Why Does the Roof of My Mouth Hurt While Swallowing? 2026
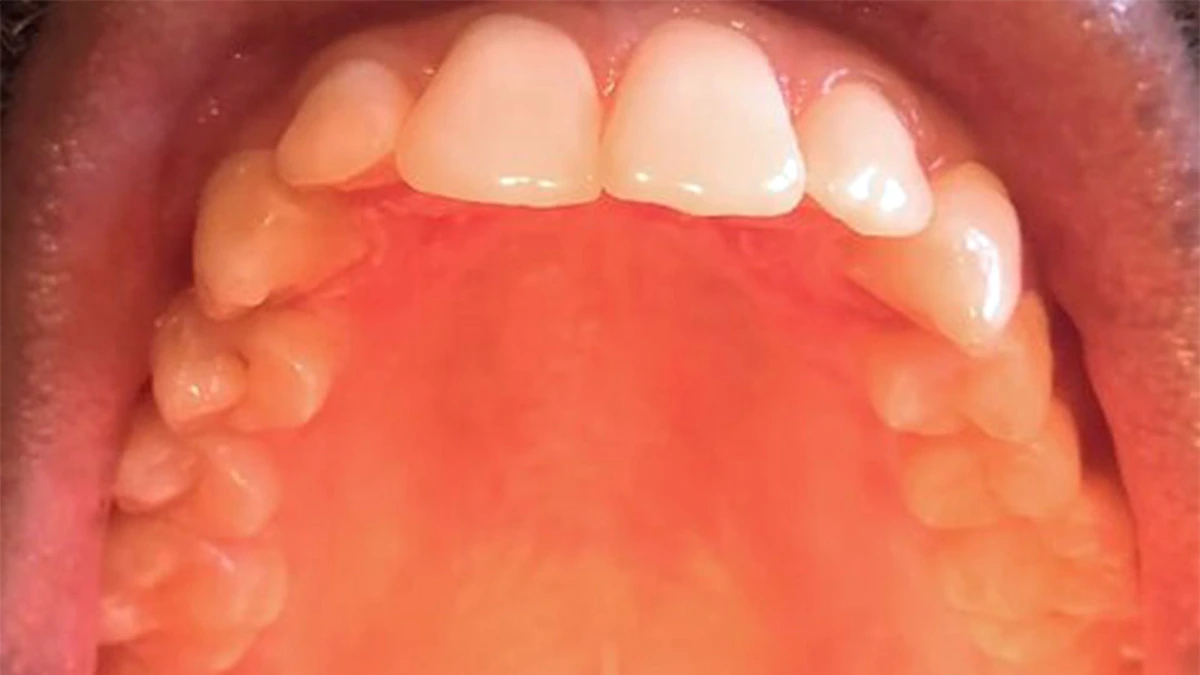
Why does the roof of my mouth hurt Is one of the most commonly searched dental questions in 2026, and the answer depends entirely on which part of your palate is affected and when the pain appears.
The roof of your mouth, called the palate, is divided into two sections: the hard palate at the front and the soft palate at the back.
Both are covered with delicate tissue that reacts quickly to heat, sharp food, infection, and inflammation.
When pain appears specifically while swallowing, the soft palate is almost always involved.
Hard Palate vs. Soft Palate: Understanding the Anatomy
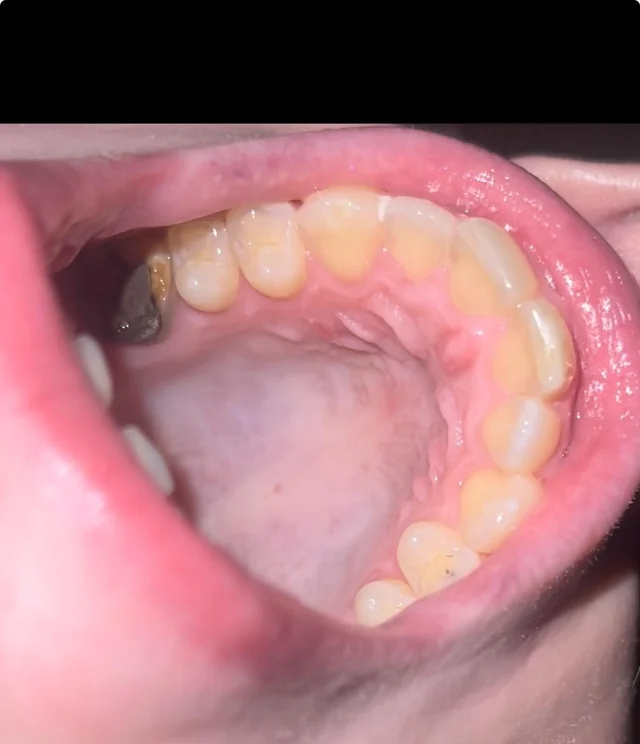
Before identifying the cause of your pain, it helps to understand exactly what the roof of your mouth is made of and what each part does.
