Why Does the Roof of My Mouth Hurt When I Swallow? Fix 2026
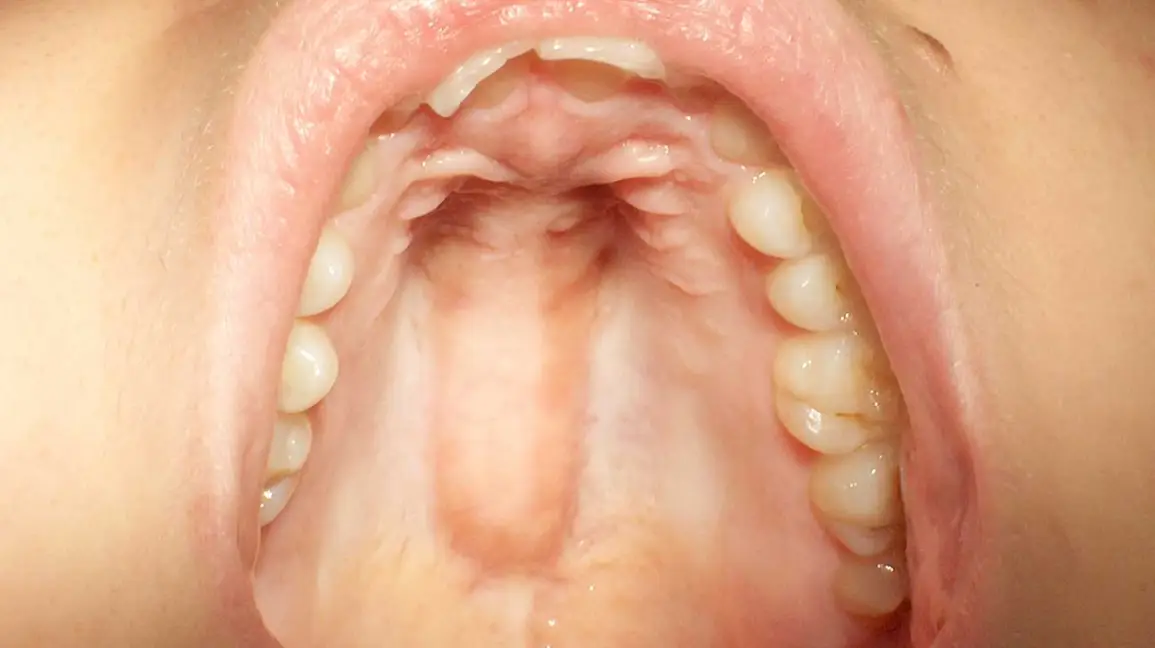
Why does the roof of my mouth hurt when I swallow is a question more people ask than you might expect — and the answer is almost never simple.
The roof of your mouth, known as the palate, is a complex structure divided into the hard palate at the front and the soft palate at the back.
Because the soft palate moves every time you swallow, any inflammation, infection, injury, or irritation in that area becomes instantly noticeable.
