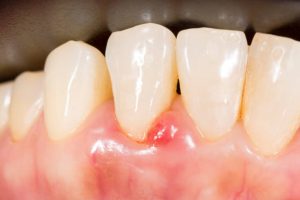
Why Is My Gum Swollen Around One Tooth in the Back Suddenly? 2026
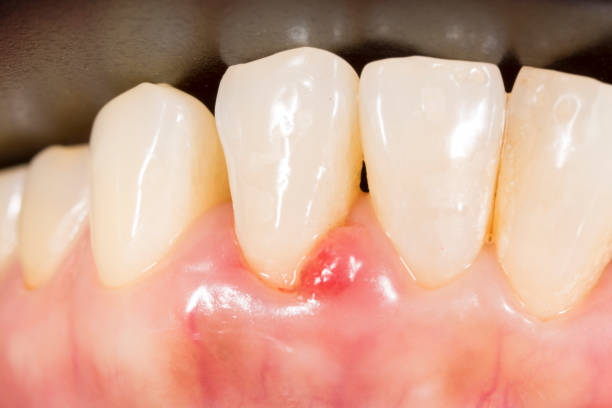
Why Is My Gum Swollen Around One Tooth in the Back You are not alone — this is one of the most common dental complaints in 2026.
Swelling around a single back tooth is almost always your body sending a clear signal that something needs attention.
It could be something minor like trapped food, or something more serious like a dental abscess or gum disease.
Either way, ignoring it is never a good idea.
What Does It Mean When Your Gum Is Swollen Around One Tooth?
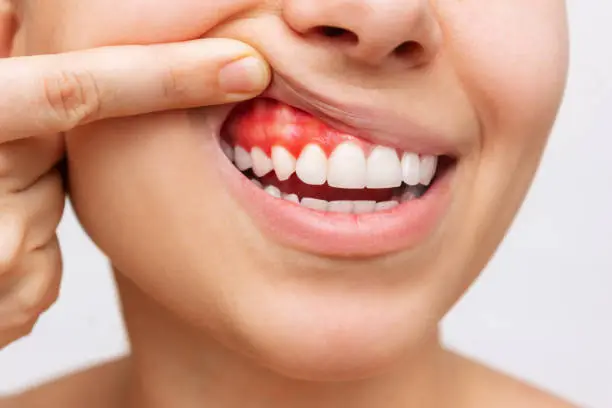
Localized gum swelling means the inflammation is limited to one specific spot rather than spreading across your entire mouth.
This is actually a useful clue. When only one tooth is affected, the cause is usually mechanical or localized — trapped food, a cracked tooth, an abscess, or a gum pocket forming around that specific tooth.
Your gum tissue is soft and protective. When bacteria, debris, or infection irritate it, it responds with inflammation — redness, puffiness, tenderness, and sometimes throbbing pain.
Why Back Teeth Are More Vulnerable
Back teeth — especially molars — are harder to clean properly.
Your toothbrush bristles and floss struggle to reach the very back of your mouth. Plaque and food debris build up in these hard-to-reach areas faster than anywhere else.
This is exactly why swollen gums around one tooth in the back are so common. The location itself creates a perfect environment for bacterial growth and gum irritation.
Top Causes of Swollen Gum Around One Back Tooth
Here is a detailed breakdown of the most common causes, ranked from mild to serious.
Trapped Food or Debris
This is the simplest and most common cause.
A popcorn husk, meat fiber, or seed can slide under your gumline and stay there. Your gum tissue reacts immediately — it swells, reddens, and becomes tender to the touch.
The good news is this type of swelling usually clears up within a day or two once you brush and floss the area properly.
Poor Oral Hygiene and Plaque Buildup
When you do not brush or floss regularly, plaque accumulates fast — especially around back molars.
Plaque is a sticky layer of bacteria. When it builds up along the gumline, it irritates the soft tissue and triggers swelling. Over time, plaque hardens into tartar, which only a dentist can remove.
This is one of the leading reasons people experience recurring gum swelling around one tooth in the back.
Gingivitis — Early Gum Disease
Gingivitis is the earliest and most treatable stage of gum disease.
