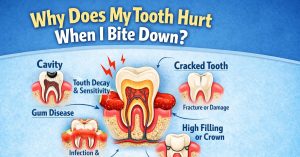
Why Does My Teeth Hurt When I Bite Down — Is It Serious? (2026)
Why Does My Teeth Hurt When I Bite Down? your mouth is sending you a clear warning signal that something needs attention.
Tooth pain when biting is one of the most common dental complaints in 2026, and it can range from a minor sensitivity issue to a sign of a serious infection or structural damage.
The cause could be as simple as a high filling or as serious as an abscess. This guide breaks down every possible reason your teeth hurt under pressure, how serious each one is, and exactly what to do about it — so you can stop guessing and start getting relief.
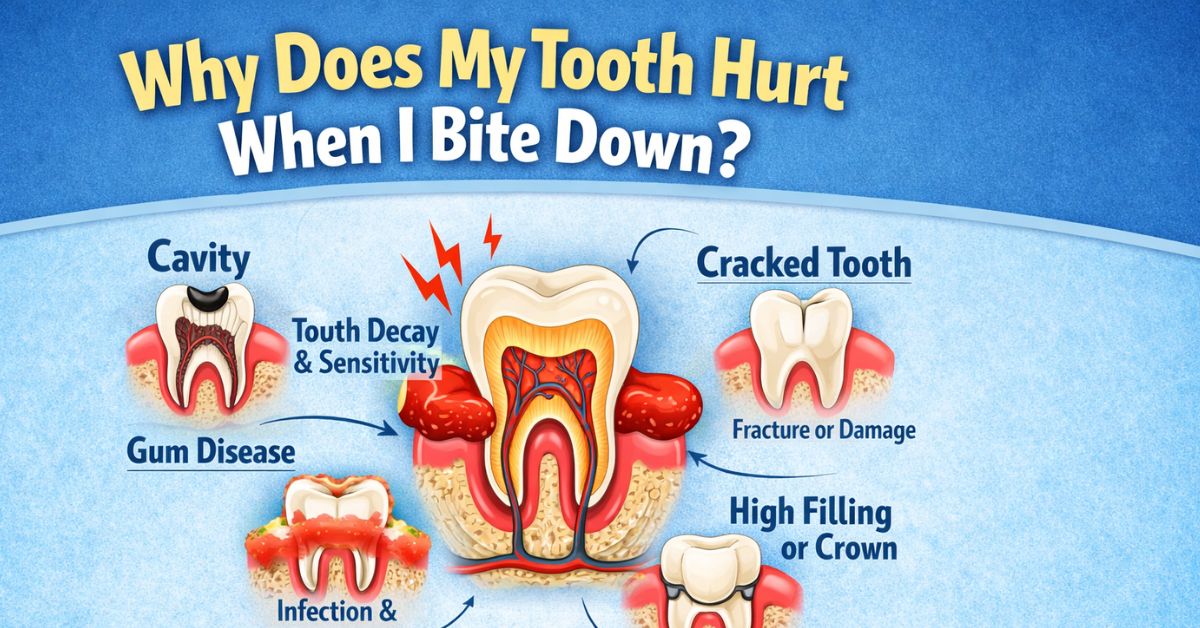
Why Does My Teeth Hurt When I Bite Down? Why Tooth Pain Happens When You Bite Down
Inside every tooth is a soft core called the pulp, which contains nerves and blood vessels. When the tooth structure is healthy and intact, biting pressure is absorbed evenly across your teeth without pain.
When something goes wrong — a crack, a cavity, an infection, or inflammation — biting pressure irritates the nerve inside. Even a tiny hairline fracture can cause the nerve to fire sharply the moment you apply any force.
Understanding what is happening inside your tooth helps you recognize which cause applies to you and how urgent the treatment really is.
