Why Do My Gums Suddenly Hurt? Signs & Solutions 2026

Why do my gums suddenly hurt is a question millions of people ask every year — and it almost always means your mouth is trying to tell you something. Gum pain can come on fast and without an obvious cause, leaving you wondering if it is something minor or something serious.
In most cases, sudden gum pain is caused by an infection, gum disease, a trapped food particle, or hormonal shifts. But sometimes it signals a dental abscess or other condition that needs prompt care.
What Your Gums Are Telling You
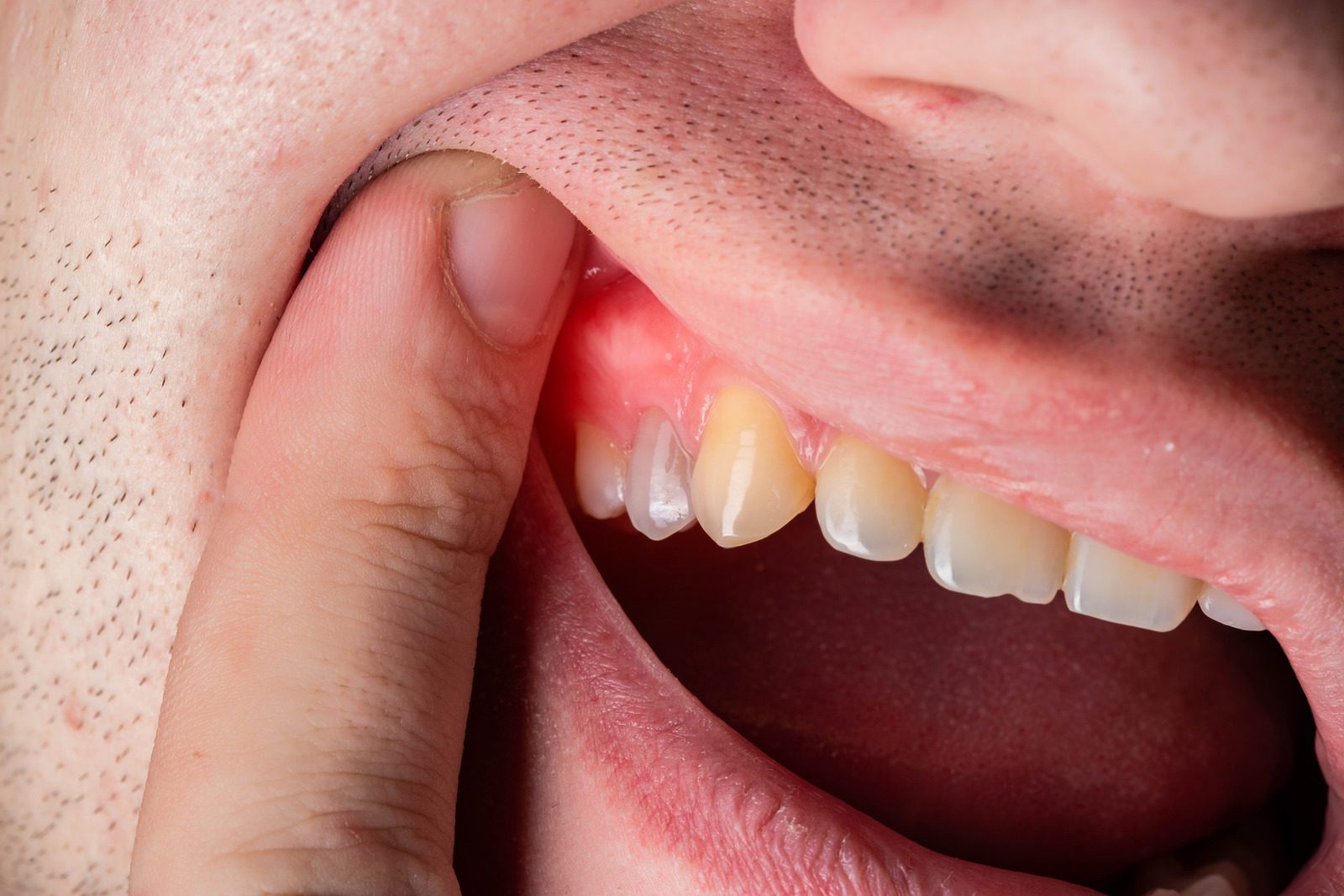
Healthy gums are firm, pale pink, and fit snugly around each tooth. They do not bleed, throb, or feel tender when you brush or eat.