It occurs when plaque accumulates around the gumline and causes inflammation. Your gums may look red, feel puffy, and bleed a little when you brush. Because back teeth are harder to clean, gingivitis often targets them first.
The good news: gingivitis is fully reversible with proper brushing, flossing, and a professional cleaning.
Periodontitis — Advanced Gum Disease
If gingivitis goes untreated, it progresses to periodontitis.
This is a bacterial infection that starts breaking down the bone and tissue holding your tooth in place. Gum pockets form, deepen, and trap more bacteria. You may notice a loose-feeling tooth or receding gums alongside the swelling.
According to the CDC, nearly 47% of adults over 30 in the US have some form of periodontal disease — making this a major public health concern.
Dental Abscess
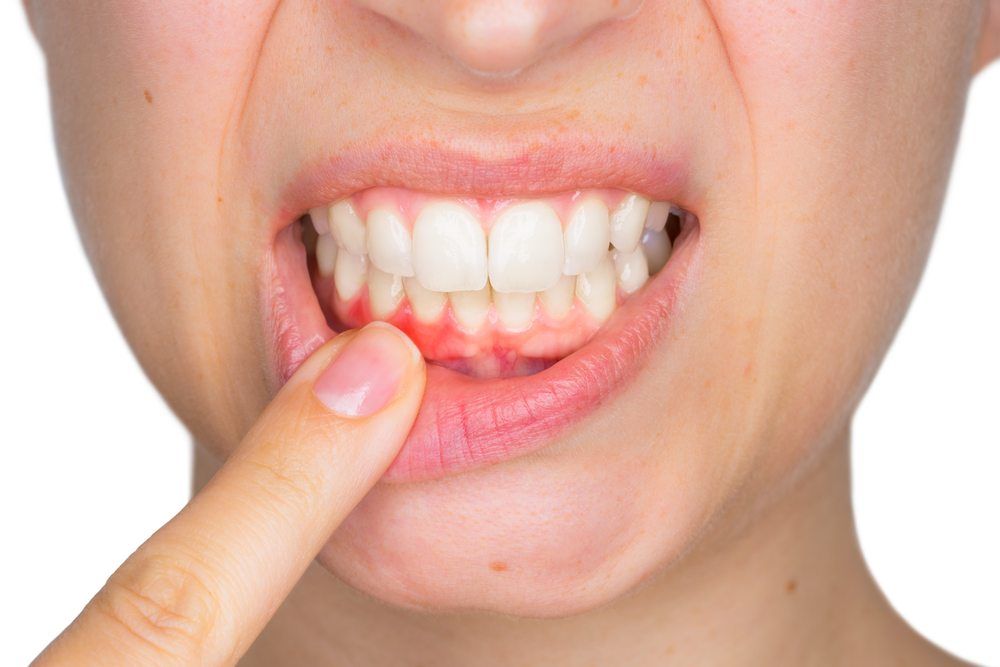
A dental abscess is one of the most serious causes of swollen gum around one tooth.
It is a pocket of pus caused by a bacterial infection — usually the result of untreated tooth decay, a cracked tooth, or advanced gum disease. The swelling can be intense, the pain is often throbbing, and you may notice a bad taste or smell in your mouth.
An abscess is a dental emergency. It will not heal on its own and can spread to your jaw, neck, and beyond if left untreated.
| Abscess Type | Location | Common Cause |
|---|---|---|
| Periapical | Root tip | Untreated cavity or fracture |
| Periodontal | Gum tissue | Advanced gum disease |
Pericoronitis — Wisdom Tooth Problem
Pericoronitis is inflammation of gum tissue around a partially erupted tooth — most often a wisdom tooth.
When a wisdom tooth only partially breaks through the gum, a flap of tissue forms over it. Food, bacteria, and debris get trapped under this flap and cause infection. The result is a painful, swollen gum right at the back of your mouth.
Symptoms of pericoronitis include throbbing pain in the back of the jaw, bad taste in the mouth, difficulty opening your mouth fully, and sometimes fever.
Cracked or Fractured Tooth
A crack in a back molar allows bacteria to enter the tooth structure.
