2. Brushing or Flossing Too Hard
Aggressive brushing is a leading cause of localized gum injury that most people overlook.
Using a hard-bristled toothbrush or snapping floss down too forcefully can cut or bruise a small section of gum tissue, leaving it red, tender, and sore for several days.
The damage looks minor but the tissue underneath can stay inflamed longer than expected.
Fix: Switch to a soft-bristled toothbrush immediately. Brush in gentle, circular motions and slide floss carefully instead of snapping it into place.
3. Canker Sore on the Gum
A canker sore (aphthous ulcer) is a small, shallow lesion that can form directly on the gum tissue.
These sores cause sharp, stinging pain concentrated in one tiny spot and are often triggered by stress, minor injury, hormonal changes, or acidic foods.
They usually measure only a few millimeters but feel disproportionately painful.
Fix: Avoid spicy, acidic, or salty foods. Apply an over-the-counter gel like benzocaine for temporary numbing. Most canker sores heal within 7 to 10 days on their own.
4. Gum Abscess or Dental Abscess
A gum abscess is a pocket of pus caused by a bacterial infection beneath the gumline, and it is one of the more serious causes of pain in one spot.
The pain from an abscess is usually deep, throbbing, and constant. You may also notice a small visible bump on the gum, swelling of the face or jaw, a foul taste in the mouth, or even a low-grade fever.
Dental abscesses can develop from untreated tooth decay, a cracked tooth, or trapped food that allowed bacteria to spread under the tissue.
Fix: This requires immediate professional dental care. An abscess will not heal on its own. Your dentist will drain the infection, prescribe antibiotics, and determine if a root canal or extraction is needed.
5. Gum Disease (Gingivitis or Periodontitis)

Gum disease does not always develop uniformly across the mouth. It frequently starts in one spot where plaque has built up along the gumline.
In the early stage — gingivitis — you may notice redness, mild swelling, or slight bleeding when brushing that one area. At this point it is reversible.
If left untreated, it progresses to periodontitis, which involves deeper infection, bone loss, and persistent pain.
Fix: Improve your brushing and flossing routine. See your dentist for a professional cleaning. Advanced cases may need scaling and root planing — a deep cleaning procedure that removes tartar from below the gumline.
6. Wisdom Tooth Eruption or Impaction
If the pain is at the very back of your mouth near your molars, an erupting or impacted wisdom tooth is a likely cause.
When a wisdom tooth pushes through the gum, the surrounding tissue becomes inflamed, swollen, and sore. Impacted wisdom teeth — those that cannot emerge properly — cause more intense, prolonged pain in that localized area.
This is especially common in people between the ages of 17 and 25 but can happen later in life too.
Fix: Rinse with warm saltwater to reduce inflammation. See a dentist or oral surgeon for an X-ray to determine whether extraction is needed.
7. Gum Recession
When gums recede, the sensitive root surface of the tooth becomes exposed, and that spot becomes more vulnerable to pain.
You may notice the gum looks lower around one tooth, and that particular area is sensitive to cold, heat, or touch.
Recession can be caused by aggressive brushing, gum disease, teeth grinding, or genetics.
Fix: Use a soft toothbrush and a sensitivity toothpaste. Your dentist may recommend a gum graft procedure if recession is significant.
8. Cracked Tooth or Dental Decay
A cracked tooth or a cavity that has reached the nerve can cause pain that radiates into the surrounding gum tissue.
The pain often feels like it is coming from the gum rather than the tooth, which is why many people do not immediately suspect the tooth itself.
The discomfort typically worsens when biting down or when consuming hot or cold foods.
Fix: See a dentist as soon as possible. Treatment may include a filling, crown, or root canal depending on the severity.
9. Ill-Fitting Dental Work
Crowns, braces, dentures, or retainers that do not fit properly can rub repeatedly against one spot of gum tissue.
This constant friction causes irritation, redness, and localized soreness that does not go away until the appliance is adjusted.
Fix: Contact your dentist or orthodontist to have the dental work adjusted. Do not try to fix it yourself at home.
10. Hormonal Changes
Hormonal fluctuations during menstruation, pregnancy, or menopause can make gum tissue more sensitive and reactive.
You may notice that one spot that was never a problem before becomes sore, swollen, or bleeds more easily during certain times of the month.
This happens because hormonal changes increase blood flow to the gums and alter how the tissue responds to plaque.