When your gums suddenly hurt, it is your body flagging that something has disrupted that healthy state — whether from bacteria, physical trauma, hormones, or disease. The location, duration, and type of pain all give important clues about the cause.
Understanding those clues helps you decide whether to manage things at home or book a dental appointment right away.
Why Do My Gums Suddenly Hurt? Top Causes Explained
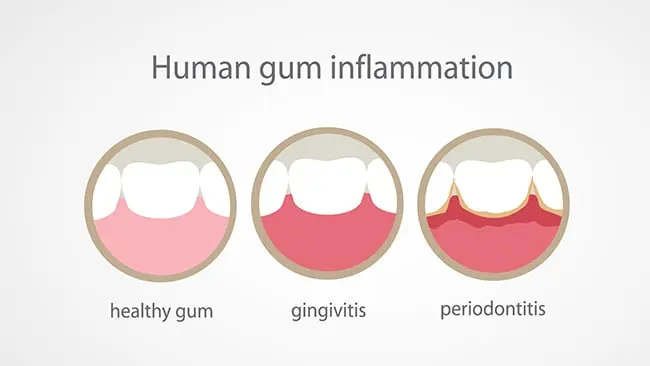
Gingivitis — The Most Common Culprit
Gingivitis is the earliest and most reversible stage of gum disease. It occurs when plaque — a sticky film of bacteria — builds up along the gumline and causes inflammation.
Symptoms include red, swollen, tender gums that bleed easily when you brush or floss. Many people first notice sudden gum soreness when the inflammation reaches a tipping point after days of plaque accumulation.
The good news is that gingivitis is fully reversible with proper brushing, flossing, and a professional dental cleaning. If left untreated, however, it progresses to a much more serious condition.
Periodontitis — Advanced Gum Disease
When gingivitis goes untreated, it advances into periodontitis. This is a destructive bacterial infection that damages the soft tissue, the connective fibers, and eventually the bone that holds teeth in place.
Periodontitis causes persistent, deep gum pain, significant bleeding, gum recession, loose teeth, and persistent bad breath. At this stage, home care alone is not enough — professional treatment is essential to stop further damage and tooth loss.
Approximately 2 in 5 adults have some form of gum disease, making it one of the most common reasons gums suddenly hurt.
Dental Abscess
A dental abscess is a pocket of pus caused by a bacterial infection at the root of a tooth or in the surrounding gum tissue. It produces intense, throbbing pain that can radiate to the jaw, ear, or neck.
The area around an abscessed tooth is often visibly swollen, warm, and tender. A small, pimple-like bump filled with pus may appear on the gum. This is a dental emergency — abscesses do not resolve on their own and require professional drainage and treatment.
If fever, facial swelling, or difficulty swallowing develops alongside gum pain, seek emergency dental or medical care immediately.
Pericoronitis — Wisdom Tooth Gum Pain
Pericoronitis is inflammation of the gum tissue around a partially erupted wisdom tooth. It is one of the most common causes of sudden gum pain in people aged 17–30.
When a wisdom tooth does not fully break through the gumline, a small flap of gum tissue called an operculum forms over it. Food particles and bacteria get trapped beneath this flap, leading to infection, significant pain, swelling, and sometimes a foul taste in the mouth.
Pericoronitis most commonly affects the lower back molars. It can progress quickly from a mild ache to severe pain with jaw stiffness, swollen lymph nodes, and difficulty swallowing if not treated promptly.
Trapped Food or Debris Under the Gumline
One of the most overlooked causes of sudden gum pain is a piece of food lodged between a tooth and the gum. A popcorn kernel skin, nut fragment, seed, or meat fiber can wedge under the gumline and immediately cause localized pain, swelling, and irritation.
This type of pain appears very suddenly — often right after eating — and is usually focused in one specific spot. Rinsing with warm salt water and gently flossing the area often resolves it quickly.
If the trapped debris is not removed, the gum tissue can become infected over the following hours or days.
Aggressive Brushing or Incorrect Flossing
Using a hard-bristled toothbrush or scrubbing your teeth too vigorously is a very common cause of sudden and recurring gum soreness. This physically damages and abrades the delicate gum tissue.