The 12 Most Common Reasons Your Teeth Hurt When You Bite Down
1. Cracked or Fractured Tooth
A cracked tooth is one of the leading causes of bite-related pain. Small cracks can develop from chewing hard foods, grinding teeth, or old dental work — and they are often invisible to the naked eye and do not always show on X-rays.
The telltale sign is sharp pain that flares when you bite down and then fades quickly when you release pressure. This happens because biting causes the crack to open slightly, irritating the nerve inside.
Left untreated, the crack can deepen, allow bacteria in, and eventually require a crown or root canal. Early treatment — usually a crown — prevents the problem from getting worse.
2. Tooth Decay and Cavities
Tooth decay does not always hurt in its early stages. According to the CDC, over 90% of adults have had at least one cavity — meaning most people have experienced decay at some point without realizing it.
When decay reaches the deeper layers of a tooth and gets close to the pulp, pressure from biting pushes on the sensitive inner tissue and triggers pain. You may also notice sensitivity to sweet foods or a visible dark spot.
The sooner a cavity is caught, the simpler the fix. Early decay is treated with a filling. Deep decay that has reached the pulp may require a root canal.
3. Dental Abscess or Tooth Infection
A dental abscess is a bacterial infection that builds up at the root of a tooth or in the surrounding gum. It develops when untreated decay or a crack allows bacteria to reach the pulp.
The infection creates pressure and swelling inside the bone, which makes biting extremely painful. Other signs include a bad taste in the mouth, swelling in the face or gum, fever, and a visible pimple-like bump on the gum near the tooth.
An abscess is a dental emergency. It will not go away on its own and can spread to the jaw, neck, or beyond if not treated quickly. Treatment usually involves a root canal or tooth extraction along with antibiotics.
4. Gum Disease (Periodontitis)
Gum disease in its advanced form, called periodontitis, causes the gum tissue to pull away from the teeth. This exposes the root surfaces, which are not protected by enamel and are far more sensitive to pressure and temperature.
When the supporting tissue around a tooth becomes inflamed or infected, biting transfers force directly into irritated tissue. You may notice bleeding when brushing, swollen or red gums, bad breath, and teeth that feel slightly loose.
Treatment ranges from a deep cleaning procedure called scaling and root planing to surgery in severe cases. Catching gum disease early makes a significant difference in how much treatment is needed.
5. A High Filling or Crown
After getting a filling or crown placed, it is possible for the restoration to sit slightly too high — even by a fraction of a millimeter. That tiny elevation means one tooth is hitting harder than all the others every time you close your mouth.
This extra pressure inflames the periodontal ligament, the small connective tissue that holds each tooth in its socket. The result is a tooth that feels bruised or sore specifically when biting down.
The fix is simple and fast. Your dentist uses special marking paper to identify exactly where the bite is too high, then smooths down the restoration. Pain usually disappears within a day or two of the adjustment.
6. Loose, Worn, or Damaged Filling
Fillings do not last forever. Over time they can crack, shift, wear down, or pull away from the tooth. When this happens, a gap forms between the filling and the tooth surface.
Bacteria enter that gap and irritate the tooth underneath. When you bite down, the filling may move or press against sensitive tissue, causing discomfort. You might also notice a rough edge or feel that food gets caught in the same spot.
A damaged filling needs to be replaced promptly. Leaving it in place allows decay to develop beneath it, which makes the eventual repair more complex and costly.
7. Teeth Grinding and Bruxism
Bruxism is the medical term for grinding or clenching teeth, usually during sleep. Many people are unaware they do it until a partner mentions it or a dentist spots the worn enamel.
The constant pressure from grinding weakens enamel, creates micro-cracks, inflames the periodontal ligament, and leaves the jaw muscles sore. If your teeth hurt primarily in the morning or after stressful periods, bruxism is a likely culprit.
Custom night guards are the standard first-line treatment. They create a cushion between upper and lower teeth and prevent grinding from doing further damage while you sleep. Stress management techniques can also reduce the frequency and intensity of bruxism.
