Why Is the Roof of My Mouth Itchy? Allergy or Infection 2026
Why is the roof of my mouth itchy — this is one of the most searched health questions in 2026, and for good reason. That persistent tickling, tingling, or scratchy sensation on your palate can be mildly annoying or a sign of something that needs medical attention.
The most common causes are seasonal allergies, oral allergy syndrome, viral infections, fungal infections, dry mouth, and sinus pressure. Some cases resolve in minutes on their own. Others require prescription treatment.
What Is the Roof of Your Mouth and Why Does It Itch?
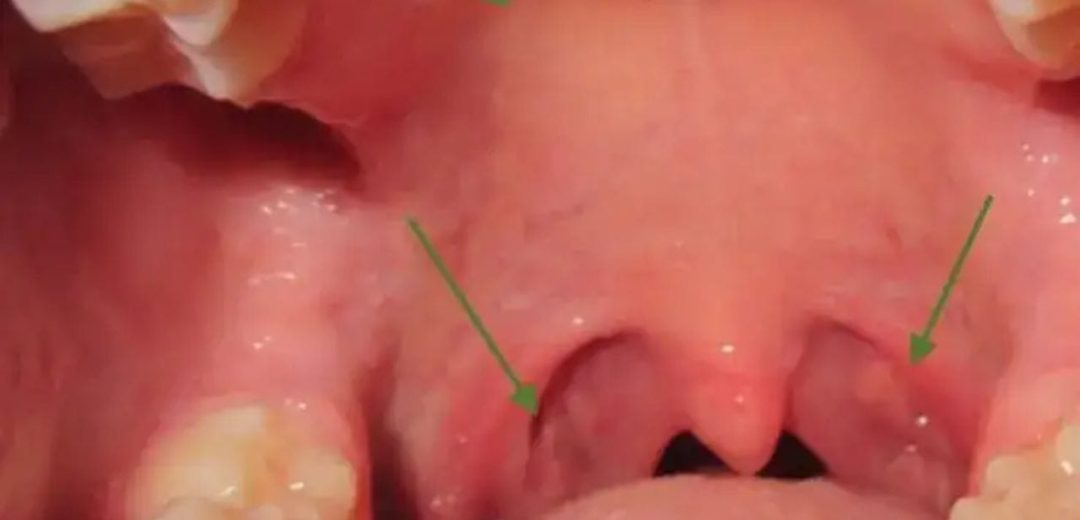
The roof of your mouth is called the palate. It has two sections — the hard palate at the front, which is firm and bony, and the soft palate at the back, which is flexible and muscular.
The palate is lined with mucous membranes that contain blood vessels, nerve endings, and immune-active tissue. When this tissue is exposed to allergens, pathogens, irritants, or inflammation from nearby structures like the sinuses, it responds with a familiar itching or tingling sensation.
Because the palate sits directly below the nasal passages and sinuses, it is especially sensitive to anything affecting the upper respiratory system. That is why sneezing, congestion, and post-nasal drip so often go hand in hand with an itchy roof of the mouth.
All Causes of Itchy Roof of Mouth — Quick Overview
| Cause | Onset | Both or One Side | Urgency Level |
|---|---|---|---|
| Seasonal allergies / hay fever | Gradual, seasonal | Both | Low |
| Oral allergy syndrome (OAS) | Within minutes of eating | Both | Low–Medium |
| Food allergy | Rapid, within 30 min | Both | Medium–High |
| Common cold or flu | Gradual | Both | Low |
| Oral thrush (fungal infection) | Gradual | Both | Medium |
| Cold sores / oral herpes | Before blister appearance | Localized | Low–Medium |
| Dry mouth (xerostomia) | Persistent | Both | Low–Medium |
| Sinus infection / sinusitis | With sinus symptoms | Both | Medium |
| Dental irritants / gum disease | After dental work or flare | Localized | Low–Medium |
| Burns from hot food | Immediate | Localized | Low |
| Drug side effects | After new medication | Both | Medium |
| Latex allergy | After latex contact | Both | Medium–High |
| Anaphylaxis (severe reaction) | Sudden, rapid | Both | Emergency |
Cause 1: Seasonal Allergies and Hay Fever
Seasonal allergies — also called allergic rhinitis or hay fever — are the most common cause of an itchy roof of the mouth. When your immune system overreacts to pollen from trees, grasses, or weeds, it releases histamine throughout the body.