This can trigger an infection in the tooth root or surrounding gum tissue. You may not even see the crack — it can be microscopic. But the swelling and pain it causes are very real.
Cracked tooth syndrome is more common than most people realize, especially in adults who grind their teeth.
Tooth Decay Near the Gumline
A cavity that forms close to the gumline can irritate the surrounding soft tissue.
Bacteria from the decaying tooth spread to the gum tissue and cause localized inflammation. The affected gum may feel sore to the touch and be sensitive to hot and cold foods.
If the decay reaches the tooth’s pulp — the inner nerve chamber — an abscess can form and cause severe swelling.
Gum Injury or Trauma
Sometimes the cause is purely mechanical.
Brushing too hard, using a stiff-bristled toothbrush, accidentally biting into something sharp, or sustaining a blow to the mouth can all cause localized gum swelling around one tooth.
This type of swelling is usually temporary and resolves within a few days as the tissue heals.
Hormonal Changes
Hormonal fluctuations — especially during pregnancy, puberty, or menstruation — can increase blood flow to the gums.
This makes gum tissue more sensitive and prone to swelling, even with normal levels of plaque. Pregnancy gingivitis is a well-known condition where the gums become inflamed due to hormonal changes, not just poor hygiene.
Symptoms You Should Never Ignore
Some symptoms alongside gum swelling are serious warning signs that need prompt dental care.
| Symptom | What It May Indicate |
|---|---|
| Throbbing, severe pain | Dental abscess |
| Pus or bad taste in mouth | Infection or abscess |
| Fever | Spreading infection |
| Facial swelling | Abscess spreading to jaw |
| Difficulty opening your mouth | Pericoronitis or severe infection |
| Loose-feeling tooth | Advanced periodontitis |
| Swollen lymph nodes | Systemic infection |
Do not wait if you experience any of these signs. Visit a dentist or emergency dental clinic the same day.
How to Diagnose the Cause

Your dentist will use a combination of methods to find out why your gum is swollen.
A visual examination lets them see redness, swelling, pus, or gum pockets. Dental X-rays show what is happening beneath the surface — bone loss, decay, abscesses, or impacted teeth. Probing the gum pocket around the tooth helps measure how deep any infection has progressed.
Do not try to self-diagnose based on symptoms alone. Many causes of swollen gum around one tooth look and feel similar, but require very different treatments.
Home Remedies for Swollen Gum Around One Tooth in the Back
These remedies can reduce discomfort and mild inflammation, but they are not substitutes for dental care when something serious is going on.
Warm Saltwater Rinse
This is the most effective and widely recommended home remedy.
Dissolve half a teaspoon of salt in a glass of warm water. Swish around your mouth for 30 seconds and spit. Repeat two to three times daily. Saltwater reduces bacteria, eases inflammation, and supports tissue healing.
Cold Compress
Apply an ice pack wrapped in a cloth to the outside of your cheek for 15 minutes at a time.
This reduces swelling by constricting blood vessels and also numbs the area to reduce pain. Do not apply ice directly to your skin.
Improve Your Brushing and Flossing
Gently but thoroughly brush the affected area with a soft-bristled toothbrush twice daily.
Floss carefully around the swollen tooth to remove any trapped food or plaque. Use a water flosser if regular floss is too painful in that area. Proper technique — brushing at a 45-degree angle away from the gumline — removes bacteria more effectively.
Antiseptic Mouthwash
An over-the-counter antiseptic mouthwash with chlorhexidine or cetylpyridinium can kill bacteria and prevent further plaque buildup.
It does not remove existing tartar, but it helps slow bacterial growth. Use it as a supplement to brushing, not a replacement.
Aloe Vera Gel
Pure, food-grade aloe vera has natural antibacterial and anti-inflammatory properties.
Gently massage a small amount onto the swollen gum with a clean finger. Leave it on for a few minutes before rinsing. Studies suggest aloe vera may help reduce gum inflammation and soothe irritated tissue.
Over-the-Counter Pain Relief
Ibuprofen (Advil, Motrin) is especially useful because it is both a pain reliever and an anti-inflammatory.