The hard palate is the firm, bony section you can feel with your tongue right behind your upper teeth. It is covered with a thin layer of mucous membrane. This section bears most of the contact with food during chewing.
The soft palate sits at the back of your mouth. It is flexible, muscular, and moves actively during swallowing to close off the nasal passages and direct food toward the throat. Because it moves constantly, even mild inflammation here causes noticeable pain during every swallow.
| Palate Section | Location | Main Function | Pain Trigger |
|---|---|---|---|
| Hard palate | Front two-thirds | Supports chewing, speech | Burns, cuts, sores, appliance pressure |
| Soft palate | Back one-third | Guides swallowing, closes nasal passage | Infections, inflammation, sinus issues |
Understanding which section hurts helps you and your dentist narrow down the cause much faster.
Why Does the Roof of My Mouth Hurt: 13 Most Common Causes
1. Thermal Burns from Hot Food or Drinks (Pizza Burn)
This is the single most common reason the roof of your mouth hurts. Hot coffee, soup, pizza straight from the oven, and freshly toasted bread can scald the delicate mucous membrane on the hard palate almost instantly.
The burn is so common with pizza specifically that it is nicknamed “pizza burn” in dental circles. The cheese retains heat far longer than it appears to, causing a deep burn that is not always felt until seconds later.
A burned palate typically heals fully within three to seven days. Cooling your food and drinks before eating is the simplest and most effective prevention available.
2. Physical Injury or Trauma
Hard or sharp foods scratch and cut the soft tissue on the roof of your mouth frequently. Tortilla chips, crusty baguettes, crackers, pretzels, and hard candy are the most common culprits.
You may not feel the scratch immediately during eating, but discomfort builds over the following hours as the irritated area becomes inflamed. These small injuries typically heal within two to three days.
Dental appliances like braces, retainers, ill-fitting dentures, and night guards can also rub against the palate over time, creating chronic irritation, sores, and pressure points that do not heal until the appliance is adjusted.
3. Canker Sores (Aphthous Ulcers)
Canker sores are small, shallow, painful ulcers that form on the soft tissue inside the mouth, including the roof. They appear as round or oval lesions with a white or yellow center and a red border around the edge.
They are not contagious and are not caused by any virus. Known triggers include stress, hormonal changes, minor mouth injuries, immune responses, and nutritional deficiencies in vitamin B12, iron, or folate.
Most canker sores heal on their own within seven to ten days. If a sore persists beyond two weeks, grows larger, or is accompanied by fever, professional evaluation is strongly recommended.
4. Cold Sores (Herpes Simplex Virus)
Cold sores are caused by the herpes simplex virus type 1 (HSV-1) and, unlike canker sores, are contagious. They typically appear on or around the lips but can also develop on the hard palate inside the mouth.
When cold sores appear on the roof of the mouth, they create painful blisters or small clusters of sores that make eating and swallowing uncomfortable. They are often preceded by a tingling or burning sensation in the area before the sores visibly appear.
Triggers include stress, fatigue, illness, sun exposure, and any change in immune function. Topical or oral antiviral medications reduce severity and healing time significantly when started at the first sign of symptoms.
5. Oral Thrush (Candida Yeast Infection)
Oral thrush is a fungal infection caused by the overgrowth of Candida albicans, a yeast naturally present in the mouth. When it overgrows, it creates raised, creamy white or pale yellow patches on the tongue, cheeks, and roof of the mouth.