Why Does the Roof of My Mouth Hurt When I Swallow? Understanding the Anatomy of the Palate
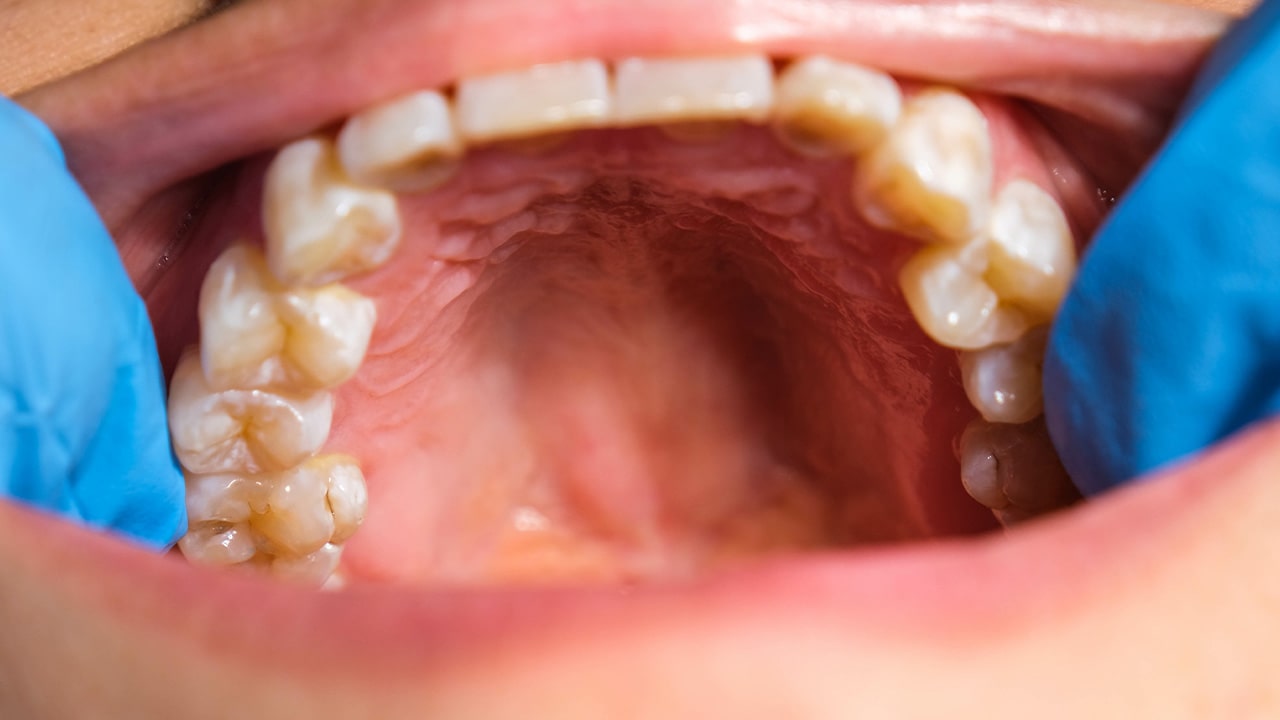
Before getting into causes, it helps to understand exactly what you are dealing with when you feel pain in the roof of your mouth.
The hard palate makes up the front two-thirds of the roof of your mouth. It is reinforced by bone and covered by a thick layer of mucous membrane. It does not move during swallowing, so pain here tends to feel like a localised soreness or tenderness when food contacts it.
The soft palate is the muscular section at the back of the roof of your mouth, right where it begins to slope downward toward your throat. It is made of muscle and connective tissue, and it moves actively every single time you swallow to seal off the nasal passages.
This is the critical point: when the soft palate is inflamed, irritated, or infected, every swallowing motion aggravates it. That is why swallowing pain in the roof of the mouth points so strongly to the soft palate — and why infections involving the throat, tonsils, and sinuses all show up there first.
Why Swallowing Makes Palate Pain Worse
Swallowing is an involuntary reflex involving over 30 muscles working in coordinated sequence. You cannot stop it or slow it down.
When the soft palate is even mildly inflamed, every swallow pulls and stretches the irritated tissue, sending a pain signal that feels disproportionately sharp relative to the underlying injury. This is why people with mild throat infections or small ulcers on the soft palate often feel like they cannot eat or drink anything without significant discomfort.
Understanding this mechanism helps explain why pain that feels severe during swallowing is often being amplified by muscle movement, not necessarily by the severity of the underlying problem.
The 12 Most Common Causes of Roof of Mouth Pain When Swallowing
Strep Throat and Bacterial Pharyngitis
Strep throat is one of the most common reasons the roof of your mouth hurts when you swallow. It is caused by Group A Streptococcus bacteria, and it inflames the pharynx, tonsils, and soft palate simultaneously.
Classic signs of strep include a sudden, severe sore throat, painful swallowing, red and swollen tonsils (sometimes with white patches or pus), tiny red spots on the soft palate, swollen lymph nodes in the neck, and fever. Strep throat is confirmed with a rapid throat swab or culture and is treated with a 10-day course of penicillin or amoxicillin.
