Why Are My Feet Peeling? Is It a Fungal Infection? 2026
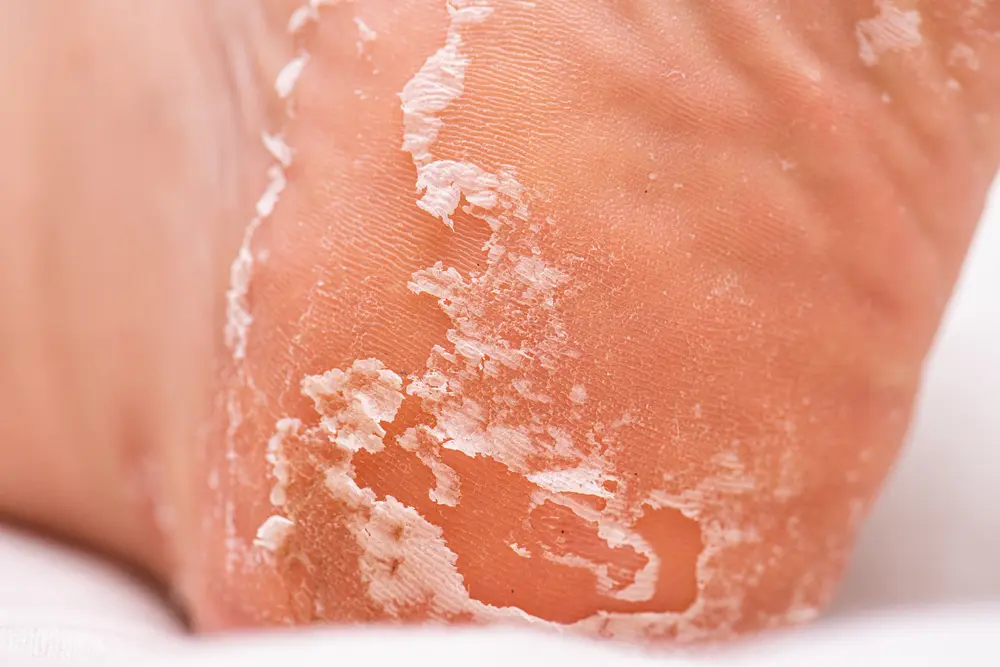
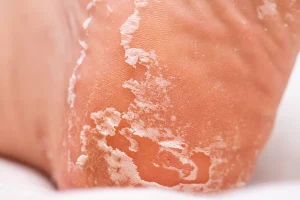
Why are my feet peeling — and is it something serious? If you have noticed flaky, cracked, or shedding skin on your feet, you are not alone.
Millions of people deal with peeling feet every year. The causes range from a simple fungal infection to dry skin, eczema, psoriasis, sunburn, or even dehydration. Knowing what is behind the peeling is the first step toward fixing it.
This guide breaks down every major cause, how to tell them apart, and exactly what to do about each one.
What Causes Feet to Peel? A Quick Overview
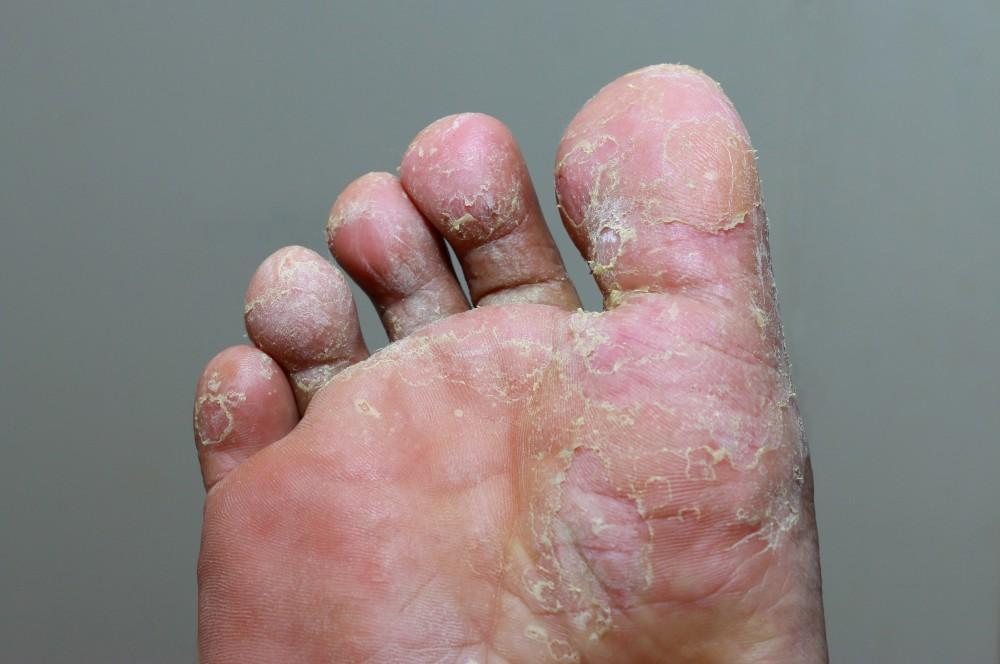
Your feet take a beating every single day. They are squeezed into tight shoes, exposed to sweat, friction, and sometimes harsh surfaces.