Snapping floss forcefully down into the gumline instead of gently guiding it in a C-shape can also cut and bruise gum tissue. Both habits cause immediate soreness and, over time, contribute to gum recession.
Switching to a soft-bristled toothbrush and using gentle circular motions usually resolves brushing-related gum pain within a few days.
Hormonal Changes
Hormonal fluctuations are a well-established trigger for sudden gum pain, particularly in women. Rising or shifting levels of estrogen and progesterone increase blood flow to the gums, making them hypersensitive, swollen, and prone to inflammation.
Common hormonal triggers for gum pain include:
- Menstruation — gum tenderness often peaks a few days before a period
- Pregnancy — “pregnancy gingivitis” affects up to 70% of pregnant women
- Puberty — teenagers frequently experience inflamed, easily bleeding gums
- Menopause — falling estrogen levels can cause dry mouth, burning gums, and increased sensitivity
Hormone-driven gum pain typically improves on its own as hormone levels stabilize, but good oral hygiene during these periods is critical to prevent secondary infection.
Canker Sores (Aphthous Ulcers)
Canker sores are small, painful ulcers that develop on the soft tissues inside the mouth, including the gums. They appear as white or yellowish spots with a red border and can cause intense, localized stinging — especially when eating, drinking, or brushing.
They are not contagious and are triggered by stress, minor mouth injuries, acidic foods, vitamin deficiencies, or immune system fluctuations. Most canker sores heal on their own within 7–14 days.
Ill-Fitting Dental Appliances
Braces, retainers, dentures, mouthguards, and aligners that do not fit properly can continuously rub against gum tissue. This friction causes irritation, soreness, and sometimes ulcers in the specific spots that are being rubbed.
Pain from dental appliances tends to be localized to the exact points of contact. Adjusting or relining the appliance with professional help usually resolves the issue.
Vitamin Deficiencies
A deficiency in Vitamin C — a condition historically known as scurvy — causes the gum tissue to weaken, swell, bleed easily, and become painful. Vitamin C is essential for producing collagen, which gives gum tissue its strength and integrity.
Deficiencies in B vitamins (particularly B12 and folate) and Vitamin K can also contribute to gum inflammation and bleeding. A diet lacking in fresh fruits, vegetables, and balanced nutrition significantly increases this risk.
Oral Infections — Thrush and Herpes
Oral thrush is a fungal infection (Candida overgrowth) that causes a white coating on the tongue and inner cheeks, along with gum soreness. It commonly affects people who have recently taken antibiotics, use steroid inhalers, or have weakened immune systems.
Herpes simplex virus (HSV-1) can cause painful blisters or sores on the gums and around the mouth during outbreaks. These viral sores tend to appear suddenly and are concentrated in clusters. Both conditions require specific medical or dental treatment.
Stress and Immune System Suppression
Chronic stress raises cortisol levels throughout the body, which suppresses immune function and promotes inflammation — including in the gums. People going through periods of high stress frequently notice that their gums become more sore, inflamed, and prone to bleeding.
Stress also drives habits like teeth grinding (bruxism) and jaw clenching, both of which place excess pressure on gum tissue and cause soreness.
Tobacco Use
Smoking and chewing tobacco are major irritants to gum tissue. Tobacco chemicals directly damage the cells lining the gums, impair blood flow to the area, and suppress the immune response needed to fight oral infections.
Tobacco users are significantly more likely to develop gum disease, slower gum healing, and persistent gum pain. Gum disease in smokers is often more severe and harder to treat than in non-smokers.
Recent Dental Work
It is completely normal to experience tender, sore gums for 2–3 days after dental procedures including cleanings, fillings, extractions, crown placements, or scaling. The tissues need time to recover from the instruments used during treatment.
If gum pain after a dental procedure worsens after 3 days, does not improve after a week, or comes with swelling or a bad taste, contact your dentist — it may indicate a post-procedure infection.
