Why Does My Gum Hurt? Causes, Symptoms & Treatment 2026

Why does my gum hurt is a question millions of people ask every year, and the answer is not always simple. Gum pain can range from a mild irritation to a sharp, throbbing ache that makes eating, brushing, and even speaking uncomfortable. Sometimes it clears up on its own.
Other times it signals a deeper dental or health problem that needs professional attention. Understanding what is behind your gum pain is the first step toward finding the right relief.
What Does Gum Pain Feel Like?

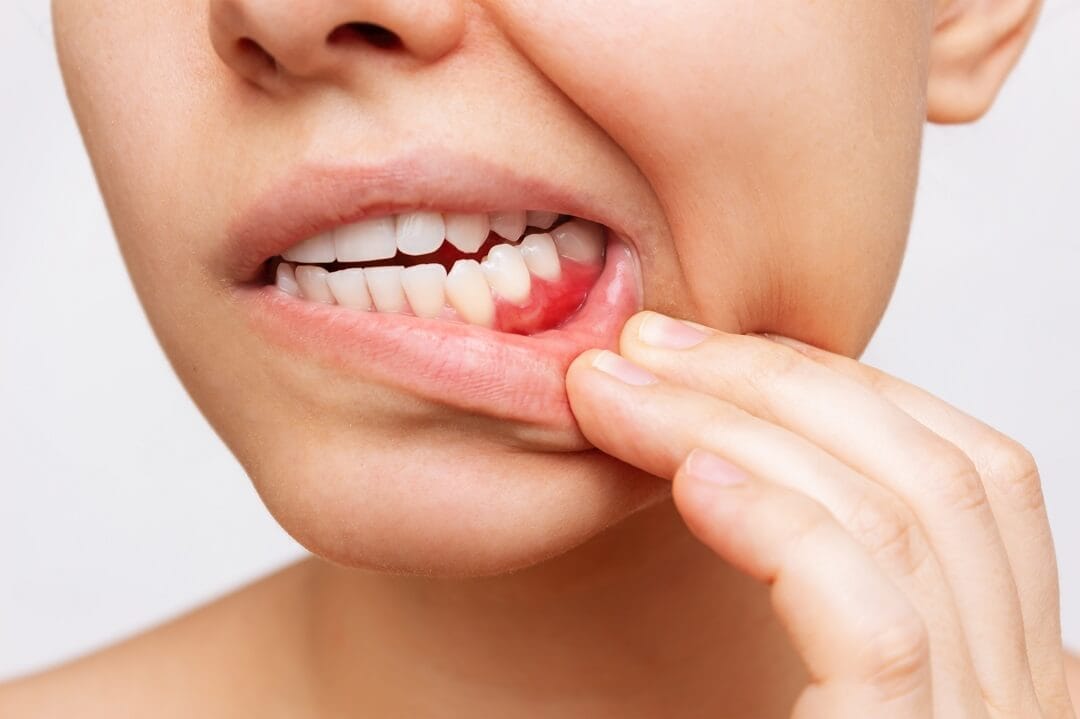
Gum pain presents differently depending on the cause. It can feel like a dull ache, a sharp sting, a throbbing sensation, or a burning discomfort along the gumline.
You might notice pain in one specific spot, across multiple teeth, or all along the upper or lower gum. Some people experience pain only when chewing, brushing, or touching the area.
Other times the gum pain is constant and does not go away no matter what you do.
Why Does My Gum Hurt? 14 Most Common Causes
1. Gingivitis (Early Gum Disease)
Gingivitis is the most common cause of gum pain and the earliest stage of gum disease. It occurs when plaque, a sticky film of bacteria, builds up along the gumline and triggers inflammation.
Symptoms include red, swollen, and tender gums that bleed easily when you brush or floss. The good news is gingivitis is reversible with proper oral hygiene and professional cleaning.
About 2 in 5 adults have some form of gum disease, making gingivitis one of the most widespread dental conditions in the world.
2. Periodontitis (Advanced Gum Disease)
When gingivitis is left untreated, it progresses into periodontitis, a more serious infection that attacks the connective tissue and bone supporting your teeth.
Symptoms include persistent gum pain, receding gums, loose teeth, visible tooth roots, bad breath, and in severe cases, tooth loss. At this stage, professional periodontal treatment is essential.
Periodontitis has also been linked to heart disease, respiratory conditions, diabetes, and certain cancers, making it far more than just a dental problem.