When the outer layer of skin breaks down, it sheds — and that shedding is what you see as peeling. The root cause determines how you treat it.
| Cause | Main Location | Key Symptom | Contagious? |
|---|---|---|---|
| Athlete’s Foot (Tinea Pedis) | Between toes, soles | Itch, burn, odor | Yes |
| Dry Skin (Xerosis) | Heels, soles | Flaking, tightness | No |
| Eczema | Anywhere on foot | Blisters, intense itch | No |
| Psoriasis | Soles, heels | Thick silvery scales | No |
| Hyperhidrosis | Between toes | White maceration, odor | No |
| Contact Dermatitis | Where shoe touches skin | Rash, redness | No |
| Sunburn | Top of foot | Redness, tenderness | No |
| Dehydration | General | Flaky, dull skin | No |
Athlete’s Foot — The Most Common Fungal Infection Behind Peeling Feet
Athlete’s foot, medically called tinea pedis, is one of the most common reasons your feet peel. It is a fungal infection caused by dermatophytes — fungi that feed on the keratin protein in your skin.
The fungus thrives in warm, moist environments. Locker rooms, public showers, swimming pool decks, and sweaty shoes are its favorite breeding grounds.
How Do You Catch Athlete’s Foot?
You can pick it up by walking barefoot on contaminated floors. Sharing socks, shoes, or towels with an infected person is another common route.
It also grows on your own feet if they stay hot and sweaty inside non-breathable shoes for hours at a time.
Where Does It Show Up First?
The infection typically starts in the web space between your fourth and fifth toes. From there it can spread to the soles, heels, and sides of the feet.
In the moccasin type, peeling covers the entire bottom of the foot and follows the edges like a sock pattern.
What Does Athlete’s Foot Feel and Look Like?
Symptoms include itching, burning, stinging, and skin that cracks or peels in thin sheets or fine flakes. The skin can turn white, red, or scaly.
In some cases, small fluid-filled blisters appear on the soles. A foul smell is also a common sign.
How to Treat Athlete’s Foot at Home
Over-the-counter antifungal creams containing clotrimazole, terbinafine, or miconazole are highly effective. Apply consistently for the full recommended period — usually 2 to 4 weeks — even after symptoms improve.
Keep your feet clean and completely dry, especially between the toes. Change socks daily and wear breathable footwear.
| OTC Antifungal | Active Ingredient | Form |
|---|---|---|
| Lotrimin AF | Clotrimazole | Cream, powder |
| Lamisil AT | Terbinafine | Cream, gel |
| Tinactin | Tolnaftate | Cream, spray, powder |
| Micatin | Miconazole | Cream, spray |
When to See a Doctor for Athlete’s Foot