Follow the recommended dosage on the packaging. It can reduce gum swelling and pain while you wait for a dental appointment. Do not place aspirin directly on the gum — this can cause a chemical burn to the tissue.
Professional Dental Treatments
When home care is not enough, your dentist has several effective treatment options.
Professional Cleaning and Scaling
If the swelling is caused by plaque and tartar buildup, a professional cleaning removes what brushing cannot.
Scaling involves using special instruments to scrape tartar from the teeth and below the gumline. This is often all that is needed for gingivitis and early periodontitis. Your gums will usually settle down significantly within a few days of treatment.
Deep Cleaning (Scaling and Root Planing)
For more advanced gum disease, a deep cleaning goes below the gumline to remove tartar from the tooth root.
Root planing smooths the root surface so bacteria have less to grip onto. This procedure is done under local anesthesia and may require multiple appointments depending on how many teeth are affected.
Antibiotics
If there is a bacterial infection involved, your dentist may prescribe oral antibiotics or place antibiotic gel directly into the gum pocket.
Antibiotics alone do not resolve the underlying problem — they must be combined with proper dental treatment to be effective long term.
Abscess Drainage
When an abscess has formed, the pus must be drained to relieve pressure and pain.
Your dentist makes a small incision in the gum to allow the infected fluid to escape. After drainage, the area is cleaned and you will likely be given antibiotics to clear any remaining infection.
Root Canal Treatment
If the infection has spread to the tooth’s pulp — the nerve and blood vessel chamber inside the tooth — a root canal is needed.
The infected pulp is removed, the canal is cleaned and shaped, and the tooth is sealed. A crown is usually placed afterward to protect the tooth. This procedure saves the tooth and eliminates the source of infection.
Tooth Extraction
In severe cases where the tooth cannot be saved — due to extreme decay, bone loss, or fracture — extraction may be necessary.
This is always a last resort. Your dentist will discuss replacement options like implants or bridges after the area has healed.
Pericoronitis Treatment
For wisdom tooth-related swelling, treatment depends on severity.
Mild pericoronitis may be treated with an irrigation to flush debris from under the gum flap, combined with a saltwater rinse and antibiotics if needed. Chronic or severe pericoronitis usually requires extraction of the wisdom tooth to permanently resolve the problem.
Prevention: How to Stop Swollen Gums From Coming Back

Prevention is far easier than treatment. These habits protect your back teeth specifically.
Brush twice daily. Use a soft-bristled toothbrush and spend extra time on your back molars. A small-headed toothbrush helps reach further back.
Floss every day. Flossing removes food and plaque from between teeth and along the gumline — areas your toothbrush simply cannot reach.
Use a water flosser. For back teeth, a water flosser is especially effective at flushing debris from hard-to-reach areas.
Rinse with antibacterial mouthwash. A daily rinse helps keep bacterial levels in check and reduces gum inflammation risk.
Get regular dental cleanings. Professional cleanings every 6 months remove tartar buildup before it can trigger gum disease.
Quit smoking. Tobacco use significantly increases the risk of gum disease and slows healing after any dental procedure.
Eat a balanced diet. Vitamin C deficiency, in particular, weakens gum tissue. Leafy greens, citrus, and fresh vegetables support gum health.
Address dental work promptly. Do not delay getting cavities or cracked teeth treated. Early treatment prevents infection from spreading to the gum tissue.
When to See a Dentist Immediately
Some situations cannot wait for a regular appointment.
Go to a dentist the same day if your swelling is accompanied by severe throbbing pain, pus, fever, facial swelling, or difficulty swallowing and opening your mouth. These are signs of a spreading infection that can become life-threatening if not treated quickly.
Even without these red flags, you should book an appointment if your gum swelling has lasted more than a week, keeps coming back in the same spot, or is getting worse despite home care.