Common Causes of Sudden Gum Pain at a Glance
| Cause | Pain Type | Location | Duration |
|---|---|---|---|
| Gingivitis | Dull ache, tenderness | Along entire gumline | Persistent if untreated |
| Periodontitis | Deep, throbbing | Multiple teeth | Ongoing, worsening |
| Dental Abscess | Severe, throbbing | One tooth or area | Worsens without treatment |
| Pericoronitis | Sharp, intense | Back of mouth (wisdom teeth) | Days to weeks |
| Trapped Food | Sharp, localized | One spot | Resolves when removed |
| Aggressive Brushing | Soreness, tenderness | Along gumline | Clears in days |
| Hormonal Changes | Generalized sensitivity | Widespread | Temporary |
| Canker Sore | Stinging, burning | One spot on gum | 7–14 days |
| Vitamin Deficiency | Aching, bleeding | Generalized | Until deficiency corrected |
Warning Signs That Demand Immediate Dental Attention
Not all gum pain needs urgent care. But certain symptoms signal that waiting is not safe.
See a dentist as soon as possible if you experience:
Gum pain that does not improve within 48 hours of home care. A visible pus-filled bump or abscess on the gum. Significant facial swelling, especially around the jaw or under the eye. Fever above 38°C (100.4°F) alongside gum pain. Difficulty swallowing or breathing. Loose teeth or visible gum recession appearing suddenly. Persistent bad taste or odor in the mouth that does not go away. Gum pain alongside jaw stiffness or locked jaw. Bleeding that does not stop with gentle pressure.
These symptoms may indicate a spreading dental infection or an abscess that can become life-threatening if it travels to the neck or throat.
Sudden Gum Pain in One Spot vs. All Over
The location of your gum pain provides important diagnostic clues:
Gum pain in one spot usually points to a localized cause — a trapped food particle, an abscess, a canker sore, pericoronitis around a specific tooth, or trauma from a sharp food item or dental appliance.
Gum pain all over or along the entire gumline more commonly signals gingivitis, periodontitis, a vitamin deficiency, hormonal changes, or aggressive brushing that affects the whole mouth.
If the one-spot pain is accompanied by visible swelling, a bad taste, or a lump on the gum, it almost certainly points to an infection that requires professional evaluation.
How to Relieve Sudden Gum Pain at Home
Most mild to moderate gum pain can be safely managed at home while you monitor whether the situation improves.
Warm Salt Water Rinse
A warm salt water rinse is the most universally effective and evidence-backed home remedy for sudden gum pain. Salt is a natural antibacterial agent that reduces inflammation, soothes irritated tissue, and helps flush bacteria and debris from around the gumline.
Mix half a teaspoon of table salt in a glass of warm (not hot) water. Swish gently for 30 seconds and spit. Repeat 3–4 times daily, especially after meals. Do not swallow the rinse.
Cold Compress
Applying a cold compress or ice pack wrapped in a clean cloth to the outside of the cheek over the sore area reduces swelling, numbs the pain, and decreases blood flow to inflamed tissue.
Apply for 10–15 minutes at a time, take a 10-minute break, and repeat as needed. This is especially helpful for abscess-related swelling and pericoronitis pain. Never apply ice directly to the skin.
OTC Pain Relievers
Over-the-counter anti-inflammatory medications reduce both pain and gum inflammation. Ibuprofen (Advil, Motrin) is particularly effective because it targets inflammation at the source. Acetaminophen (Tylenol) relieves pain without anti-inflammatory action.
Follow the label dosing instructions carefully. If you have stomach issues, kidney disease, or are pregnant, check with a healthcare provider before taking NSAIDs like ibuprofen.
Topical Benzocaine Gel
Over-the-counter topical oral anesthetic gels containing benzocaine (such as Orajel or Anbesol) can be applied directly to the sore gum area to provide fast, localized numbing relief.
These are effective for canker sore pain, post-dental procedure soreness, and mild localized gum irritation. Use sparingly and only as directed on the label. Do not use in children under 2 years old.
Clove Oil
Clove oil contains eugenol, a natural compound with proven anesthetic and antibacterial properties. Dipping a cotton ball in diluted clove oil and gently pressing it against the sore gum area provides temporary numbing relief.
Always dilute clove oil in a carrier oil (like olive or coconut oil) at a 1:10 ratio before applying to gum tissue. Undiluted clove oil can burn the mucosa.
Antimicrobial Mouthwash
Using an alcohol-free antiseptic mouthwash containing chlorhexidine or cetylpyridinium chloride helps kill bacteria in the mouth that are contributing to gum inflammation and pain.
Chlorhexidine mouthwash is particularly effective for gingivitis and post-procedure gum care, though it may stain teeth with prolonged use. Use it twice daily after brushing for short-term relief.