These patches can bleed when scraped, cause a burning or sore sensation, and interfere with taste perception. Thrush on the soft palate specifically causes pain and discomfort when swallowing because the tissue moves during each swallow.
People who wear dentures, use corticosteroid inhalers, take antibiotics, or have weakened immune systems are at highest risk. Treatment requires prescription antifungal medication in the form of a liquid rinse, gel, or oral tablet.
6. Sinus Infection and Sinus Pressure
The maxillary sinuses sit very close to the roof of the mouth, separated by only a thin layer of bone in the hard palate region. When sinuses become infected or inflamed, that pressure pushes downward and creates referred pain in the palate.
Sinus-related palate pain is usually felt as a dull, widespread ache rather than a sharp, localized pain. It typically worsens when you bend forward, lean over, or jump, because the movement shifts the sinus fluid.
You will usually have accompanying nasal congestion, facial heaviness, postnasal drip, or a general feeling of pressure behind the cheekbones. Treating the sinus infection or allergy with decongestants resolves the palate pain without any dental treatment needed.
7. Acid Reflux (GERD)
Gastroesophageal reflux disease causes stomach acid to travel upward into the throat and sometimes reach the back of the oral cavity. The soft palate, being at the back of the mouth, is directly exposed to this acid during reflux episodes.
Chronic acid exposure erodes the delicate mucous membrane lining the soft palate, causing burning, soreness, and sensitivity that is especially noticeable during swallowing. Many people do not connect their palate pain to reflux without medical guidance.
If the roof of your mouth consistently hurts in the morning or after meals, especially accompanied by a sour or bitter taste in the mouth, acid reflux should be investigated as a primary cause alongside dental evaluation.
8. Dry Mouth (Xerostomia)
Dry mouth occurs when the salivary glands do not produce enough saliva to keep the mouth properly moist. Saliva provides a protective coating over oral tissues, maintains the pH balance, and prevents the build-up of irritating bacteria and fungi.
Without adequate saliva, the palate becomes dry, fragile, and more vulnerable to irritation, sores, burning sensations, and fungal infections like thrush. Many common medications including antihistamines, antidepressants, diuretics, and blood pressure drugs list dry mouth as a side effect.
Dehydration, mouth breathing, alcohol consumption, and smoking all reduce saliva production significantly. Staying well hydrated, using alcohol-free mouthwash, and chewing sugar-free gum stimulates saliva flow and reduces palate soreness.
9. Burning Mouth Syndrome
Burning mouth syndrome is a chronic, complex condition characterized by a persistent burning or scalding sensation in the mouth, including the roof, with no visible cause or injury. It can affect the tongue, lips, cheeks, and palate simultaneously.
The exact cause is not always identified. Possible contributors include nerve damage, hormonal changes in menopause, vitamin deficiencies, anxiety disorders, and certain medications. It predominantly affects middle-aged and older women.
The burning is often described as feeling like you have just scalded the inside of your mouth with hot liquid, but no burn is actually present. Managing the condition requires identifying any underlying triggers and working with both a dentist and a physician for combined care.
10. Dental Abscess with Referred Pain
A dental abscess is a bacterial infection at the root of a tooth or in the surrounding gum tissue. While the abscess itself sits near the tooth, the pain and inflammation can radiate upward and be felt throughout the hard palate.
You may feel tenderness, pressure, or a throbbing ache on the roof of your mouth near a specific upper tooth without immediately recognizing the tooth as the source. This referred pain pattern makes dental abscesses easy to misidentify as a palate problem.
Associated signs include a foul or salty taste in the mouth, visible swelling near the gumline, fever, a small pimple-like bump on the gum, and extreme sensitivity to hot and cold temperatures in the affected tooth.
11. Nutritional Deficiencies
Deficiencies in specific vitamins and minerals make the oral tissues significantly more prone to irritation, sores, burning, and inflammation. The most common nutritional gaps that affect the palate are vitamin B12, folate, iron, and vitamin C.