Fix: Maintain strict oral hygiene during hormonal shifts. Inform your dentist if you are pregnant or perimenopausal so they can adjust your care plan accordingly.
11. Oral Herpes (HSV-1 Viral Infection)
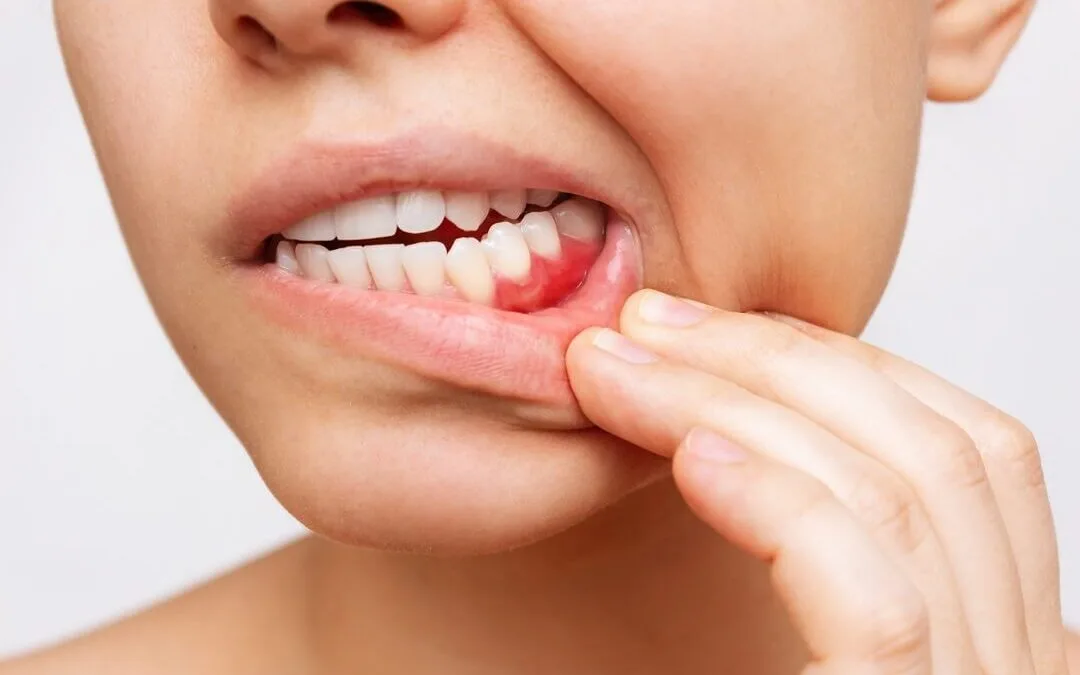
The herpes simplex virus can cause painful blisters or sores to appear on the gum in one localized spot.
These appear as small, white or yellow fluid-filled bumps that are extremely tender to the touch.
Unlike bacterial infections, viral sores typically clear up on their own within one to two weeks, though antiviral medications can shorten the duration.
Fix: Avoid touching the sore. Keep the area clean. Consult a doctor if sores are recurring or if you are immunocompromised.
Comparison Table: Common Causes at a Glance
| Cause | Pain Type | Visible Sign | Home Fix Possible? | See Dentist? |
|---|---|---|---|---|
| Trapped food | Sharp, pressure | Redness | Yes (floss + rinse) | If persists |
| Aggressive brushing | Tender, sore | Minor redness | Yes (soft brush) | If no improvement |
| Canker sore | Sharp, stinging | White/yellow sore | Yes (gel + rinse) | If lasts 2+ weeks |
| Gum abscess | Throbbing, deep | Visible bump, swelling | No | Immediately |
| Gum disease | Dull ache | Redness, bleeding | Partial | Yes |
| Wisdom tooth | Dull to sharp | Back gum swelling | Temporary | Yes |
| Gum recession | Sensitivity | Lower gum line | Partial | Yes |
| Cracked tooth | Deep, sharp | None visible | No | Yes |
| Ill-fitting dental work | Friction, dull | Rubbed area | No | Yes |
| Hormonal changes | Dull, tender | Mild swelling | Yes (hygiene) | If persistent |
| Viral infection | Stinging | Blisters/bumps | Partial | If recurring |
How to Relieve Gum Pain at Home
Before heading to the dentist, these home remedies can help manage mild gum pain safely.
Warm Saltwater Rinse
This is the most recommended first step for any localized gum discomfort.