Left untreated, strep can progress to scarlet fever, rheumatic fever, or peritonsillar abscess. If you suspect strep, do not wait — it will not resolve on its own.
Tonsillitis
Tonsillitis is inflammation of the tonsils, which sit at the sides of the back of the throat — right next to the soft palate. When the tonsils swell, the adjacent soft palate tissue also becomes inflamed and painful during swallowing.
Chronic tonsillitis can flare repeatedly without any obvious infection trigger. People with chronic tonsillitis often experience recurring bouts of swallowing pain, visible red or pitted tonsils, and sometimes tonsil stones (calcified debris in the tonsillar crypts). Antibiotic treatment manages acute episodes; chronic cases may ultimately require a tonsillectomy.
Thermal Burns from Hot Food or Drinks
The most common minor cause of roof of mouth pain is a thermal burn from food or drink that was too hot. Pizza straight from the oven, freshly brewed coffee, hot soup, and toasted bread are the most frequent culprits.
Burns affect the delicate mucous membrane of the palate and can cause immediate pain, rawness, and tenderness that worsens when swallowing for several days afterward. A mild burn typically heals on its own within 3 to 7 days. During healing, cold or room-temperature foods and drinks are your best allies.
Canker Sores on the Palate (Aphthous Ulcers)
Canker sores are small, round ulcers with a white or yellow centre and a red border. They are non-contagious and can develop anywhere inside the mouth — including the hard or soft palate.
When a canker sore forms on the soft palate, swallowing pain can be significant because the ulcer is stretched and compressed with every swallow. Common triggers include stress, hormonal changes, minor mouth trauma, iron or B12 deficiency, and certain foods such as citrus and spicy dishes. Most canker sores heal within 7 to 14 days without treatment. Saltwater rinses, topical anaesthetic gels, and avoiding trigger foods speed recovery.
Oral Thrush (Candida Overgrowth)
Oral thrush is a fungal infection caused by an overgrowth of Candida albicans, a yeast normally present in the mouth in small amounts. When the immune system is weakened, or when antibiotics disrupt the normal balance of oral bacteria, Candida multiplies and creates white, creamy patches on the palate, tongue, and inner cheeks.
These patches can bleed if scraped and cause a burning soreness that makes swallowing uncomfortable. Oral thrush is more common in people who wear dentures, use corticosteroid inhalers, have diabetes, are undergoing chemotherapy, or have HIV. Treatment requires prescription antifungal medication — nystatin suspension or fluconazole tablets.
Cold Sores (Herpes Simplex Virus) on the Palate
The herpes simplex virus type 1 (HSV-1), which causes cold sores around the lips, can also cause lesions inside the mouth, including on the hard palate. These fluid-filled blisters are painful, tingle before they appear, and make swallowing especially uncomfortable.
HSV-1 is triggered by stress, fever, fatigue, sunburn, or any factor that temporarily suppresses immune function. The outbreak typically lasts 7 to 10 days. Antiviral medications such as aciclovir can reduce the duration and severity of the outbreak if taken early, ideally at the first sign of tingling.
Sinus Infection (Sinusitis)
The maxillary sinuses sit directly above the hard palate, separated by a thin layer of bone. When these sinuses become infected and inflamed, the pressure they exert downward can cause pain in the roof of the mouth — especially during swallowing when head position shifts slightly.
Sinus-related palate pain is almost always accompanied by nasal congestion, facial pressure around the cheeks and eyes, postnasal drip, and reduced sense of smell. The palate pain clears once the sinus infection resolves. Saline nasal rinses, decongestants, and — in bacterial sinusitis — antibiotics are the standard treatment.
Dry Mouth (Xerostomia)
Dry mouth occurs when the salivary glands do not produce enough saliva to keep the oral tissues moist. Saliva is essential for lubricating the palate and throat during swallowing. Without it, swallowing becomes a friction-heavy movement that irritates the dry mucous membrane of the palate.