8. TMJ Disorder (Temporomandibular Joint Disorder)
The temporomandibular joint — the TMJ — is the hinge that connects your jaw to your skull. When this joint becomes inflamed or misaligned, the pain can radiate to the teeth, making chewing feel uncomfortable even when the teeth themselves are perfectly healthy.
TMJ disorders affect between 5 and 12 percent of people and are more common in women aged 20 to 40. Symptoms often include jaw clicking or popping, difficulty opening the mouth fully, ear pain, headaches, and facial soreness.
Treatment ranges from nightguards and jaw exercises to physical therapy and anti-inflammatory medications. Severe cases may require specialist care, but many people find significant relief through conservative approaches.
9. Sinus Infection (Sinus Toothache)
This is one of the most commonly overlooked causes of tooth pain when biting. Your upper back teeth — the molars — sit directly below the sinus cavities. When the sinuses become inflamed or infected, the resulting pressure pushes down on the roots of these teeth.
The key distinguishing feature is that a sinus toothache typically affects several upper teeth at once rather than a single tooth. It often comes with nasal congestion, facial pressure, and tenderness when you bend forward.
Treatment is directed at the sinus infection itself — nasal decongestants, saline rinses, steam, or antibiotics if prescribed by a doctor. As the sinuses clear, the tooth pain resolves without any dental work needed.
10. Dentin Hypersensitivity (Exposed Dentin)
Beneath the outer enamel of each tooth is a layer called dentin. Dentin contains tiny microscopic channels called dentinal tubules that lead directly to the nerve of the tooth.
When enamel wears away from aggressive brushing, acidic foods, or gum recession, the dentin becomes exposed. Pressure from biting — especially on hard, cold, or hot food — travels through those tubules and triggers a sharp, temporary nerve response.
Desensitizing toothpastes containing potassium nitrate or stannous fluoride can reduce this sensitivity over time. Your dentist may also apply fluoride varnish or a bonding agent to seal the exposed dentin and provide faster relief.
11. Impacted Wisdom Teeth
Wisdom teeth, also called third molars, typically emerge between the ages of 18 and 24. When there is not enough space for them to come in properly, they become impacted — stuck under the gum or pushing against neighboring teeth.
Impacted wisdom teeth create pressure, inflammation, and sometimes infection in the surrounding tissue. The result is pain in the back of the mouth that often worsens when biting down, especially on the lower jaw.
Extraction is the standard treatment for impacted wisdom teeth. The procedure is extremely common and, when performed promptly, prevents damage to adjacent teeth and reduces the risk of recurring infection.
12. Periodontal Ligament Inflammation
Every tooth is held in its socket by a small but important connective tissue called the periodontal ligament. This tissue acts like a shock absorber for your teeth during chewing.
When the ligament becomes inflamed — from injury, infection, excessive bite pressure, or grinding — even normal biting force triggers significant pain. This is sometimes called “ligament sprain” of the tooth.
The inflamed ligament can heal on its own once the underlying cause is removed. Depending on the trigger, treatment may involve bite adjustment, antibiotics, or rest from hard foods for a period of time.
Causes by Location: Where Is Your Pain?

| Location of Pain | Most Likely Causes |
|---|---|
| Single back tooth | Cracked tooth, cavity, abscess, high filling |
| Multiple upper back teeth | Sinus infection, bruxism |
| Front teeth | Trauma, crack, old dental work, gum recession |
| All teeth or widespread | TMJ disorder, bruxism, dentin hypersensitivity |
| Bottom teeth | Gum disease, enamel wear, bruxism, impacted wisdom tooth |
| After recent dental work | High filling or crown, post-procedure inflammation |
Severity Guide: How Serious Is It?
| Cause | Urgency Level | Can It Wait? |
|---|---|---|
| Dental abscess | Emergency | No — see dentist same day |
| Deep cavity | High | Within a few days |
| Cracked tooth | High | Within a week |
| Gum disease | Moderate | Within 1 to 2 weeks |
| High filling or crown | Low | A few days (quick fix) |
| Sinus toothache | Low to moderate | Manage sinuses first |
| Bruxism or TMJ | Moderate | Book appointment soon |
| Dentin hypersensitivity | Low | Try home treatment first |
| Impacted wisdom tooth | Moderate to high | Within a week |
Home Remedies to Manage Pain While You Wait
These steps can reduce discomfort temporarily but will not fix the underlying problem. They are meant to hold you over until you can see a dentist.