Mix one teaspoon of salt into a glass of warm water and rinse for 30 seconds, two to three times a day. Salt reduces bacteria, draws out minor infections, and calms inflamed tissue.
Cold Compress on the Outside of the Cheek
Applying a cold pack wrapped in a cloth to the outside of your cheek for 15 minutes can reduce swelling and numb soreness temporarily.
This works especially well for abscesses or post-injury swelling. Never apply ice directly to the gum tissue.
Over-the-Counter Pain Relievers
Ibuprofen (an NSAID) is the best OTC option for gum pain because it reduces both pain and inflammation.
Acetaminophen works for pain relief only. Follow dosage instructions on the label. Do not apply aspirin directly to the gum — this can cause a chemical burn.
Clove Oil
Clove oil contains eugenol, a natural anesthetic compound that dentists have used for centuries.
Apply a tiny amount to a cotton ball and dab it on the sore spot. It provides short-term numbing. Do not use it in excess or in deep gum pockets.
Hydrogen Peroxide Rinse

Dilute 3% hydrogen peroxide with equal parts water and use it as a mouth rinse.
This kills bacteria in the sore area and can help with minor infections or canker sores. Spit it out completely and do not swallow.
Aloe Vera Gel
Pure aloe vera gel applied to the gum can soothe irritation and reduce inflammation due to its antibacterial and anti-inflammatory properties.
Use food-grade or dental-grade aloe vera, not a cosmetic product with additives.
When to See a Dentist — Do Not Wait
Some symptoms indicate you need professional care right away, not in a few days.
Go to the Dentist If You Notice
- Pain that has lasted more than 5 to 7 days without improvement
- Visible swelling of the gum, jaw, or face
- A bump or pus-filled blister on the gum
- A bad taste or foul smell from the area
- Bleeding that does not stop with gentle care
- Fever alongside gum pain
- Difficulty opening your mouth, swallowing, or eating
- Pain that is spreading to the jaw, ear, or neck
Dental infections can spread rapidly. An untreated abscess can become a serious medical emergency if the infection reaches deeper tissues or the bloodstream.
Gum Pain in One Spot by Location
Back of the Mouth (Near Molars)
Pain here is most commonly linked to wisdom teeth — either erupting or impacted. It can also indicate a gum pocket behind the last molar where food traps easily.
An X-ray is often needed to confirm what is happening in this area.
Upper Gum Pain in One Spot
The upper jaw has sinus roots running close to the back teeth. Pain in one upper gum spot may sometimes be referred sinus pain, especially during a cold or sinus infection.
A cracked upper tooth or abscess in this zone can also feel like sinus pressure.
Between Two Teeth (Interdental Gum Pain)
Pain directly between two teeth almost always points to trapped food or early gum disease starting in that interdental pocket.
Regular flossing prevents most of these episodes before they become painful.
Front Gum Pain in One Spot
The front gums are more likely to be injured by hard foods or aggressive brushing. A canker sore here is very common.
Check for a visible white or yellow sore before assuming something more serious.
How to Prevent Gum Pain from Coming Back
Prevention is simpler than treatment. These habits will protect your gums long-term.
Daily Oral Hygiene Routine
Brush twice a day with a soft-bristled toothbrush using gentle, circular motions. Brush for a full two minutes each time.
Floss once a day to remove food particles and plaque from between teeth before they irritate the gum.
Choose the Right Products
Use fluoride toothpaste and an antibacterial mouthwash daily. Avoid whitening toothpastes that contain abrasive particles if your gums are already sensitive.
Replace your toothbrush every three to four months, or sooner if the bristles are splayed.
Regular Dental Checkups
Visit your dentist every six months for a professional cleaning and exam.
A hygienist removes tartar that cannot be removed at home, and your dentist can catch early problems before they become painful.
Stay Hydrated and Eat Well
Drink enough water to prevent dry mouth, which allows bacteria to multiply faster.
Eat a diet rich in Vitamin C (citrus, leafy greens) and Vitamin D (dairy, eggs, sunlight) — both are essential for healthy gum tissue.
Avoid Smoking and Tobacco
Tobacco use is one of the biggest risk factors for gum disease. It reduces blood flow to the gums, masks early warning signs like bleeding, and significantly slows healing.
Quitting tobacco is one of the most impactful things you can do for your gum health.