Improve Your Brushing Technique
Switch immediately to a soft-bristled toothbrush if you have been using a medium or hard one. Use gentle, small circular motions aimed at a 45-degree angle toward the gumline.
Never saw back and forth horizontally across the gumline. Use light pressure — let the bristles do the work. Proper brushing technique resolves a significant proportion of recurring gum soreness.
Eat a Soft Food Diet
While your gums are healing, avoid crunchy, sharp, acidic, spicy, or hard foods that can aggravate inflamed tissue. Chips, crackers, popcorn, nuts, citrus, and raw vegetables are common irritants.
Stick to soft foods like yogurt, oatmeal, scrambled eggs, soft pasta, mashed potatoes, soup, and smoothies. Soft eating prevents further trauma to already-sensitized gum tissue.
Stay Well Hydrated
Drinking plenty of water throughout the day keeps the mouth moist, flushes bacteria away from the gumline, and prevents the dry conditions in which oral bacteria thrive.
Dehydration reduces saliva production. Saliva is a natural antibacterial agent, so keeping it flowing by staying hydrated is a simple but important strategy for gum health.
Professional Treatments for Gum Pain

When home care is not enough or the cause is more serious, dentists have several targeted treatments available:
Professional Dental Cleaning (Prophylaxis)
A routine professional cleaning removes plaque and tartar (calcified plaque) that cannot be removed by brushing alone. For gingivitis-related gum pain, this is often the single most effective treatment and produces rapid improvement.
Cleanings are recommended twice yearly for most people and more frequently for those with active gum disease.
Scaling and Root Planing
Scaling and root planing is a deep-cleaning procedure used for periodontitis. A dental hygienist uses specialized instruments to clean beneath the gumline — removing bacteria, plaque, and tartar from the root surfaces.
This procedure disrupts the bacterial colonies that are driving the infection and allows the gum tissue to heal and reattach to the tooth. It may require local anesthesia and multiple appointments.
Antibiotic Therapy
For bacterial gum infections, abscesses, and pericoronitis, dentists may prescribe oral antibiotics such as amoxicillin, metronidazole, or doxycycline to clear the infection from the inside.
Topical antibiotic gels are also sometimes placed directly into gum pockets after scaling and root planing to target bacteria more precisely.
Abscess Drainage
A dental abscess requires professional drainage to remove the pus. The dentist numbs the area, makes a small incision, and flushes out the infection. This provides immediate, significant pain relief.
A root canal or tooth extraction may follow, depending on the condition of the affected tooth. Antibiotics are typically prescribed alongside drainage.
Gum Surgery
In advanced periodontitis, surgical procedures like flap surgery or gum grafting may be necessary. Flap surgery lifts back the gum tissue to allow deep cleaning of root surfaces. Gum grafts replace lost tissue in areas of significant recession.
These procedures are performed by a periodontist — a dental specialist focused on gum disease treatment — and significantly reduce long-term gum pain and tooth loss risk.
Wisdom Tooth Extraction
For recurrent or severe pericoronitis, extraction of the problematic wisdom tooth is the most definitive and permanent solution. Removing the tooth eliminates the pocket where food and bacteria accumulate.
In some cases, the overlying gum flap (operculum) can be surgically removed to expose the tooth without extraction, though the flap can regrow in some patients.
Gum Pain Prevention: Long-Term Strategies
| Prevention Strategy | How It Helps | Frequency |
|---|---|---|
| Brush with soft-bristled toothbrush | Removes plaque without damaging gum tissue | Twice daily |
| Floss properly | Clears bacteria between teeth and at gumline | Once daily |
| Use antimicrobial mouthwash | Reduces oral bacteria load | Once daily |
| Professional dental cleaning | Removes tartar that brushing can’t reach | Every 6 months |
| Drink plenty of water | Maintains saliva production, flushes bacteria | 8 glasses daily |
| Eat a balanced diet | Provides Vitamin C, calcium, B vitamins for gum health | Daily |
| Quit smoking | Restores blood flow and immune response to gums | Immediately |
| Manage stress | Lowers cortisol-driven gum inflammation | Ongoing |
| Wear a nightguard if you grind | Reduces pressure on gum tissue during sleep | Nightly |
Gum Pain in Special Populations

Gum Pain During Pregnancy
Pregnancy gingivitis is extremely common and typically peaks in the second trimester. Rising progesterone levels make gum tissue hypersensitive and more reactive to the bacteria in plaque.