Dry mouth is a side effect of hundreds of common medications, including antihistamines, antidepressants, blood pressure medications, and decongestants. It is also caused by dehydration, mouth breathing, and autoimmune conditions such as Sjögren’s syndrome. Staying hydrated, using sugar-free gum or lozenges to stimulate saliva, and using artificial saliva sprays can all provide relief.
Dental Abscess or Infected Upper Tooth
The roots of the upper back teeth sit very close to the palate and the floor of the maxillary sinus. When an upper tooth develops an abscess — a pocket of infection at the root tip — the pain and pressure can radiate directly into the roof of the mouth and worsen during swallowing.
Dental abscesses also feel worse when biting down on the affected side and may be accompanied by swelling in the gum, a raised bump near the tooth root, bad taste in the mouth, or fever. A dental abscess will not resolve without professional treatment. The tooth requires either root canal therapy to remove the infection or extraction if the tooth cannot be saved.
Acid Reflux and GERD
Gastro-oesophageal reflux disease (GERD) causes stomach acid to travel up the oesophagus and, in some cases, reach the throat and the back of the mouth. Chronic acid exposure irritates and inflames the soft palate and throat, causing a burning sensation and soreness that worsens during swallowing.
GERD-related palate pain is typically worse after large meals, when lying down, or after consuming alcohol, caffeine, spicy food, or tomato-based products. Lifestyle modifications combined with proton pump inhibitors or H2 blockers prescribed by a doctor are the standard treatment approach.
Ill-Fitting Dental Appliances
Dentures, retainers, orthodontic braces, and night guards that do not fit correctly can rub repeatedly against the palate, creating friction wounds, pressure sores, and ulcers that make swallowing painful.
This type of palate pain develops gradually and is often worst in a specific location that corresponds to where the appliance contacts the tissue. The solution is a professional adjustment or refitting of the appliance by a dentist. Do not continue wearing an appliance that is causing tissue damage.
Nutritional Deficiencies
Deficiencies in iron, vitamin B12, folate, and zinc are all known to cause mouth sores, burning sensations, and increased tissue fragility inside the mouth. These deficiencies make the palate more vulnerable to injury and slower to heal, prolonging any pain during swallowing.
If you are getting recurrent canker sores or persistent palate soreness without any obvious cause, ask your doctor to test your iron, B12, and folate levels. Correcting the deficiency often significantly reduces the frequency and severity of mouth sores.
Comparing Causes by Location of Pain

Where exactly the pain is felt in the roof of your mouth provides important clues about its cause.
| Pain Location | Most Likely Causes |
|---|---|
| Front hard palate, burns when touched | Thermal burn, canker sore, physical scratch |
| Back soft palate, worse when swallowing | Strep throat, tonsillitis, viral infection |
| All over the palate, with white patches | Oral thrush, herpes simplex virus outbreak |
| One side only | Peritonsillar abscess, infected upper tooth, salivary gland blockage |
| Back palate with nasal congestion | Sinus infection, postnasal drip, allergies |
| Burning without visible sore | GERD acid reflux, dry mouth, burning mouth syndrome |
| Near an upper tooth, with swelling | Dental abscess, advanced gum disease |
Using this table alongside your other symptoms helps narrow down the cause significantly before you visit a professional.
How to Tell If It Is Serious
Most causes of roof of mouth pain when swallowing are minor and resolve on their own within a week or two. However, some situations demand prompt professional attention.
Signs That Need Urgent Attention
Difficulty breathing or swallowing fluids — this level of swelling suggests a peritonsillar abscess or epiglottitis, both of which are medical emergencies. Go to an emergency department immediately.
High fever above 38.5°C (101.3°F) — fever alongside palate pain suggests a bacterial infection that may need antibiotic treatment. See a doctor the same day.
Swelling on one side of the throat — one-sided throat swelling, with the uvula pushed to one side, is a hallmark of peritonsillar abscess and requires urgent drainage.