These deficiencies reduce the mucous membrane’s ability to repair itself after minor injuries and lower the immune response that normally keeps oral bacteria and fungi in check. The result is more frequent canker sores, longer healing times, and chronic palate soreness.
Eating a balanced diet rich in leafy greens, lean proteins, dairy products, and fortified cereals addresses most common deficiencies. Supplementation may be necessary if dietary intake is inadequate or absorption is impaired.
12. Palatal Cysts and Growths
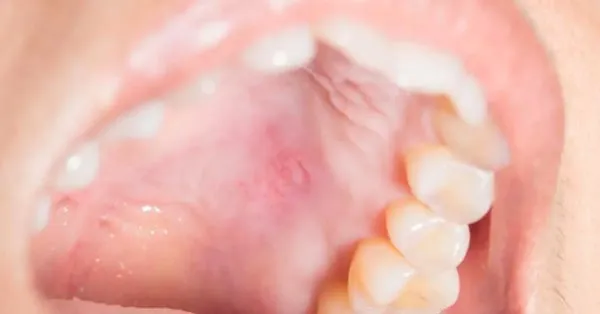
Palatal cysts are fluid-filled sacs that form in the tissue of the hard or soft palate. They are usually benign and may go unnoticed until they grow large enough to cause pressure or discomfort during eating or swallowing.
Squamous papillomas are small, non-cancerous wart-like growths caused by the human papillomavirus (HPV). They are typically painless but can become irritated and sore when repeatedly scraped or bitten during normal chewing.
Any persistent lump, bump, or growth on the roof of your mouth that does not resolve within two weeks requires professional evaluation. While most palatal growths are benign, early examination rules out more serious conditions.
13. Oral Cancer
Oral cancer is the least common but most serious cause of persistent palate pain. It can appear on the hard or soft palate as a sore that does not heal, a red or white patch, a lump, thickening of the tissue, or unexplained bleeding.
According to the American Cancer Society, oral cancer is most treatable when caught at an early stage. Risk factors include tobacco use, heavy alcohol consumption, HPV infection, prolonged sun exposure to the lips, and a history of oral cancer.
Any sore, patch, or growth on the roof of your mouth that persists beyond two weeks without improvement must be evaluated by a dentist or oral surgeon immediately for a definitive diagnosis and biopsy if necessary.
Symptom and Cause Comparison Table
| Cause | Type of Pain | Pain Location | Key Additional Symptoms |
|---|---|---|---|
| Thermal burn | Sharp, raw, stinging | Hard palate, front | Peeling tissue, raw surface |
| Physical injury | Stinging, tender | Where cut occurred | Visible scratch or cut |
| Canker sore | Burning, tender | Any area of palate | Round white/yellow ulcer with red border |
| Cold sore | Tingling then burning | Hard palate | Blisters, preceded by tingling |
| Oral thrush | Burning, diffuse | Soft and hard palate | White creamy patches, taste change |
| Sinus infection | Dull, widespread | Upper palate | Congestion, facial pressure, postnasal drip |
| Acid reflux | Burning, worse after meals | Soft palate, back | Sour taste, morning worsening |
| Dry mouth | Constant, mild burning | Entire palate | Sticky sensation, frequent thirst |
| Burning mouth syndrome | Persistent burning | Tongue and palate | No visible cause, worsens through day |
| Dental abscess | Throbbing, pressure | Near a specific tooth | Gum swelling, fever, bad taste |
| Nutritional deficiency | Soreness, frequent sores | Any oral tissue | Fatigue, frequent canker sores |
| Palatal cyst/growth | Pressure, mild pain | Specific bump location | Visible bump or mass |
| Oral cancer | Persistent, worsening | Any location | Non-healing sore, bleeding, numbness |
Why the Roof of My Mouth Hurts Specifically While Swallowing
Swallowing-specific pain is an important clue because it narrows the likely cause significantly. The soft palate is the key structure involved in every swallow it lifts, tenses, and presses against the back of the throat to prevent food and liquid from entering the nasal cavity.
Any condition that inflames or irritates the soft palate will produce pain specifically during swallowing. This includes oral thrush on the soft palate, cold sores at the back of the mouth, sinus drainage irritating the soft palate tissue, acid reflux reaching the back of the oral cavity, and strep throat or tonsillitis radiating into the soft palate.