Warm salt water rinse. Dissolve half a teaspoon of salt in a cup of warm water and rinse gently for 30 seconds. Salt water reduces inflammation and cleans the area around an irritated tooth.
Over-the-counter pain relievers. Ibuprofen or acetaminophen can reduce tooth pain and swelling. Ibuprofen is generally more effective for dental pain because it targets inflammation directly.
Cold compress. Apply a cold pack wrapped in a cloth to the outside of your face for 15 to 20 minutes. This reduces swelling and numbs the area.
Clove oil. Clove oil contains eugenol, a natural anesthetic. Dab a small amount on a cotton ball and apply it to the sore tooth for temporary numbing relief.
Avoid trigger foods. Stay away from hard, crunchy, very hot, very cold, or sweet foods until you have been seen by a dentist. These will all aggravate the pain and potentially worsen the problem.
Sleep with your head elevated. Lying flat increases blood pressure in the head, which can intensify tooth pain. Propping your head up slightly on an extra pillow can reduce throbbing overnight.
Desensitizing toothpaste. If the pain is from sensitivity rather than infection, brushing with a desensitizing toothpaste and leaving it on the tooth overnight can reduce nerve reactivity over time.
Treatments Your Dentist May Recommend
| Cause | Dental Treatment |
|---|---|
| Cracked tooth | Crown, bonding, or root canal depending on severity |
| Cavity | Filling or root canal if decay has reached the pulp |
| Abscess | Root canal and antibiotics, or extraction |
| Gum disease | Scaling and root planing, surgery if advanced |
| High filling or crown | Bite adjustment (quick, painless procedure) |
| Bruxism | Custom night guard, stress management |
| TMJ disorder | Night guard, physical therapy, anti-inflammatories |
| Impacted wisdom tooth | Extraction |
| Dentin hypersensitivity | Fluoride varnish, bonding agent, desensitizing products |
Warning Signs That Mean You Need Urgent Dental Care
Some situations cannot wait for a routine appointment. Go to a dentist or emergency dental clinic as soon as possible if you experience any of the following.
Swelling in your face, jaw, or neck is a red flag. It can indicate an abscess that is spreading beyond the tooth. Untreated dental infections can reach the throat and airway, which is life-threatening.
A fever alongside tooth pain suggests the infection has entered your bloodstream. This is a medical emergency, not just a dental inconvenience.
Pain that throbs constantly without stopping, especially pain that keeps you awake at night, suggests an active nerve infection. Over-the-counter medications will only dull this temporarily.
Pus, a bad taste, or a visible bump on the gum near a sore tooth all point to an abscess. Do not wait and hope it goes away — it will not.
Pain that spreads to the ear, neck, or head alongside jaw stiffness or locking could indicate a severe TMJ flare or a spreading infection. Get evaluated promptly.
How Dentists Diagnose the Cause of Bite Pain
Your dentist uses several tools to track down the exact cause of tooth pain when biting. Knowing what to expect helps you prepare for your appointment.
A percussion test involves the dentist gently tapping each tooth with a small instrument to identify which one reacts. A bite stick test has you bite down on a specific point to isolate whether a crack is present. Dental X-rays identify cavities, infections, and bone changes that are not visible on the surface.