Comparison of Common Causes and Their Treatments
| Cause | Severity | Home Care Helps? | Professional Treatment Needed? |
|---|---|---|---|
| Trapped food / debris | Mild | Yes | No (if cleared quickly) |
| Poor hygiene / plaque | Mild–Moderate | Partially | Professional cleaning |
| Gingivitis | Mild–Moderate | Partially | Scaling and cleaning |
| Periodontitis | Moderate–Severe | No | Deep cleaning, scaling |
| Dental abscess | Severe | No | Drainage, root canal, antibiotics |
| Pericoronitis | Moderate–Severe | Partially | Irrigation, antibiotics, extraction |
| Cracked tooth | Moderate–Severe | No | Crown, root canal, or extraction |
| Trauma / injury | Mild | Yes | Only if not improving |
Readiness Checklist Before Your Dental Appointment
Before you go to the dentist, it helps to track the following details so your dentist can make the best diagnosis quickly.
- How long has the swelling been present?
- Is it getting better or worse?
- Do you feel throbbing pain or pressure?
- Do you notice any bad taste or smell?
- Any fever, facial swelling, or swollen neck glands?
- Have you had recent dental work on that tooth?
- Are your wisdom teeth fully erupted?
Frequently Asked Questions (FAQs)
Why is my gum swollen around just one tooth in the back?
Localized swelling around one back tooth usually points to trapped food, plaque buildup, an abscess, gum disease, or a wisdom tooth problem. Back molars are harder to clean and more prone to bacterial buildup, which is why swelling often starts there.
Can a swollen gum around one tooth go away on its own?
Mild swelling caused by trapped food or minor irritation may clear up within a day or two once the area is cleaned. Swelling from gum disease, tooth decay, or an abscess will not resolve without professional dental treatment.
Is a swollen gum around one back tooth a dental emergency?
It can be — especially if caused by a dental abscess. If you have severe pain, pus, fever, or facial swelling alongside the gum swelling, you need to see a dentist the same day.
What is the fastest way to reduce gum swelling at home?
A warm saltwater rinse is the most effective immediate home remedy. Rinse two to three times daily with half a teaspoon of salt in warm water. Ibuprofen can help with pain and inflammation in the short term.
Can pericoronitis go away without treatment?
Mild pericoronitis can sometimes settle temporarily, but it tends to come back. If the wisdom tooth is partially erupted and there is a gum flap present, the problem will usually recur until the tooth is extracted.
What does a gum abscess feel like?
A gum abscess typically causes severe throbbing pain, a visible swollen bump on the gum, a bad taste in the mouth, and sometimes fever. The area may feel warm to the touch. This is a dental emergency.
How long does swollen gum around one tooth last?
If caused by trapped food or minor irritation, swelling may resolve within 2 to 3 days with good hygiene. If caused by infection, gum disease, or an abscess, it will persist or worsen without treatment.
Can brushing too hard cause gum swelling around one tooth?
Yes. Aggressive brushing with a hard-bristled toothbrush can irritate and cut gum tissue, causing localized swelling around one tooth. Switch to a soft-bristled brush and use gentle circular strokes.
Does gum swelling around one tooth mean I need a root canal?
Not necessarily. A root canal is only needed if the infection has reached the tooth’s inner pulp. Many cases of swollen gum are resolved with professional cleaning, antibiotics, or abscess drainage without requiring a root canal.
Can gum swelling around one tooth lead to tooth loss?
Yes, if left untreated. Advanced periodontitis destroys the bone and tissue supporting the tooth, which can eventually lead to the tooth becoming loose and falling out or needing extraction.
Conclusion
If your gum is swollen around one tooth in the back, your body is sending you a clear message — pay attention now, not later.
The causes range from something as simple as trapped food debris to something as serious as a spreading dental abscess.
Back molars are the most vulnerable teeth in your mouth because they are hardest to keep clean, which is why localized swelling tends to appear there first.
Start with good home care — warm saltwater rinses, gentle brushing, careful flossing, and ibuprofen for pain relief.
These steps can ease mild irritation quickly.
But if the swelling lasts more than a week, is getting worse, or comes with pain, pus, fever, or facial changes, do not delay.
Book a dental appointment immediately.
Early treatment prevents small problems from becoming expensive, painful, and potentially dangerous ones.
Your gum health directly affects your overall health — so take that swelling seriously and act on it today.