3. Tooth Abscess
A tooth abscess is a pocket of pus caused by a bacterial infection inside or around a tooth. It can form at the tip of the tooth root (periapical abscess), in the gum tissue (periodontal abscess), or around a partially erupted tooth (pericoronal abscess).
Symptoms include severe throbbing pain that may radiate to the jaw, neck, or ear, along with swelling, fever, and a bad taste in the mouth. Left untreated, an abscess can spread to the jaw, face, neck, and in rare cases, the bloodstream causing a life-threatening infection called sepsis.
If you suspect an abscess, see a dentist immediately. This is not something to manage at home long-term.
4. Brushing Too Hard
Brushing with too much pressure or using a hard-bristled toothbrush can damage delicate gum tissue and cause soreness, irritation, and bleeding. Over time, aggressive brushing leads to gum recession.
Gum recession exposes the sensitive roots of your teeth, which causes ongoing sensitivity and pain that worsens without intervention.
Switch to a soft-bristled toothbrush and use gentle, circular motions. Electric toothbrushes with pressure sensors can also help you avoid applying too much force.
5. Canker Sores (Mouth Ulcers)
Canker sores are small, painful ulcers that can appear directly on the gum tissue. They are usually round or oval with a white or yellow center and a red border.
They are triggered by stress, minor mouth injuries, acidic foods, hormonal changes, or an impaired immune system. Most heal on their own within one to two weeks without treatment.
While canker sores are not contagious or dangerous, they can make eating, talking, and brushing very uncomfortable while they are present.
6. Hormonal Changes
Hormonal fluctuations during puberty, menstruation, pregnancy, and menopause significantly affect gum sensitivity. During these periods, more blood flows to the gums and they become more reactive to bacteria and plaque.
Pregnancy gingivitis is especially common, with many expectant mothers experiencing swollen, tender, and bleeding gums throughout pregnancy due to rising hormone levels.
During menopause, gums may burn, change color, bleed, or hurt as estrogen levels drop. Speaking with your doctor and dentist together is the best approach during hormonal transitions.
7. Wisdom Teeth Eruption
When wisdom teeth (third molars) begin to emerge, they can push through the gum tissue and cause significant localized pain, swelling, and redness in the back of the mouth.
Impacted wisdom teeth, those that cannot fully emerge and become stuck beneath the gum, are especially painful. They create pockets of gum tissue where bacteria can accumulate and cause infection.
Pain from wisdom teeth typically occurs between the ages of 17 and 25 but can happen later. A dental X-ray can confirm whether your wisdom teeth are the source of pain.
8. Food Particles Trapped Under the Gumline
Small pieces of food such as popcorn kernels, seeds, or hard shells can become trapped between the tooth and the gum. This creates intense localized pressure and irritation that can feel similar to an abscess.
The trapped debris causes bacteria to multiply rapidly in the area, leading to swelling, tenderness, and sometimes infection if not cleared promptly.
Thorough flossing and an antiseptic rinse can often dislodge the particle and relieve the pain.
9. Ill-Fitting Dental Appliances
Braces, retainers, dentures, or ill-fitting crowns and bridges can rub against gum tissue and cause chronic soreness, irritation, and inflammation.
Dentures that no longer fit properly are a common culprit, especially in older adults. Even a small misalignment creates constant friction that breaks down gum tissue over time.
If a dental appliance is causing pain, visit your dentist or orthodontist for an adjustment rather than continuing to tolerate the discomfort.
10. Sinusitis and Sinus Pressure
The roots of the upper back teeth sit very close to the sinus cavities. When the sinuses become inflamed or infected, the resulting pressure can cause pain that feels like it is coming from the upper gums and teeth.
This is why people with sinus infections often think they have a toothache or gum problem when the actual issue is sinus-related.
Once the sinus infection clears, the gum and tooth pain typically resolves as well.
11. Vitamin Deficiencies
A lack of Vitamin C is directly linked to swollen, bleeding, and painful gums. In severe cases, Vitamin C deficiency leads to scurvy, a condition characterized by extremely inflamed and deteriorating gum tissue.
Low levels of Vitamin D and Vitamin B12 are also associated with increased gum inflammation and slower healing of oral tissues.
Adding more citrus fruits, leafy greens, and vegetables to your diet, or taking a daily multivitamin, can make a noticeable difference in gum health.