White or yellow patches that do not wipe off — this can indicate oral thrush or a bacterial infection requiring treatment. Do not ignore it.
Sores or lesions present for more than two weeks without improvement — persistent non-healing sores anywhere in the mouth should be evaluated for oral cancer. Early detection is critical.
A firm lump or growth that grows over days or weeks — any unexplained growth in the mouth that persists beyond two weeks needs a professional assessment.
Jaw or facial swelling — spreading infection from a dental abscess can become life-threatening if it reaches the neck and airway.
Home Remedies That Actually Help
For minor causes — burns, canker sores, mild viral infections, or small physical scratches — several home remedies can effectively reduce pain and speed healing.
Warm Saltwater Rinse
Mix half a teaspoon of salt into a cup of warm (not hot) water and gently swish for 15 to 30 seconds before spitting. Saltwater reduces inflammation, draws out fluid from swollen tissue, and creates a mildly antibacterial environment that keeps the area clean during healing.
Repeat two to three times per day, particularly after meals. It is one of the most evidence-supported home remedies for any oral irritation.
Cold Foods and Cool Water
Cold temperatures numb irritated tissue and reduce swelling temporarily. Drinking cold water, eating ice cream, or using crushed ice held gently in the mouth can provide meaningful short-term relief for burns and ulcers on the palate.
Avoid ice cubes directly pressed against a burn — this can cause additional cold-related damage to already compromised tissue. Cool water and soft cold foods are the safer option.
Honey
Raw honey has well-documented antimicrobial and anti-inflammatory properties. A small amount placed directly on a canker sore or burn on the palate can reduce bacterial activity, create a protective coating, and soothe inflamed tissue.
Manuka honey, with its higher concentration of active antibacterial compounds, is particularly effective. Apply with a clean finger or cotton swab up to three times per day.
Over-the-Counter Topical Anaesthetics
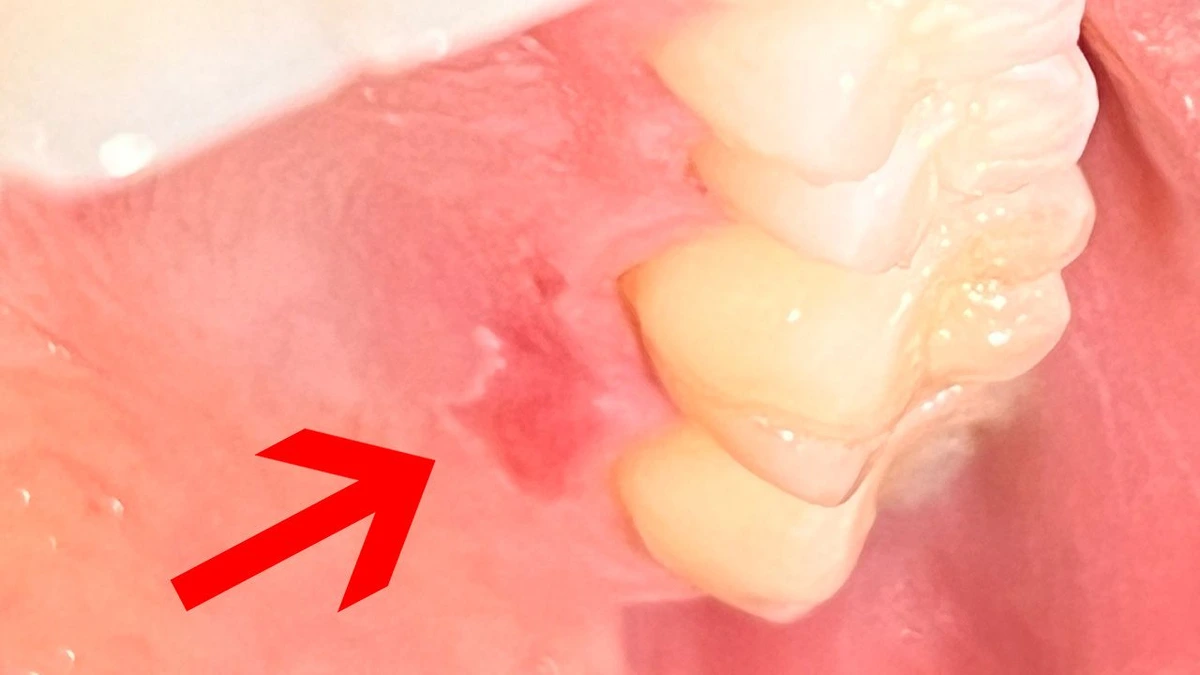
Gels and sprays containing benzocaine or lidocaine (found in products like Orajel and Anbesol) can be applied directly to sores or burns on the palate for short-term pain relief. These work by temporarily numbing the nerve endings in the surface tissue.