Histamine causes inflammation and itching in soft tissues, and the mucous membranes of the palate are among the first places this shows up. The itching usually appears alongside sneezing, a runny or stuffy nose, watery eyes, and throat irritation.
Symptoms are predictable — they flare during specific pollen seasons (spring and fall are most common) and improve when you are indoors or when pollen counts drop.
Common seasonal triggers: Birch tree pollen (spring), grass pollen (late spring to summer), ragweed pollen (late summer to fall), mold spores (damp weather), dust mites (year-round).
Treatment: Over-the-counter antihistamines like cetirizine (Zyrtec), fexofenadine (Allegra), or loratadine (Claritin) are the first line of treatment. Nasal corticosteroid sprays like fluticasone (Flonase) reduce inflammation in the nasal passages and also relieve palate itching linked to post-nasal drip. For severe or persistent seasonal allergies, an allergist may recommend allergen immunotherapy — a course of allergy shots or sublingual drops that gradually desensitize the immune system.
Cause 2: Oral Allergy Syndrome (OAS) — Pollen-Food Allergy Syndrome
Oral allergy syndrome is the most commonly misunderstood cause of an itchy palate. It is also known as pollen-food allergy syndrome (PFAS) and affects as many as 1 in 3 people with seasonal pollen allergies.
OAS occurs when your immune system confuses proteins in certain raw fruits, vegetables, and nuts with pollen proteins. Because these food proteins are structurally similar to pollen, the immune system mounts an allergic response as if you have been exposed to the pollen you are already sensitized to.
Symptoms appear rapidly — usually within a few minutes of eating the trigger food. You will feel itching, tingling, or mild swelling in the lips, tongue, roof of the mouth, and throat. The reaction is almost always limited to the mouth and throat and resolves within 20–30 minutes of spitting out or swallowing the food.
Cooking, microwaving, or peeling the food destroys the cross-reactive proteins, which is why most people with OAS can eat the same foods in cooked, canned, or processed form without any reaction.
Pollen-food cross-reaction table:
| Pollen Allergy | Foods That Commonly Trigger OAS |
|---|---|
| Birch tree pollen | Apples, pears, cherries, peaches, plums, carrots, celery, almonds, hazelnuts, kiwi |
| Grass pollen | Celery, melons, oranges, peaches, tomatoes |
| Ragweed pollen | Bananas, cucumbers, melons, zucchini, sunflower seeds |
| Mugwort pollen | Celery, apples, carrots, spices (coriander, fennel) |
Treatment: Stop eating the trigger food. Drink water to clear the mouth. Mild OAS symptoms resolve on their own within 30 minutes. For more bothersome symptoms, a non-sedating antihistamine like Benadryl or Allegra speeds relief. Avoid the raw form of trigger foods during high pollen season, when OAS symptoms are most intense. Long-term treatment with pollen-specific immunotherapy can reduce OAS severity by reducing overall pollen sensitivity.
Cause 3: True Food Allergy
A true food allergy is more serious than oral allergy syndrome and requires a different level of caution. Where OAS is caused by cross-reactive pollen proteins, a true food allergy is an IgE-mediated immune response to a food protein itself.
True food allergies cause symptoms that extend beyond the mouth. Along with an itchy palate, you may experience hives, swelling of the lips or tongue, stomach pain, vomiting, difficulty breathing, or a drop in blood pressure. These reactions can progress to anaphylaxis — a life-threatening emergency.
Common food allergens include peanuts, tree nuts, shellfish, fish, milk, eggs, wheat, and soy. Symptoms typically begin within 30 minutes of eating the allergen.