Pregnant women should maintain meticulous oral hygiene and continue seeing their dentist for regular cleanings throughout pregnancy. Untreated gum disease during pregnancy has been linked to preterm birth and low birth weight in some studies.
Gum Pain in Children and Teenagers
Children teething, losing baby teeth, or erupting adult teeth commonly experience gum tenderness in the affected areas. Teenagers undergoing puberty frequently develop gingivitis due to hormonal changes.
Children with braces are at significantly higher risk of gingivitis because food and plaque accumulate around brackets and wires. Extra diligence with brushing, water flossers, and regular cleanings is essential.
Gum Pain in Older Adults
Older adults are at higher risk for periodontitis, gum recession, and dry mouth — all of which cause gum pain. Many medications commonly prescribed to older adults (including blood pressure drugs, antidepressants, and antihistamines) reduce saliva flow, increasing gum vulnerability.
Regular dental visits and proactive management of dry mouth are especially important for gum health in older adults.
Frequently Asked Questions (FAQs)
Why do my gums suddenly hurt for no reason?
Sudden gum pain without an obvious cause is often linked to trapped food debris, the early stages of gingivitis, hormonal changes, or a developing infection. If it lasts more than 48 hours, see a dentist to rule out an abscess or gum disease.
Can stress cause sudden gum pain?
Yes. Elevated cortisol from chronic stress suppresses the immune system and promotes inflammation throughout the body, including the gums. Stress also drives teeth grinding, which places excess pressure on gum tissue and causes soreness.
Why do my gums hurt in one spot only?
Localized gum pain in one spot typically points to a trapped food particle, an abscess, a canker sore, pericoronitis around a wisdom tooth, or a minor gum injury. If the spot is swollen, has a bad taste, or does not improve in 2 days, see a dentist.
How long should gum pain last?
Minor gum pain from irritation or a canker sore typically resolves within 7–14 days with basic home care. Pain from an abscess or periodontitis will worsen without treatment. Pain lasting more than a week without improvement needs professional evaluation.
Is sudden gum pain a sign of infection?
It can be. Sudden, intense, throbbing gum pain — especially with swelling, pus, a bad taste, or fever — strongly suggests a dental abscess or pericoronitis, both of which are infections requiring prompt dental treatment.
Can gum pain go away on its own?
Minor gum pain from brushing trauma, a canker sore, or temporary hormonal sensitivity can resolve on its own. Pain from infection, abscess, or periodontitis will not go away without treatment and will worsen if ignored.
What is the fastest home remedy for gum pain?
A warm salt water rinse provides rapid relief by reducing inflammation and killing surface bacteria. Applying a cold compress to the cheek and taking ibuprofen together give the fastest combined relief for swelling and pain.
Why do my gums hurt after eating?
Gum pain after eating is often caused by a sharp food item (chip, cracker, or nut) injuring the gum tissue, food trapped under the gumline, acid from certain foods irritating inflamed gums, or pain from an abscess aggravated by chewing.
Can vitamin deficiency cause sudden gum pain?
Yes. A deficiency in Vitamin C weakens gum tissue, causing it to swell, bleed, and become painful. Low levels of Vitamin B12, folate, and Vitamin K can also contribute to gum sensitivity and increased bleeding.
When should I go to the ER for gum pain?
Go to the emergency room if gum pain is accompanied by significant facial or neck swelling, fever, difficulty swallowing, difficulty breathing, or signs that an infection is spreading. These symptoms indicate a potentially life-threatening dental abscess.
Conclusion
Why do my gums suddenly hurt almost always has a clear answer — and most causes are very treatable when caught early. Whether the trigger is plaque buildup triggering gingivitis, a trapped seed causing localized irritation, a wisdom tooth flare-up, or a hormonal surge making your gums hypersensitive, the right response depends on reading your symptoms carefully.
Start with salt water rinses, a soft-bristled toothbrush, and OTC pain relief. Monitor the pain closely over 48 hours. If it worsens, spreads, comes with swelling, or does not improve within a week, book a dental appointment promptly.
Left untreated, gum infections and disease escalate quickly — but caught early, they are almost entirely reversible. Good oral hygiene, regular dental cleanings, and healthy habits are your best long-term defense against gum pain ever striking again.