They do not treat the underlying cause but can make eating, drinking, and swallowing more manageable while the tissue heals. Follow the dosage instructions carefully and do not exceed the recommended daily limit.
Stay Hydrated
Adequate hydration is essential for maintaining a moist, protected oral environment. Dehydration worsens dry mouth, concentrates any irritants already present in saliva, and slows tissue healing.
Aim for at least 8 glasses of water per day. If you have a fever alongside the mouth pain, increase intake to compensate for fluid loss. Warm herbal teas — particularly chamomile — can soothe inflamed tissue while providing hydration.
Avoid Triggers
Spicy, acidic, crunchy, and very hot foods all aggravate irritated palate tissue and delay healing. Temporarily switching to a soft, bland diet — yoghurt, scrambled eggs, mashed potato, oatmeal, smoothies — protects the tissue and makes swallowing significantly less painful during recovery.
Alcohol and tobacco should also be avoided. Both impair tissue healing, dry out oral mucous membranes, and introduce additional irritants to already compromised tissue.
Professional Treatments by Cause
When home remedies are insufficient, professional treatment depends entirely on what is driving the pain.
| Cause | Professional Treatment |
|---|---|
| Strep throat | 10-day course of penicillin or amoxicillin |
| Tonsillitis (chronic) | Tonsillectomy for recurrent or severe cases |
| Oral thrush | Nystatin oral suspension or fluconazole tablets |
| HSV cold sores | Antiviral medication — aciclovir or valaciclovir |
| Dental abscess | Root canal therapy or tooth extraction |
| GERD | Proton pump inhibitors, H2 blockers, lifestyle changes |
| Sinusitis (bacterial) | Antibiotics, nasal steroids, saline irrigation |
| Nutritional deficiency | Targeted supplementation — B12, iron, folate |
| Ill-fitting appliances | Dental adjustment or refitting |
| Oral cancer (suspected) | Biopsy, specialist referral, oncology assessment |
| Peritonsillar abscess | Emergency drainage and IV antibiotics |
| Burning mouth syndrome | Topical clonazepam, antidepressants, cognitive therapy |
The most important rule: if you have already tried home management for 7 to 10 days and the pain has not improved, stop waiting and see a professional. The cause will not diagnose itself.
The Role of the Epiglottis in Swallowing Pain
One cause that is less commonly discussed but important to mention is epiglottitis — inflammation of the epiglottis, the flap of tissue that closes over the airway during swallowing.
When the epiglottis is inflamed, the pain spreads to the entire back of the mouth including the soft palate, creating a confusing picture that can mimic tonsillitis or strep throat. Unlike those conditions, epiglottitis also causes a muffled or changed voice, drooling, significant difficulty swallowing even fluids, and stridor (a high-pitched breathing sound).
Epiglottitis is a medical emergency. If you suspect it, go to the emergency department without delay. It can progress to complete airway obstruction rapidly.
Peritonsillar Abscess
A peritonsillar abscess (quinsy) is a collection of pus that forms in the tissue beside the tonsil, usually as a complication of untreated tonsillitis or strep throat. It causes extreme one-sided throat and palate pain, severe difficulty swallowing, a muffled “hot potato” voice, fever, and the uvula visibly pushed to one side.