Warning signs that require emergency care: Throat tightening or difficulty breathing, swelling of the tongue or lips that restricts airway, dizziness or fainting, rapid heartbeat, or skin turning pale or blue.
Treatment: Mild reactions can be managed with antihistamines. Anyone with a known severe food allergy should carry an epinephrine auto-injector (EpiPen or Auvi-Q) at all times. Anaphylaxis is treated with an intramuscular injection of epinephrine and emergency medical care. Call 911 immediately if you suspect anaphylaxis.
Cause 4: Common Cold and Flu
A common cold or flu virus can cause an itchy, scratchy, or sore feeling on the roof of the mouth. This happens because the virus inflames the mucous membranes lining the nose, throat, and palate.
Post-nasal drip — when excess mucus runs from the nasal passages down the back of the throat — is a major contributor to palate itching during a cold. The constant dripping irritates the soft palate and the back of the throat.
Cold-related palate itching is usually accompanied by a runny or stuffy nose, sneezing, sore throat, fatigue, and possibly a low-grade fever. Symptoms generally resolve within 1–2 weeks as the infection clears.
Treatment: Rest, stay well hydrated, and eat nutritious foods. Use a humidifier to keep air moist and soothe irritated mucous membranes. Over-the-counter decongestants reduce nasal congestion and lessen post-nasal drip. Saline nasal sprays help flush the nasal passages. Sipping warm liquids like broth or herbal tea soothes the palate. There is no prescription cure for a cold — treatment is supportive and focused on managing symptoms while the immune system does its job.
Cause 5: Oral Thrush (Candida Fungal Infection)
Oral thrush — medically known as oral candidiasis — is a fungal infection caused by the overgrowth of Candida albicans yeast in the mouth. It is a common and very recognizable cause of an itchy, sore palate.
The hallmark sign is white or yellowish cottage cheese-like patches on the tongue, inner cheeks, gums, and roof of the mouth. The tissue beneath these patches is often red and inflamed. Affected areas may feel sore, itchy, or have a burning sensation. Some people describe a cottony feeling in the mouth or difficulty tasting food.
Who is most at risk for oral thrush:
People with weakened immune systems (HIV/AIDS, cancer, organ transplant recipients), those who use inhaled corticosteroids (like asthma inhalers) and do not rinse their mouth afterward, people taking broad-spectrum antibiotics that disrupt the natural oral microbiome, denture wearers who do not clean their dentures thoroughly, people with uncontrolled diabetes, babies and elderly adults, and smokers.
Treatment: Oral thrush does not clear up on its own without antifungal treatment. A doctor will prescribe antifungal medication — most commonly nystatin (as a liquid mouthwash or lozenges) for mild cases. Fluconazole tablets are used for more persistent infections. Always finish the full course of treatment. To prevent recurrence, rinse your mouth with water or brush your teeth after using corticosteroid inhalers, remove and clean dentures every night, practice good oral hygiene, and manage blood sugar levels if diabetic.
Cause 6: Cold Sores (Oral Herpes — Herpes Simplex Virus Type 1)

Cold sores are caused by the herpes simplex virus type 1 (HSV-1). Before a blister actually appears, the affected area — which can include the roof of the mouth — goes through a prodromal phase of tingling, itching, or burning.
This itchy warning phase typically lasts 1–2 days before the characteristic blisters develop. Cold sores most commonly appear on or around the lips, but they can also form on the hard palate, gums, and inside the cheeks.
HSV-1 stays dormant in the body and reactivates in response to triggers like stress, sun exposure, illness, hormonal changes, or a weakened immune system.
Treatment: There is no cure for HSV-1, but antiviral medications significantly reduce the duration and severity of outbreaks. Topical antivirals like acyclovir cream (Zovirax) applied at the first tingling sign can shorten outbreaks. Oral antivirals — acyclovir, valacyclovir (Valtrex), or famciclovir — are prescribed for frequent or severe outbreaks or for people who are immunocompromised. Over-the-counter docosanol (Abreva) is a topical option for mild outbreaks.