If you feel pain primarily when swallowing and not when your mouth is at rest, the soft palate or throat is almost certainly the area that needs examination rather than the hard palate at the front.
Pain on the Back of the Roof of the Mouth
Pain specifically at the very back of the roof of your mouth while swallowing most commonly points to soft palate inflammation, throat infection, or postnasal drip from a sinus condition. This location is also more susceptible to acid reflux damage than the hard palate.
Strep throat, tonsillitis, and mononucleosis can all cause pain that is felt in the back of the roof of the mouth even when the primary infection is in the throat. If swallowing pain is severe, comes on rapidly, or is accompanied by a high fever, seek medical attention the same day.
Pain on the Hard Palate Front Section
Pain focused at the front section of the palate near your teeth is most commonly caused by burns, cuts, canker sores, cold sores, or pressure from dental appliances. These causes are all localized and do not typically worsen during swallowing.
A tooth infection in one of the upper front or back teeth can also produce referred pain directly in the hard palate tissue above that tooth. Tapping gently on the suspect tooth often reproduces the pain and helps identify the dental source.
Home Remedies for Roof of Mouth Pain
These remedies provide effective temporary relief while the cause heals naturally or while you wait for a dental or medical appointment.
Saltwater rinse. Mix one teaspoon of salt into a cup of warm water. Swish gently for 30 seconds and spit. Repeat two to three times daily. Saltwater reduces inflammation, gently cleans the affected area, and creates an environment less hospitable to bacteria and fungi.
Cold water or ice chips. Immediately after a burn, rinsing with cold water reduces the heat in the tissue and limits damage. Sucking gently on ice chips provides ongoing relief for burns, cuts, and canker sores without causing additional trauma.
Over-the-counter topical gels. Products containing benzocaine temporarily numb the sore area and reduce pain during eating. Apply a small amount directly to the sore using a cotton swab and follow label instructions carefully regarding frequency of use.
Soft, cool diet. Switch to foods like yogurt, smoothies, mashed potatoes, scrambled eggs, and oatmeal while your palate heals. These foods do not scrape, scratch, or deliver heat to the already-irritated tissue, allowing faster recovery.
Desensitizing mouthwash. Alcohol-free mouthwashes containing aloe vera or chamomile soothe inflamed tissue without the additional burning that alcohol-based products cause on already-sore oral mucosa.
Stay well hydrated. Drinking enough water maintains saliva flow, which coats and protects the palate tissue. Dehydration allows the mucous membrane to dry out, increasing sensitivity and slowing the healing of any existing sores or burns.
Avoid triggers. Stay away from spicy foods, acidic foods like citrus and tomatoes, very salty foods, carbonated drinks, and alcohol until the palate has fully healed. All of these are direct irritants that significantly slow recovery.
Professional Treatment Options by Cause
| Cause | First-Line Professional Treatment | Additional Options |
|---|---|---|
| Severe burn | Prescription mouth rinse, analgesic gel | Observation, soft diet guidance |
| Persistent canker sores | Topical steroid, prescription lidocaine | Cauterization for recurring sores |
| Cold sores | Oral antiviral (acyclovir, valacyclovir) | Topical antiviral cream |
| Oral thrush | Antifungal rinse or tablet (nystatin, fluconazole) | Denture adjustment if applicable |
| Sinus infection | Antibiotics or decongestants | Referral to ENT specialist |
| Acid reflux | Proton pump inhibitors, H2 blockers | Dietary modification plan |
| Dental abscess | Root canal and antibiotics | Extraction if tooth unsalvageable |
| Dry mouth | Saliva substitutes, medication review | Prescription saliva stimulants |
| Burning mouth syndrome | Clonazepam, tricyclic antidepressants | Cognitive behavioral therapy |
| Palatal cyst/growth | Surgical removal or biopsy | Monitoring for benign growths |
| Oral cancer | Surgical resection, radiation, chemotherapy | Multidisciplinary oncology team |
When to See a Dentist or Doctor
Not every instance of palate pain requires an urgent visit, but specific symptoms always warrant same-day or next-day professional care.