This is a dental and medical emergency. The abscess must be drained by a clinician — it will not resolve on its own, and the swelling can progress to threaten the airway. If you notice these symptoms, do not wait until the next day to seek help.
When It Could Be Oral Cancer
Persistent pain in the roof of the mouth, particularly pain that has not improved after two weeks and is accompanied by any of the following, warrants an urgent professional evaluation:
A sore or ulcer on the palate that does not heal within two weeks. A white patch (leukoplakia) or red patch (erythroplakia) that was not previously present. A lump, thickening, or hard raised area in the mouth. Unexplained numbness in any part of the mouth or lips. Difficulty moving the tongue or jaw. Unexplained weight loss alongside mouth pain.
Oral cancer is most treatable when caught at an early stage. Most palate pain is not oral cancer — but dismissing persistent symptoms without professional evaluation carries unnecessary risk. If you are in any doubt, make the appointment.
Burning Mouth Syndrome
Burning mouth syndrome (BMS) is a chronic pain condition characterised by a persistent burning sensation on the tongue, palate, lips, or throughout the entire mouth, often without any visible cause.
It is more common in post-menopausal women and is linked to nerve dysfunction, hormonal changes, nutritional deficiencies, and anxiety. The burning sensation is typically worse throughout the day and may be temporarily relieved by eating or drinking. Treatment is challenging and may involve topical clonazepam, low-dose antidepressants, alpha-lipoic acid supplementation, and cognitive behavioural therapy for the pain component.
How Long Should Roof of Mouth Pain When Swallowing Last?

The timeline varies dramatically depending on the cause.
| Cause | Expected Duration |
|---|---|
| Thermal burn (minor) | 3 to 7 days |
| Canker sore | 7 to 14 days |
| Viral throat infection | 7 to 10 days |
| Strep throat (with antibiotics) | 2 to 4 days after starting treatment |
| Oral thrush (with treatment) | 7 to 14 days |
| HSV outbreak | 7 to 10 days |
| Sinus infection | 10 to 21 days (longer if bacterial) |
| Dental abscess | Does not resolve without treatment |
| GERD-related irritation | Weeks to months if untreated |
| Burning mouth syndrome | Chronic; ongoing management needed |
If your pain has lasted longer than its expected duration — or if it is getting worse rather than better — professional evaluation is necessary regardless of how mild it started.
Prevention: How to Protect the Roof of Your Mouth
Many causes of palate pain are avoidable with consistent habits.
Let hot food cool before eating. Give pizza, soup, and hot drinks 2 to 3 minutes before putting them in your mouth. The majority of palate burns are entirely preventable.
Use a soft toothbrush and gentle technique. Hard bristles and aggressive brushing can scratch the palate, particularly near the gum line of the upper teeth.
Maintain excellent oral hygiene. Daily brushing, flossing, and antibacterial mouth rinse use reduce bacterial populations that cause gum disease, dental abscesses, and oral infections.
Manage GERD proactively. Avoiding known reflux triggers — late meals, lying down after eating, alcohol, caffeine — reduces acid exposure to the throat and palate.
Stay up to date with dental checkups. Regular professional examinations catch dental abscesses, early gum disease, and suspicious tissue changes before they become serious problems.
Address nutritional deficiencies. If you are prone to recurrent mouth sores, ask your doctor to test your B12, iron, and folate levels at your next physical.
Replace dental appliances when they wear or shift. Dentures, retainers, and night guards that no longer fit correctly should be adjusted promptly rather than worn until damage occurs.