Cause 7: Dry Mouth (Xerostomia)
Dry mouth — medically called xerostomia — happens when the salivary glands produce insufficient saliva to keep the mouth properly lubricated. Saliva does far more than simply keep the mouth moist. It protects the mucous membranes, washes away bacteria, neutralizes acid, and maintains the natural balance of oral microorganisms.
When saliva production drops, the tissues of the palate become dry, irritated, and sensitive. This often presents as a persistent itching, tingling, or rough sensation on the roof of the mouth.
Common causes of dry mouth: Dehydration, mouth breathing (especially during sleep), antihistamines, antidepressants, blood pressure medications, diuretics, antipsychotics, anxiety medications, radiation therapy to the head or neck, diabetes, Sjögren’s syndrome (an autoimmune condition that attacks moisture-producing glands), and aging.
Treatment: Sip water frequently throughout the day — small, regular sips are more effective than drinking large amounts at once. Chew sugar-free gum or suck on sugar-free candies to stimulate saliva production. Use a humidifier while sleeping to reduce nighttime mouth dryness. Ask your doctor whether a medication you take may be contributing and if an alternative is available. Prescription saliva substitutes or saliva-stimulating medications (pilocarpine) are available for severe cases. Avoid alcohol, caffeine, and tobacco, all of which worsen dry mouth.
Cause 8: Sinus Infection (Sinusitis)
Your sinuses sit directly above the roof of your mouth. When your sinuses become inflamed and congested — whether from a bacterial infection, viral infection, or allergies — the pressure and inflammation can create a sensation of itching or discomfort on the palate.
The connection is both anatomical and inflammatory. Post-nasal drip from congested sinuses drains directly onto the soft palate, causing irritation. The shared nerve pathways between the sinus cavities and palate mean that sinus inflammation is often felt as palate discomfort.
Sinus-related palate itching is almost always accompanied by other sinus symptoms: nasal congestion, facial pressure or pain (especially behind the eyes and cheekbones), headache, thick nasal discharge, and sometimes fever.
Treatment: Saline nasal irrigation (using a neti pot or squeeze bottle) flushes the sinuses and reduces irritation. Over-the-counter decongestants such as pseudoephedrine or oxymetazoline nasal spray (Afrin, used for no more than 3 consecutive days) relieve congestion. Nasal corticosteroid sprays reduce inflammation. Viral sinusitis resolves on its own within 10–14 days. Bacterial sinusitis that does not improve after 10 days or worsens may require antibiotics prescribed by a doctor.
Cause 9: Dental Problems and Oral Irritants
The mouth is a complex environment where problems with teeth, gums, and dental appliances can easily cause palate discomfort.
Poorly fitting dentures or dental appliances that rub against the palate create mechanical irritation that leads to itching, soreness, or ulceration. Gum disease — particularly periodontitis — causes inflammation that can spread to the roof of the mouth. Recent dental procedures including extractions, fillings, or root canals can cause temporary sensitivity and itching in surrounding tissues as they heal.
Some toothpastes contain sodium lauryl sulfate (SLS), a foaming agent that irritates sensitive oral tissues in some people. Strong mouthwashes containing alcohol can also dry out and irritate the palate lining.
Treatment: Have dentures checked and adjusted if they cause persistent irritation. Treat gum disease with professional cleaning and improved oral hygiene. Switch to an SLS-free toothpaste or an alcohol-free mouthwash if these products seem to trigger symptoms. Allow post-dental-procedure sensitivity to resolve naturally — usually within a few days to a week.
Cause 10: Burns from Hot Food or Liquid
Burning the roof of the mouth on hot food or drinks — especially pizza, soups, coffee, or hot beverages — is extremely common. The hard palate is one of the first areas to contact hot food, and its thin tissue layer burns quickly.