Gum Pain vs. Tooth Pain — How to Tell the Difference
Many people struggle to tell whether the pain is coming from the gum or the tooth. Here is a simple guide.
| Feature | Gum Pain | Tooth Pain |
|---|---|---|
| Location | Soft tissue surface | Deep inside or below the tooth |
| Triggered by | Touch, brushing, pressure on gum | Hot, cold, biting down |
| Visible sign | Redness, swelling, sore on gum | Visible cavity, dark spot, crack |
| Type of pain | Tender, sore, throbbing | Sharp, shooting, aching |
| Spreads to | Jaw or nearby gum area | Ear, temple, jaw |
If you cannot tell whether it is gum or tooth pain, a dentist visit is the only reliable way to diagnose it accurately.
Gum Pain During Pregnancy
Pregnancy gingivitis is extremely common and affects up to 70% of pregnant women.
Hormonal surges increase blood flow to the gum tissue, making it more sensitive, puffy, and prone to bleeding — sometimes in just one localized area.
The condition usually resolves after delivery, but maintaining careful oral hygiene throughout pregnancy is essential. Inform your dentist that you are pregnant before any treatment.
Can Stress Cause Gum Pain in One Spot?
Yes. Psychological stress can cause gum pain in several indirect ways.
Stress suppresses the immune system, making it harder to fight off bacterial infections in the gums. It also triggers habits like jaw clenching, teeth grinding (bruxism), and nail biting — all of which put pressure on the gums.
Additionally, stress is one of the most common triggers for canker sores.
Managing stress through sleep, exercise, and relaxation techniques indirectly benefits your gum health.
Frequently Asked Questions (FAQs)
Q1. Why does my gum hurt in one spot but looks normal?
Pain can come from beneath the gum surface where the tissue appears healthy on the outside. A trapped food particle, early infection, or nerve irritation from a nearby tooth can cause soreness without visible changes.
Q2. How long should gum pain in one spot last?
Mild gum pain from minor irritation usually clears up within 3 to 5 days with good home care. If the pain persists beyond one week, you need to see a dentist.
Q3. Can a cavity cause gum pain in one spot?
Yes. Decay near the gumline or a cavity that has reached the root can create pain that feels like it is coming from the gum rather than the tooth itself.
Q4. Is it normal for gums to hurt in one spot randomly?
Occasional soreness in one spot is common and usually harmless. However, recurring or worsening pain in the same spot is not normal and should be evaluated by a dentist.
Q5. What is the fastest way to relieve gum pain at home?
A warm saltwater rinse combined with an OTC anti-inflammatory like ibuprofen provides the fastest reliable relief for most types of localized gum pain.
Q6. Can stress cause my gum to hurt in one specific area?
Yes. Stress weakens the immune system and triggers habits like teeth grinding that put pressure on specific gum areas. It is also a primary trigger for canker sores, which cause sharp localized pain.
Q7. Why does my gum hurt in one spot at the back of my mouth?
Back-of-mouth gum pain is most frequently caused by an erupting or impacted wisdom tooth. A gum pocket forming behind the last molar or a dental abscess in that area are also common culprits.
Q8. Should I see a dentist if only one spot on my gum hurts?
Yes, if the pain lasts more than 5 to 7 days, worsens, or is accompanied by swelling, a bump, foul taste, or fever. Minor pain that resolves in a few days is usually manageable at home.
Q9. Can gum disease affect just one spot?
Yes. Gum disease often begins in a single area where plaque has accumulated heavily, especially around a tooth that is harder to clean properly with a toothbrush or floss.
Q10. What is a gum abscess and how do I know if I have one?
A gum abscess is a pus-filled pocket caused by a bacterial infection. Signs include deep throbbing pain, a visible bump on the gum, foul taste, facial swelling, and sometimes fever. It requires immediate dental treatment.
Conclusion
Gum pain in one spot is rarely random — it almost always has a clear, identifiable cause.
Whether it is as simple as a piece of trapped food or as serious as a dental abscess, the key is to act promptly and not ignore persistent pain.
Start with home remedies like warm saltwater rinses, gentle flossing, and soft-bristled brushing.
If the pain lasts more than a week, spreads, or comes with swelling and fever, see a dentist without delay.
The sooner you identify the cause, the faster you heal and the lower your risk of complications.
Protect your gums daily with proper hygiene, regular dental checkups, and a healthy diet.
Your gums are the foundation of your entire oral health — treat them with care.