See a dentist or doctor immediately if your palate pain is accompanied by high fever. Fever alongside oral pain strongly suggests an active infection that may be spreading beyond the oral cavity.
Get professional evaluation urgently if you notice facial swelling, especially around the cheeks, jaw, or neck. Swelling in these areas indicates that an infection has moved into deeper tissue planes, which can become dangerous rapidly.
Seek care without delay if you have a sore, patch, or lump on the roof of your mouth that has not healed or changed in two weeks. The two-week rule is the standard guideline for screening suspicious oral lesions for cancer.
For mild, clearly identifiable causes like a burn or small canker sore, schedule a routine appointment within the next week if home remedies are not providing adequate relief within five to seven days.
Warning Signs That Require Urgent Attention
Some symptoms alongside roof of mouth pain should never be waited out at home. Recognizing them early can make a critical difference in outcomes.
Difficulty swallowing that worsens rapidly over hours, pain that radiates into the ear and throat simultaneously, or any swelling that makes breathing feel restricted all require emergency medical evaluation rather than a dental appointment.
A sore on the roof of your mouth that bleeds without being touched, grows in size, or develops a hard raised edge underneath the tissue should be examined by an oral surgeon or dentist trained in oral cancer screening as soon as possible.
How to Prevent Roof of Mouth Pain
Preventing the most common causes of palate pain is straightforward with consistent daily habits that protect the delicate tissue lining the roof of your mouth.
Let hot food and drinks cool adequately before eating or drinking. The most effective prevention for the most common cause of palate pain costs nothing and takes only one minute of patience before every hot meal.
Brush gently with a soft-bristled toothbrush and avoid pressing the brush against the palate with force. Aggressive brushing irritates the mucous membrane and can create chronic low-grade soreness over time.
Maintain thorough daily oral hygiene including brushing twice, flossing once, and using an alcohol-free mouthwash. This keeps bacterial and fungal populations in check and reduces the risk of infections developing on the palate.
Manage stress through regular exercise, adequate sleep, and relaxation practices. Stress is a well-documented trigger for both canker sores and cold sore recurrences, which are two of the most frequent causes of palate pain.
Get enough vitamin B12, folate, and iron through your diet or supplementation. Deficiencies in these nutrients directly weaken oral tissue integrity and immune responses that protect the palate from repeated sores.
See your dentist at least every six months for professional cleanings and examinations. Routine checkups identify ill-fitting dental appliances, early gum disease, failing restorations, and suspicious oral lesions before they cause significant pain.
Roof of Mouth Pain in Children vs. Adults
Children commonly experience palate pain from burns and cuts during eating, teething irritation in younger children, and hand-foot-and-mouth disease, a viral illness that causes blisters throughout the oral cavity including the palate.
Children with persistent palate sores, difficulty eating, or unexplained fever alongside oral pain should be seen by a pediatric dentist or pediatrician promptly. Do not attempt to pop or scrape blisters inside a child’s mouth.
In older adults, palate pain is more commonly associated with ill-fitting dentures, dry mouth from medications, nutritional deficiencies related to diet changes, and chronic conditions like acid reflux and diabetes that compromise tissue healing.
The Connection Between Palate Pain and Overall Health
Recurring, unexplained palate pain is not always purely a dental problem. It can signal systemic health conditions including autoimmune diseases such as lupus and Crohn’s disease, both of which are associated with increased frequency and severity of oral ulcers.
Diabetes impairs the immune system and reduces the body’s ability to fight oral infections, making thrush, persistent canker sores, and slow-healing wounds more likely in people with poorly controlled blood sugar levels.
If you experience frequent, recurrent palate pain without an obvious cause, mentioning it to your primary care physician as well as your dentist ensures that no systemic health condition is being overlooked alongside the oral symptoms.
Palate Pain During Pregnancy

Hormonal changes during pregnancy significantly increase the risk of canker sores, gum inflammation, and sensitivity throughout the oral cavity including the roof of the mouth. Morning sickness and acid reflux are also very common in the first trimester and can cause direct soft palate irritation from repeated acid exposure.