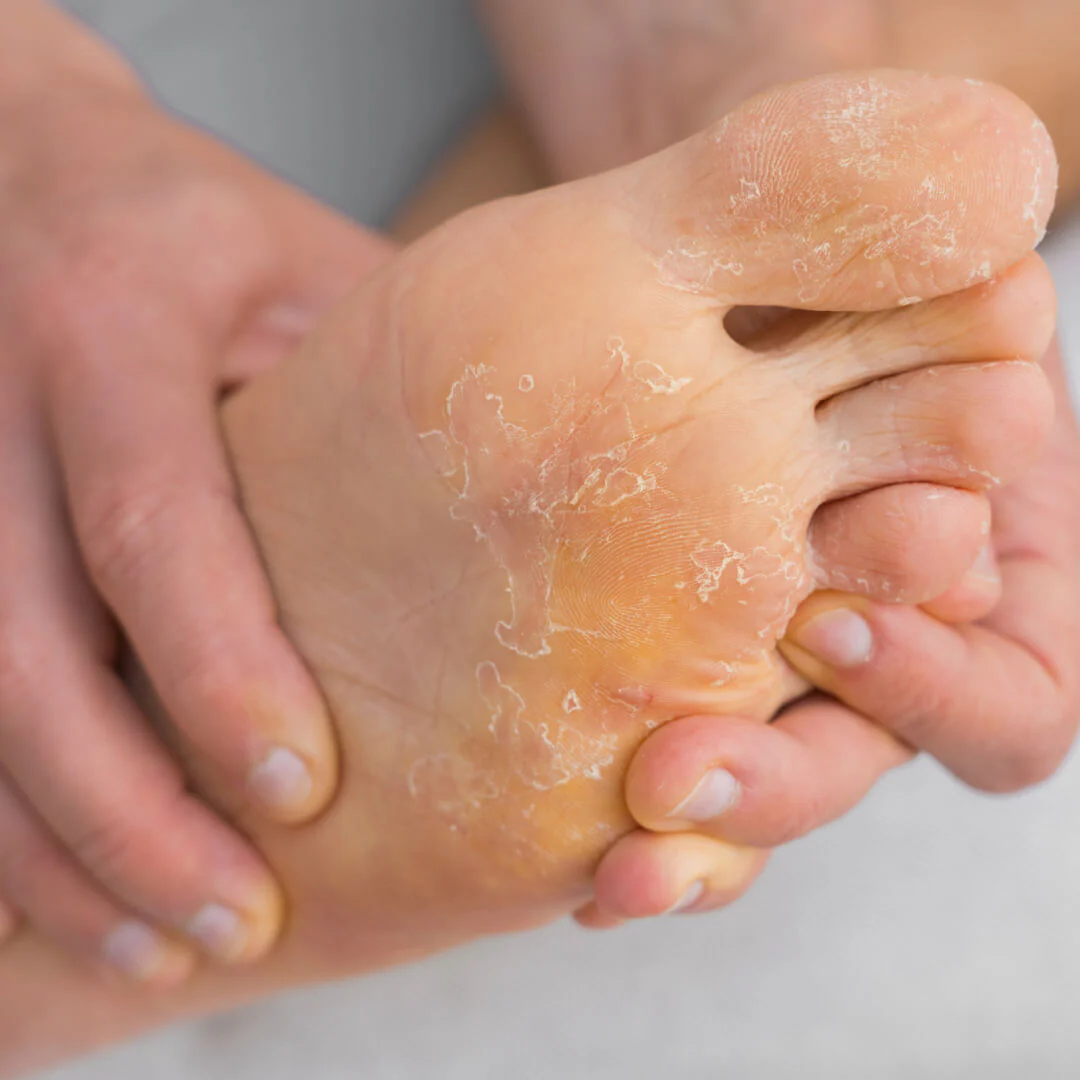
See a doctor if OTC treatment does not clear the infection within 4 weeks. Prescription oral antifungals may be needed for stubborn or widespread cases.
People with diabetes must see a provider promptly. Even a minor foot infection can escalate quickly in people with diabetes.
Dry Skin (Xerosis) — When Peeling Has Nothing to Do With Fungus
Dry skin, or xerosis, is one of the most straightforward causes of peeling feet. It has nothing to do with infection.
The outer skin layer simply lacks enough moisture to stay supple and intact. It dries out, stiffens, and then sheds.
Where Does Dry Skin Typically Peel?
Dry skin tends to concentrate on the heels, the balls of the feet, and the outer edge of the big toe. It does not usually cause intense itching or redness the way athlete’s foot does.
The skin may feel tight, rough, and scaly rather than burning or stinging.
What Makes Dry Skin Worse?
Hot showers strip the skin’s natural oils. Walking barefoot on hard floors adds friction. Low humidity, harsh soaps, and aging all reduce skin moisture.
Dehydration also plays a role — if your body is not getting enough water, your skin barrier suffers and peeling can follow.
How to Treat Dry, Peeling Feet
Apply a thick cream or ointment moisturizer right after bathing, when the skin is still slightly damp. Ointments lock in moisture better than lotions.
Apply at bedtime and put on cotton socks immediately after. This overnight method helps the product penetrate deeper into the skin layers.
Gentle exfoliation with a pumice stone two to three times per week helps remove dead skin buildup so moisturizer works better.
Eczema on Feet — When Your Immune System Triggers the Peeling
Eczema, or atopic dermatitis, is an inflammatory skin condition that can absolutely show up on your feet and toes. It is not contagious and is not caused by a fungus.
Triggers include allergens, heat, stress, sweat, and harsh skincare products. Flare-ups cause the top layer of skin to become red, itchy, and dry — then it peels.
Dyshidrotic Eczema — The Blister-First Type
Dyshidrotic eczema is a specific type that commonly affects the feet. It causes clusters of small, intensely itchy blisters on the soles and sides of the feet.
As those blisters heal, the skin cracks and peels. It can look a lot like athlete’s foot, but antifungal treatment will not help.
How to Tell Eczema Apart From Athlete’s Foot
Eczema does not have a foul smell. It tends to respond to hydrocortisone cream rather than antifungals. It often appears on other parts of the body too, like the elbows, knees, and hands.