12. Smoking and Tobacco Use
Cigarette smoking and smokeless tobacco are major risk factors for gum disease and gum pain. Tobacco reduces blood flow to the gums, weakens the immune response, and creates an environment where harmful bacteria thrive.
Smokeless tobacco is particularly damaging because it sits directly against gum tissue for extended periods, causing sores, gum recession, and a significantly elevated risk of oral cancer.
Smokers are at a much higher risk of developing severe gum disease than non-smokers, and their gum disease tends to progress faster and respond more poorly to treatment.
13. Medications and Drug Side Effects
Certain medications list gum pain, gum overgrowth, or increased gum bleeding as side effects. Blood thinners, anti-seizure drugs, and some calcium channel blockers (used for blood pressure) are among the most common offenders.
Dry mouth, a side effect of many medications including antihistamines and antidepressants, also contributes to gum inflammation because saliva plays a key role in keeping bacteria in check.
Always inform your dentist of all medications you are currently taking so they can factor this into their diagnosis and treatment plan.
14. Gum Recession
Gum recession occurs when the gum tissue gradually pulls away from the teeth, exposing the sensitive root surfaces. It is caused by aggressive brushing, gum disease, genetics, or teeth grinding.
Exposed roots are more sensitive to temperature, pressure, and acids. This sensitivity is often felt as a sharp pain that flares during eating, drinking hot or cold liquids, or brushing.
Treatment ranges from improving oral hygiene habits and using desensitizing toothpaste to surgical gum grafts in more advanced cases.
Gum Pain Symptoms: What to Watch For
Knowing which symptoms accompany your gum pain helps determine how urgent the situation is.
| Symptom | Possible Cause |
|---|---|
| Red, swollen gums that bleed when brushing | Gingivitis or early gum disease |
| Throbbing pain in one spot with swelling | Tooth abscess |
| Pain at back of mouth, difficulty opening jaw | Wisdom tooth eruption or impaction |
| Burning or sore gums with white ulcer | Canker sore |
| Gum pain with fever and facial swelling | Dental abscess requiring urgent care |
| Receding gums with root sensitivity | Gum recession |
| Bleeding gums, loose teeth, bad breath | Periodontitis (advanced gum disease) |
| Upper gum pain with sinus pressure | Sinusitis |
| Painful gums after starting a new medication | Drug side effect |
| Swollen, tender gums during pregnancy | Pregnancy gingivitis |
Gum Pain in One Specific Spot
Sometimes gum pain is isolated to one exact area rather than the whole mouth. This is often more telling than widespread gum soreness.
Pain in one spot on the upper gum could indicate a periapical abscess above an upper tooth, a sinus issue, or a trapped piece of food.
Pain in one spot on the lower gum may signal an abscess, a partially erupted wisdom tooth, a misaligned tooth, or a localized injury or trauma.
If the pain persists in one spot for more than three days, does not improve with home care, or is accompanied by swelling, pus, or fever, see a dentist promptly.
Gum Pain Stages: From Mild to Severe
| Severity Level | Symptoms | What to Do |
|---|---|---|
| Mild | Slight tenderness, occasional bleeding when brushing | Improve oral hygiene, use warm salt water rinse |
| Moderate | Swelling, persistent soreness, frequent bleeding | Book a dental appointment within a week |
| Severe | Throbbing pain, abscess, fever, difficulty eating | See a dentist urgently within 24–48 hours |
| Emergency | Facial swelling, difficulty swallowing or breathing | Go to emergency dental care immediately |
Home Remedies for Gum Pain Relief
These remedies can ease discomfort while you wait for a dental appointment. They are not cures but provide meaningful temporary relief.
Warm Salt Water Rinse
Dissolve one teaspoon of table salt in a cup of warm water. Swish thoroughly around your mouth for 30 to 60 seconds and spit. Repeat two to three times daily.
Salt water has natural antimicrobial properties and helps reduce inflammation. It is one of the most effective and accessible gum pain remedies available.
Do not use hot water as it can worsen irritation, and do not swallow the solution.
Cold Compress
Apply an ice pack or a cloth-wrapped bag of frozen peas to the outside of your cheek for 10 to 15 minutes. This helps reduce swelling and numbs the area temporarily.
Cold compression is especially helpful for abscess-related swelling or wisdom tooth pain. Use it in intervals throughout the day for best results.
Never apply ice directly to the skin or gum tissue.