Temperature testing applies cold or warm stimuli to the tooth to see how the nerve responds — and how long the response lasts. A prolonged or lingering response often indicates nerve involvement. Special marking paper called articulating paper is used to check whether a filling or crown is sitting too high in your bite.
How to Prevent Tooth Pain When Biting Down

Most causes of bite-related tooth pain are preventable with consistent habits. Brush twice a day with a soft-bristled toothbrush. Use fluoride toothpaste and floss daily to prevent the decay and gum disease that are responsible for the majority of dental pain.
Wear a mouthguard during contact sports. A single hard impact can crack a tooth, leading to months of pain and expensive treatment.
If you know you grind your teeth, ask your dentist about a custom night guard before the grinding causes visible damage. Early intervention costs far less than treating cracked or worn teeth after the fact.
Limit acidic foods and drinks like citrus, soda, and wine. These erode enamel over time and accelerate sensitivity. If you consume them, rinse with water afterward rather than brushing immediately, which can spread the acid further.
Schedule dental checkups every 6 months. Many of the problems that cause bite pain — cavities, cracked fillings, early gum disease — are easily caught and treated when identified early. By the time they are causing significant pain, they are usually more complex and costly to fix.
Frequently Asked Questions (FAQs)
Why does my tooth hurt when I bite down but there is no visible damage?
Hairline cracks and early infections often cause pain without any visible sign. A dentist can use bite tests, percussion testing, and X-rays to find problems that cannot be seen with the naked eye.
Is it normal for teeth to hurt when biting after a filling?
Some sensitivity for a few days after a filling is normal as the tooth settles. If pain persists beyond a week or worsens, the filling may be sitting too high and needs a quick adjustment.
Can a sinus infection really make my teeth hurt when I bite?
Yes. Your upper back molars sit directly beneath the sinus cavities. Sinus inflammation creates pressure that pushes down on the tooth roots, causing pain that feels exactly like a toothache.
Can teeth grinding cause tooth pain when biting?
Yes. Grinding wears down enamel, creates micro-cracks, and inflames the periodontal ligament. All of these lead to pain when any biting pressure is applied, especially in the morning.
When should I go to the emergency dentist for bite pain?
Go immediately if you have facial or jaw swelling, a fever, constant throbbing pain that does not ease, pus near a tooth, or pain spreading to the neck. These are signs of a spreading infection.
What does an abscessed tooth feel like when biting down?
An abscess usually causes severe, constant pain that is significantly worse when biting or applying any pressure to the tooth. It may also come with swelling, a bad taste, and a bump on the gum near the affected tooth.
Can TMJ disorder cause tooth pain when biting?
Yes. TMJ dysfunction causes pain that radiates into the teeth even when the teeth themselves have no damage. Clicking, jaw stiffness, or difficulty opening the mouth wide are common accompanying signs.
How do I know if my tooth pain when biting is serious?
Pain that is severe, constant, accompanied by swelling or fever, or has lasted more than a few days is serious. Pain that is mild, linked to a specific food type, or that appeared after dental work is usually less urgent but should still be evaluated.
Can I fix tooth pain when biting at home?
Home remedies like salt water rinses, clove oil, and over-the-counter pain relievers can reduce discomfort temporarily. They do not fix the underlying problem and should not be used as a substitute for dental care.
What is the most common reason teeth hurt when biting?
Cracked teeth, cavities, and high fillings are the three most common causes seen in dental offices. Each is treatable, and the earlier they are caught, the simpler and less expensive the treatment.
Conclusion
When your teeth hurt when you bite down, the problem is almost never something that fixes itself on its own. In 2026, dental care is more accessible and more precise than ever — and most causes of bite-related tooth pain, from a cracked tooth to a high filling to a sinus infection, are completely treatable when caught early.
The key is not to ignore the pain or mask it indefinitely with over-the-counter medication. Use the information in this guide to understand what might be happening, manage your discomfort temporarily with safe home remedies, and book a dental appointment without delay. Your teeth are telling you something important — listen to them.