Immediately after the burn, you will feel pain and tenderness. As the burn heals over 3–7 days, the tissue goes through an itching phase as new cells regenerate — similar to how healing skin on the body itches as it repairs itself.
Treatment: Drink cool water immediately after a burn to stop heat damage. Suck on ice chips or cold water to soothe the area. Avoid spicy, acidic, or very hot foods while the palate heals. Over-the-counter oral analgesics like benzocaine gel can numb discomfort temporarily. Most mouth burns heal completely within a week without any special treatment.
Cause 11: Medication Side Effects
Certain medications cause oral side effects including dryness, burning, and itching of the palate. These are not necessarily allergic reactions to the drug — they may be direct pharmacological effects on the salivary glands or oral tissues.
Common medication-related culprits include antihistamines (ironically, while treating allergies), antidepressants, blood pressure medications (particularly ACE inhibitors, which can cause a persistent itchy or tickly feeling in the throat and palate), diuretics, antipsychotics, and some cancer medications including Afinitor, Gilotrif, and Nexavar.
Treatment: Do not stop a prescribed medication without consulting your doctor. If you develop new oral symptoms after starting a medication, inform your prescriber. A dosage adjustment or alternative medication may be available. Treating medication-induced dry mouth with increased hydration and saliva substitutes can relieve palate itching associated with reduced saliva.
Cause 12: Latex Allergy
Latex allergy can cause oral itching and swelling after contact with latex-containing products. This is relevant during dental procedures where latex gloves are used, or when eating foods with latex cross-reactivity.
Latex cross-reactive foods include bananas, avocados, kiwi, chestnuts, and tomatoes. If you experience oral itching specifically during or after dental visits where latex gloves were used, mention this to your dentist and allergist.
Treatment: Inform your healthcare providers of any latex sensitivity. Request latex-free gloves and equipment. Avoid foods that cross-react with latex if sensitized. An allergist can confirm a latex allergy through skin prick testing or blood testing.
How to Tell Allergies from Infection — Side-by-Side Comparison
This is the most frequently asked question about an itchy roof of the mouth. Use this comparison to narrow down the likely cause.
| Feature | Allergies / OAS | Infection (Cold, Thrush, Herpes) |
|---|---|---|
| Onset | Predictable, seasonal, or after eating | Gradual, after illness exposure |
| Duration | Minutes to hours (OAS); seasonal (hay fever) | Days to weeks |
| White patches in mouth | No | Yes (oral thrush) |
| Blisters or sores | No | Yes (cold sores) |
| Fever | No | Possible (cold, flu, sinusitis) |
| Runny nose / sneezing | Yes (hay fever) | Possible (cold, sinusitis) |
| Improves with antihistamine | Yes | Unlikely |
| Both eyes watery | Yes (seasonal allergies) | Rarely |
| Triggered by specific foods | Yes (OAS, food allergy) | No |
| Improves when away from trigger | Yes | No |
| Requires prescription | Not usually (mild) | Yes (thrush, recurrent herpes) |
Home Remedies That Actually Help
If your itchy palate is mild and you have ruled out a serious allergy or infection, these home remedies offer safe, effective relief.
Saltwater rinse: Mix half a teaspoon of salt in 8 oz of warm water. Swish and gargle for 30 seconds and spit. Salt reduces inflammation, kills surface bacteria, and soothes irritated tissue. Repeat 2–3 times daily.
Stay hydrated: Sip water consistently throughout the day. Dehydration causes dry mucous membranes that feel itchy and scratchy. Aim for 8 glasses of water daily and more if you are in a dry environment.
Cool foods and drinks: Suck on ice chips, eat chilled yogurt, or sip cold water. Cool temperatures temporarily numb nerve endings in the palate and provide fast, short-term relief.
Honey: A small spoonful of raw honey (if you are not allergic) coats the palate and provides a natural anti-inflammatory, antimicrobial soothing effect. Do not give honey to children under one year of age.