When to See a Doctor vs. a Dentist
Knowing which professional to contact helps you get the right diagnosis and treatment faster.
| Situation | Who to See |
|---|---|
| Severe sore throat, white patches, fever | Doctor or urgent care — likely strep or tonsillitis |
| Minor burn or canker sore, improving | Manage at home; see dentist if no improvement in 10 days |
| White or creamy patches on palate | Doctor — possible oral thrush |
| One-sided throat swelling | Emergency department — possible peritonsillar abscess |
| Pain near upper tooth, worse when biting | Dentist — possible dental abscess |
| Sore or patch not healed after 2 weeks | Dentist — oral cancer screening |
| GERD-related burning, chronic | Doctor — GI evaluation and treatment |
| Ill-fitting dentures or braces causing pain | Dentist — appliance adjustment |
| Difficulty breathing or swallowing fluids | Emergency department immediately |
Never hesitate to seek care when symptoms feel serious. Both dentists and doctors can perform an initial assessment of palate pain and refer you to the appropriate specialist if needed.
Frequently Asked Questions (FAQs)
Why does the roof of my mouth hurt only when I swallow?
The soft palate moves every time you swallow. When it is inflamed from an infection, sore, or irritation, that movement triggers pain. Strep throat, tonsillitis, and soft palate ulcers are the most common reasons.
Can a sinus infection make the roof of my mouth hurt when swallowing?
Yes. The sinuses sit directly above the palate and press downward when infected. The pain often accompanies nasal congestion and facial pressure, and it clears once the sinus infection is resolved.
How long will roof of mouth pain when swallowing last?
Minor burns and canker sores heal within 7 to 14 days. Strep throat resolves in 2 to 4 days with antibiotics. Any pain lasting beyond two weeks without improvement needs professional evaluation.
What does it mean if the back of my palate hurts when I swallow?
Pain at the back of the palate during swallowing is most commonly linked to the soft palate or tonsils. Strep throat, tonsillitis, peritonsillar abscess, or a viral infection are the most likely causes.
Can acid reflux cause the roof of my mouth to hurt?
Yes. Stomach acid that reaches the back of the throat can irritate and inflame the soft palate. GERD-related palate pain typically feels like a burning sensation and worsens after meals or when lying down.
Is it normal for the roof of my mouth to hurt after eating hard food?
Yes. Chips, crusty bread, crackers, and similar hard foods can scratch the palate tissue. The resulting soreness during swallowing typically resolves within 3 to 5 days with soft foods and saltwater rinses.
Can dry mouth cause pain in the roof of my mouth when swallowing?
Yes. Without adequate saliva, the palate loses its protective moisture layer. Swallowing becomes a dry, friction-heavy movement that irritates the tissue and can cause or worsen soreness.
When should I be worried about roof of mouth pain?
See a doctor or dentist if pain has lasted more than 10 to 14 days, you have a fever, there is visible swelling or white patches, you have difficulty swallowing liquids, or you notice a sore or lump that is not healing.
Can stress cause the roof of my mouth to hurt?
Stress does not directly injure the palate, but it is a well-established trigger for canker sores, HSV outbreaks, and bruxism — all of which can cause palate pain. Managing stress reduces the frequency of these flare-ups significantly.
How do I soothe roof of mouth pain when swallowing at home?
Warm saltwater rinses, cold water, soft bland foods, topical anaesthetic gel, honey applied to sores, and staying well hydrated are the most effective home measures. Avoid spicy, acidic, crunchy, or very hot foods until the pain resolves.
Conclusion
Why does the roof of my mouth hurt when I swallow is a question with many possible answers — from the completely harmless to the genuinely urgent. A thermal burn from hot pizza, a canker sore on the soft palate, or a minor scratch from a sharp food are by far the most common culprits, and they all resolve on their own with basic home care within one to two weeks. Infections like strep throat, oral thrush, and sinusitis are the next most frequent causes, and they respond well to appropriate medical or dental treatment.
The key is paying attention to how your pain behaves over time. Pain that improves day by day, follows a known minor cause, and stays manageable is almost always benign. Pain that worsens, spreads, produces visible lesions or swelling, comes with fever, or persists beyond two weeks is your body signalling that something more needs attention.
Start with home remedies when appropriate. Move to professional care without delay when the warning signs appear. Your palate is one of the most active tissues in your body — protect it, treat it promptly when something is wrong, and it will heal well.