Clove Oil
Clove oil contains eugenol, a natural compound with powerful numbing and antimicrobial properties. Apply a small amount to a cotton ball and press gently against the painful gum area.
If your gums are sensitive, dilute the clove oil with a carrier oil such as coconut oil before applying to avoid further irritation.
Clove oil provides fast but temporary relief and should not replace professional dental treatment.
Hydrogen Peroxide Rinse
Mix one part 3% hydrogen peroxide with two parts water and swish around the mouth for about 30 seconds before spitting. This can help reduce bacterial load and ease inflammation.
Hydrogen peroxide rinses have been shown to reduce plaque, decrease bleeding gums, and fight oral bacteria. Use it no more than twice daily.
Never swallow hydrogen peroxide solution and do not use concentrations higher than 3%.
Over-the-Counter Pain Relievers
Non-steroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen or acetaminophen can reduce both pain and inflammation in the short term.
Take as directed on the packaging and do not exceed the recommended dose. These medications treat symptoms but do not address the underlying cause of gum pain.
If you are on other medications or have existing health conditions, check with your pharmacist or doctor before taking pain relievers.
Aloe Vera Gel
Food-grade aloe vera gel applied directly to sore gum tissue can soothe irritation and provide anti-inflammatory relief. It is especially helpful for canker sores and inflamed gum tissue.
Keeping the gel refrigerated and applying it cold can amplify the soothing effect. Leave it on for a few minutes before rinsing.
Only use food-safe aloe vera gel intended for oral use.
Professional Dental Treatments for Gum Pain
When home remedies are not enough, these are the professional treatments your dentist may recommend.
| Treatment | Best For |
|---|---|
| Professional cleaning (scale and polish) | Gingivitis and early gum disease |
| Deep cleaning (scaling and root planing) | Periodontitis and moderate gum disease |
| Antibiotics (oral or local) | Bacterial infections, abscesses |
| Root canal therapy | Periapical abscess and infected tooth pulp |
| Tooth extraction | Severely impacted wisdom teeth, unsalvageable teeth |
| Gum surgery (flap surgery) | Advanced periodontitis |
| Bone and tissue grafting | Bone loss or significant gum recession |
| Abscess drainage | Draining pus from a dental abscess |
When to See a Dentist Urgently
Some gum pain symptoms require same-day or emergency dental care. Do not wait and hope these resolve on their own.
See a dentist immediately if you experience any of the following:
- A visible swollen lump or bump on the gum that looks like a pimple or boil
- Facial or neck swelling alongside gum pain
- Fever above 38°C (100.4°F) combined with dental pain
- Difficulty swallowing, breathing, or opening your mouth
- Gum pain that has lasted more than one week without improvement
- Pus or a bad taste draining from the gum
- Gum pain after a recent dental procedure that is getting worse instead of better
Gum Disease and Its Link to Overall Health

Gum pain is not just a dental issue. Research has consistently linked gum disease to serious systemic health conditions.
| Systemic Condition | How It Connects to Gum Disease |
|---|---|
| Heart disease | Oral bacteria can enter the bloodstream and contribute to arterial inflammation |
| Type 2 diabetes | Gum disease worsens blood sugar control and vice versa |
| Respiratory disease | Oral bacteria inhaled into the lungs can trigger or worsen lung infections |
| Alzheimer’s disease | Some research links chronic gum infection to increased dementia risk |
| Pregnancy complications | Periodontitis has been associated with premature birth and low birth weight |
| Rheumatoid arthritis | Shares similar inflammatory mechanisms with periodontal disease |
This makes treating gum pain promptly not just about oral comfort but about protecting your whole body.
How to Prevent Gum Pain
Prevention is far easier and less expensive than treatment. These daily habits keep your gums healthy and pain-free.
Daily Oral Hygiene Routine
Brush your teeth twice a day using a soft-bristled toothbrush and fluoride toothpaste. Use gentle circular motions rather than aggressive back-and-forth scrubbing.
Floss at least once a day to remove food particles and plaque from between teeth and below the gumline where a toothbrush cannot reach.
Use an antibacterial or antiseptic mouthwash daily to kill bacteria that brushing and flossing miss.
Diet and Nutrition
Limit sugary foods and drinks that feed the bacteria responsible for plaque and gum disease. Drink plenty of water to support saliva production, which naturally protects your gums.