Steam inhalation: Breathing steam from a bowl of hot water (cover your head with a towel) or a warm shower can open congested nasal passages, reduce post-nasal drip, and relieve palate itching related to sinus pressure or a cold.
Avoid known triggers: If specific raw foods, seasonal pollen, or household irritants consistently trigger your symptoms, avoid them as much as possible. Cook or peel fruits and vegetables if you have OAS. Keep windows closed during high pollen days.
Switch oral care products: If you recently started a new toothpaste or mouthwash and the itching appeared shortly after, try switching to a gentle, SLS-free, alcohol-free product for 1–2 weeks to see if symptoms improve.
Over-the-Counter Treatments for Itchy Roof of Mouth
| Treatment Type | Examples | Best For |
|---|---|---|
| Non-sedating antihistamine | Cetirizine (Zyrtec), fexofenadine (Allegra), loratadine (Claritin) | Seasonal allergies, OAS, mild food reactions |
| Sedating antihistamine | Diphenhydramine (Benadryl) | Acute allergic reactions, nighttime relief |
| Nasal corticosteroid spray | Fluticasone (Flonase), budesonide (Rhinocort) | Hay fever, sinusitis-related palate itch |
| Decongestant | Pseudoephedrine, oxymetazoline (Afrin) | Sinus congestion, post-nasal drip |
| Saline nasal spray | Simply Saline, NeilMed | Nasal rinsing, sinus relief |
| Topical antiviral (OTC) | Docosanol (Abreva) | Cold sores (applied at first tingle) |
| Oral analgesic gel | Benzocaine (Orajel) | Temporary numbing of irritated palate |
| Saliva substitute | Biotene mouthwash, Oasis dry mouth spray | Dry mouth / xerostomia |
When to See a Doctor Immediately
Most causes of an itchy roof of the mouth are not emergencies. But certain symptom combinations require prompt or immediate medical attention.
See a doctor urgently (same day) if:
The itching is severe and getting worse rapidly. You have difficulty swallowing or feel like something is blocking your throat. White patches or blisters appear in your mouth. The itching is accompanied by a fever over 101°F (38.3°C). You have had this symptom for more than 10–14 days without improvement. You are immunocompromised and develop any new oral symptoms.
Call 911 or go to an emergency room immediately if:
Your throat feels like it is closing or tightening. You have difficulty breathing. Your lips, tongue, or throat are swelling rapidly. You feel faint, dizzy, or your heart is racing. Your skin is turning pale, blue, or you feel you may lose consciousness. You have used an EpiPen and symptoms are not resolving. These are signs of anaphylaxis — a life-threatening allergic reaction that can be fatal without immediate epinephrine treatment.
Prevention — How to Stop Itchy Roof of Mouth from Recurring

Preventing recurring palate itching depends on knowing your triggers. These habits reduce risk across most causes.
Track your symptoms — keep a simple diary noting when itching occurs, what you ate beforehand, what the pollen count was, and what other symptoms appeared alongside it. Patterns will emerge within 1–2 weeks that help identify your specific trigger.
Start antihistamines 1–2 weeks before your allergy season begins rather than waiting for symptoms to appear. Pre-treatment is significantly more effective than reactive treatment.
Cook or microwave raw fruits and vegetables that trigger OAS reactions. Peeling foods also reduces cross-reactive protein exposure. Most people with OAS can eat the same foods without reaction when cooked.
Practice excellent oral hygiene — brush twice daily, floss once daily, rinse with a gentle mouthwash, and stay up to date on dental checkups. Good oral hygiene prevents thrush, reduces gum inflammation, and keeps oral tissues healthy.
Rinse your mouth with water and brush your teeth after using corticosteroid inhalers. This simple step dramatically reduces the risk of oral thrush.
Stay well hydrated throughout the day to maintain healthy saliva production and keep mucous membranes moist and resistant to irritation.
See an allergist if seasonal allergies or OAS are significantly affecting your quality of life. Immunotherapy can substantially reduce long-term sensitivity and prevent recurring symptoms.