Pregnant women should maintain their regular dental visits, inform their dentist of their pregnancy at every appointment, and avoid any over-the-counter medications including oral numbing gels without first checking with their obstetrician about safety during pregnancy.
What Normal Roof of Mouth Should Look and Feel Like
A healthy palate should be smooth, moist, consistently pink in color, and entirely painless during eating, swallowing, and speaking. The hard palate has natural ridges near the front called rugae, which are normal anatomical features.
Any deviation from these normal characteristics including white patches, red patches, lumps, persistent dryness, bleeding spots, or ulcers that do not heal should be documented and reported to a dental professional promptly.
Running your tongue lightly across the roof of your mouth during your daily oral hygiene routine is a simple habit that helps you catch any early changes before they develop into more significant problems.
Frequently Asked Questions (FAQs)
Why does the roof of my mouth hurt while swallowing?
Swallowing-specific pain usually means the soft palate is inflamed from an infection, sinus drainage, oral thrush, acid reflux, or a cold sore. The soft palate moves actively during every swallow, so any inflammation causes immediate pain.
Is roof of mouth pain always serious?
No. Most cases are caused by minor burns, cuts, or canker sores that heal on their own within three to ten days. Pain that persists beyond two weeks or comes with fever and swelling does require professional evaluation.
Can a sinus infection cause roof of mouth pain?
Yes. The sinus cavities sit very close to the upper palate. Sinus inflammation pushes downward and creates a dull, widespread ache across the hard palate that typically goes away once the sinus infection is treated.
What does oral thrush look like on the roof of the mouth?
Oral thrush appears as raised, creamy white or pale yellow patches on the palate. These patches can be scraped off but may bleed slightly, and they cause a burning or sore sensation, especially during swallowing.
How long does a burned roof of mouth take to heal?
A burned palate from hot food or drinks typically heals completely within three to seven days. Rinsing with cold water immediately after the burn, staying hydrated, and eating only soft, cool foods speeds up the healing process.
Can acid reflux cause the roof of my mouth to hurt?
Yes. Stomach acid reaching the back of the oral cavity directly irritates the soft palate tissue. Reflux-related palate pain is often worse in the morning or after eating and is usually felt as a burning sensation at the back of the mouth.
When should I worry about a sore on the roof of my mouth?
See a dentist or doctor if any sore, lump, or patch on the roof of your mouth has not healed within two weeks. Persistent oral sores can occasionally indicate oral cancer, which is most treatable when identified at an early stage.
Can stress cause roof of mouth pain?
Yes. Stress is a well-documented trigger for canker sores and cold sore recurrences. Both conditions cause direct palate pain. Reducing stress through sleep, exercise, and relaxation lowers the frequency of stress-triggered oral sores.
What foods should I avoid when the roof of my mouth hurts?
Avoid hot foods and drinks, spicy foods, acidic foods like citrus and tomatoes, hard crunchy foods like chips, and salty snacks. All of these irritate the inflamed palate tissue and significantly slow down the natural healing process.
Does dry mouth cause roof of mouth pain?
Yes. Without adequate saliva, the palate loses its protective coating and becomes dry, fragile, and prone to soreness, burning sensations, and fungal infections like oral thrush. Staying well hydrated is the simplest management strategy.
Conclusion
Understanding why does the roof of my mouth hurt is the essential first step toward getting the right relief, whether the cause is something as minor as a burn from hot pizza or as serious as an oral infection that needs professional treatment.
The roof of your mouth, divided into the hard palate at the front and the soft palate at the back, is constantly exposed to heat, sharp food edges, bacteria, fungi, and acid from daily life.
When pain appears specifically while swallowing, the soft palate is almost always the primary location affected.
Most causes of palate pain are benign, temporary, and respond well to simple home remedies like saltwater rinses, cold water, soft diets, and over-the-counter numbing gels.
However, pain that persists beyond two weeks, comes with swelling or fever, or appears as a growth that does not heal must always be evaluated by a dentist or doctor without delay.
Preventing palate pain starts with letting hot food cool before eating, brushing gently, staying well hydrated, and maintaining regular dental checkups twice a year.