Eat a diet rich in Vitamin C (citrus fruits, bell peppers, strawberries), Vitamin D (fatty fish, eggs), and calcium (dairy products, leafy greens) to support gum tissue health.
Avoid smoking and limit alcohol consumption, both of which dry out oral tissues and promote bacterial growth.
Regular Dental Checkups
Visit your dentist every six months for a professional cleaning and examination. Even with excellent home care, tartar (hardened plaque) can only be removed by professional tools.
Your dentist can spot early signs of gingivitis, cavities, or other problems before they develop into painful, expensive issues.
Early treatment always leads to better outcomes and less time in the dental chair.
Gum Pain vs. Tooth Pain: How to Tell the Difference
It is not always easy to determine whether your pain is coming from the gum or the tooth itself. Here is a quick guide.
| Pain Type | Gum Pain | Tooth Pain |
|---|---|---|
| Location | Along or on the gum tissue | Deep inside the tooth or root |
| Triggered by | Touching, brushing, flossing gumline | Hot, cold, sweet, or pressure |
| Appearance | Redness, swelling, or sores on gum | May see decay, crack, or no visible sign |
| Bleeding | Common with gum pain | Less common unless gum is also involved |
| Relief from rinses | Often helps | Less effective on its own |
If you are unsure, a dentist can quickly pinpoint the source with a clinical exam and X-rays.
Gum Pain After Dental Work
It is normal to experience some gum soreness after dental procedures including fillings, cleanings, extractions, and root canals. This usually resolves within two to three days.
If gum pain after a dental procedure is getting worse rather than better, lasting longer than a week, or accompanied by swelling or fever, contact your dentist immediately as this may indicate infection.
Never ignore worsening pain after dental work. Your dentist needs to know so they can intervene before a minor complication becomes a major problem.
Frequently Asked Questions (FAQs)
Why does my gum hurt in one spot only?
Localized gum pain is often caused by a trapped food particle, an abscess, a canker sore, or a partially erupted wisdom tooth. See a dentist if it persists beyond three days.
Can stress cause gum pain?
Yes, indirectly. Stress weakens the immune system and can trigger canker sores, lead to teeth grinding, and cause poor oral hygiene habits that all contribute to gum pain.
Why do my gums hurt when I brush?
Gums that hurt during brushing are usually inflamed from gingivitis, damaged by aggressive brushing technique, or reacting to a hard-bristled toothbrush. Switch to soft bristles and gentle pressure.
Is gum pain a sign of something serious?
It can be. While minor gum soreness often resolves on its own, pain accompanied by swelling, fever, pus, or loose teeth signals a serious infection requiring urgent dental care.
Why does my gum hurt after eating?
Food particles stuck between teeth or under the gumline, hard or crunchy foods irritating inflamed tissue, or acid from certain foods can all cause post-meal gum pain.
Can a sinus infection cause gum pain?
Yes. The roots of upper back teeth are located very close to the sinus cavities. Sinus inflammation creates pressure that can feel exactly like upper gum or tooth pain.
How long does gum pain usually last?
Gum pain from minor causes like a canker sore or brushing injury heals within one to two weeks. Pain from infection or gum disease will not resolve without treatment and will worsen over time.
Should I stop flossing if my gums hurt?
No. Continue flossing gently to remove bacteria and food debris. If flossing causes severe pain or bleeding, it is a sign your gums need professional attention, not that you should stop.
Can pregnancy cause gum pain?
Yes. Rising hormone levels during pregnancy make gums more sensitive and prone to inflammation, causing a condition called pregnancy gingivitis that requires gentle but consistent oral care.
What is the fastest home remedy for gum pain?
A warm salt water rinse provides quick, safe relief by reducing bacteria and inflammation. Clove oil and a cold compress are also effective for fast temporary pain reduction.
Conclusion
Why does my gum hurt is a question that deserves a real, thorough answer because gum pain is your body’s way of telling you something is wrong. Whether the cause is as simple as brushing too hard or as serious as a dental abscess, identifying the problem quickly makes all the difference.
Most cases of gum pain are preventable with consistent daily oral hygiene, a healthy diet, and regular dental visits every six months. When pain is persistent, severe, or accompanied by swelling and fever, do not wait and hope it goes away. See a dentist promptly.
Your gums protect your teeth and your teeth support your overall health. Taking gum pain seriously in 2026 means protecting your smile, your comfort, and your long-term wellbeing for years to come.