Frequently Asked Questions (FAQs)
Q1. Why is the roof of my mouth itchy with no other symptoms?
An itchy palate with no other symptoms is most often caused by mild oral allergy syndrome after eating a raw fruit, vegetable, or nut. Dry mouth from dehydration or a toothpaste ingredient is also a common silent culprit.
Q2. Is an itchy roof of the mouth a sign of COVID-19?
An itchy palate alone is not a recognized hallmark symptom of COVID-19. However, COVID-19 can cause a range of oral symptoms including dry mouth, inflammation, and sometimes altered taste. If you have other COVID symptoms, get tested.
Q3. Why does the roof of my mouth itch only in spring and fall?
Itching that appears predictably each spring and fall is almost certainly caused by seasonal pollen allergies. Birch and tree pollen peak in spring; ragweed and weed pollen peak in late summer and fall. Start antihistamines before your season begins.
Q4. Can oral thrush cause an itchy palate?
Yes. Oral thrush caused by Candida albicans overgrowth causes itching, soreness, and a cottony feeling on the palate, tongue, and inner cheeks. White or yellowish patches are the hallmark sign. It requires prescription antifungal treatment to clear.
Q5. Why does eating certain fruits make the roof of my mouth itch?
This is classic oral allergy syndrome. Your immune system is confusing proteins in that raw fruit with pollen proteins from a pollen you are already allergic to. Try cooking or peeling the fruit — this usually eliminates the reaction entirely.
Q6. Can stress cause an itchy roof of the mouth?
Stress does not directly cause palate itching, but it can trigger cold sore outbreaks (HSV-1), worsen allergic symptoms, cause dry mouth, and suppress immune function. Managing stress reduces the frequency of stress-related triggers.
Q7. Is an itchy palate dangerous?
In most cases, no. Mild itching from allergies, OAS, a cold, or dry mouth is not dangerous. It becomes dangerous only if the throat swells, breathing becomes difficult, or the reaction progresses toward anaphylaxis — which requires emergency care.
Q8. How long should an itchy roof of the mouth last?
OAS-related itching resolves within 20–30 minutes. Allergy-related itching resolves within hours once the trigger is removed. Cold-related itching clears within 1–2 weeks. If itching persists beyond 2 weeks with no clear cause, see a doctor.
Q9. Can I use antihistamines to stop an itchy palate immediately?
Yes. Over-the-counter antihistamines like Benadryl work within 20–30 minutes for allergic reactions and OAS. Non-sedating options like Zyrtec or Allegra take slightly longer to act but do not cause drowsiness and are better for daytime use.
Q10. When should I see an allergist about itchy roof of the mouth?
See an allergist if symptoms occur regularly during pollen seasons, if multiple foods trigger reactions, if OAS symptoms are worsening, or if you have ever had a reaction severe enough to involve throat swelling or breathing difficulty. An allergist can confirm your specific triggers through testing and discuss long-term management including immunotherapy.
Conclusion
Why is the roof of my mouth itchy — in 2026, the answer points most often to seasonal allergies, oral allergy syndrome, or a mild infection, all of which are very manageable once correctly identified.
The key is recognizing the pattern of your symptoms. Does the itching appear at the same time of year? Does it follow eating specific raw foods? Does it come with white patches, blisters, or sinus pressure? Each pattern points to a different cause, and each cause has a specific and effective treatment.
Most cases of itchy palate resolve with simple interventions — antihistamines, saltwater rinses, hydration, trigger avoidance, and good oral hygiene. More persistent or severe cases may need prescription antifungals, antivirals, nasal steroids, or allergy immunotherapy.
The truly important thing to remember is that throat swelling, breathing difficulty, or rapid worsening of any oral allergic reaction is a medical emergency. Act immediately. For everything else, use the guidance in this article, track your symptoms, and speak with a doctor or allergist if things are not improving within two weeks. Relief is almost always possible once you find the right cause.