If antifungal treatment has not worked after 2 to 4 weeks, eczema is a strong possibility.
Treatment for Eczema on Feet
Fragrance-free moisturizers and mild cleansers are the foundation of eczema management. Avoid hot water, harsh soaps, and synthetic fabrics.
A healthcare provider may prescribe topical corticosteroids or calcineurin inhibitors for persistent flares.
Psoriasis on Feet — Thick Scales That Peel in Sheets
Psoriasis is an autoimmune condition. When it affects the feet, it is called palmoplantar psoriasis. The immune system attacks healthy skin cells, causing rapid skin turnover.
The result is thick, red patches covered in silvery-white scales that can peel off in large sheets. It can also cause pain, soreness, and cracking that bleeds when you walk.
How Does Foot Psoriasis Differ From Other Causes?
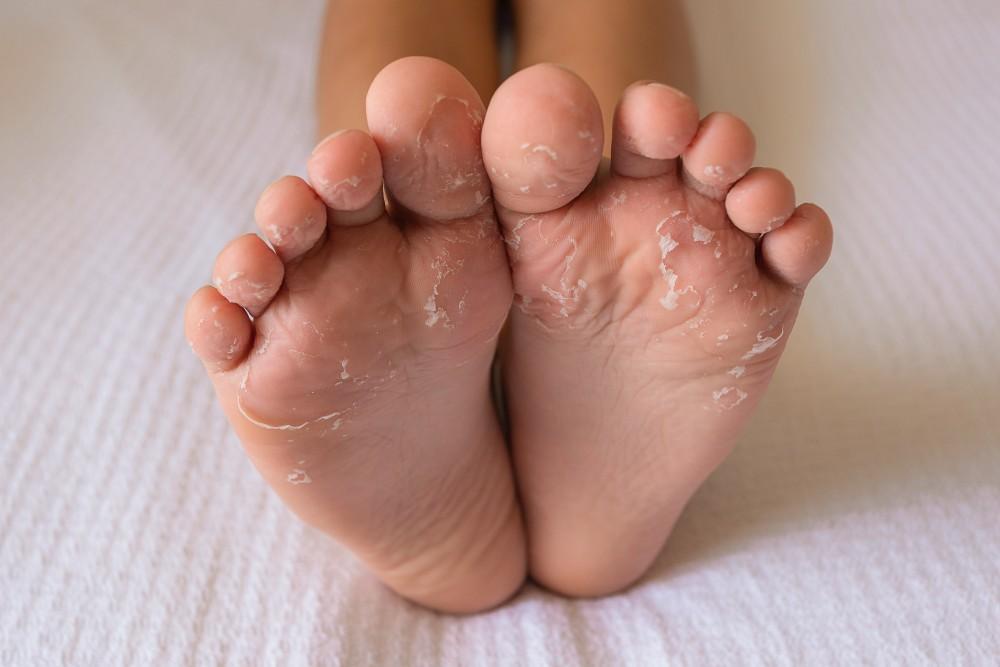
The scale pattern is distinctive — thick, layered, and silvery rather than thin and flaky. It typically affects the entire sole rather than just the toe spaces.
Psoriasis may also appear on the elbows, knees, scalp, and nails at the same time.
Treatment Options for Psoriasis
Prescription-strength topical creams are the first-line treatment. Phototherapy (controlled UV light exposure) is also effective.
For severe cases, oral or injectable biologics may be prescribed. Psoriasis requires ongoing management — there is no permanent cure, but symptoms can be well controlled.
Hyperhidrosis — When Excessive Sweating Causes Peeling
Hyperhidrosis means sweating excessively beyond what the body needs for temperature control. On the feet, this keeps the skin constantly damp inside shoes.
When moisture soaks into skin for hours, it breaks down the skin barrier. The waterlogged skin softens, macerates, and then peels — especially between the toes.
Signs That Sweat Is the Problem
The skin between the toes looks white, soft, and soggy rather than red and scaly. Odor and recurrent rashes may also accompany the peeling.
The pattern typically does not match athlete’s foot — it is more diffuse and appears after long periods inside shoes.
How to Manage Hyperhidrosis-Related Peeling
Breathable socks and moisture-wicking footwear are essential. Change socks when they feel damp. Antifungal powder inside shoes can help keep things dry and prevent secondary fungal overgrowth.
Severe cases may need prescription-strength aluminum chloride antiperspirant or other medical treatments.
Contact Dermatitis — When Your Shoes or Socks Are the Culprit
Contact dermatitis is a rash caused by skin contact with an irritant or allergen. On feet, the usual suspects include rubber or adhesives in shoes, synthetic sock materials, fragrance in foot creams, and laundry detergents.
The rash and peeling typically appear exactly where the skin touches the trigger — often the top of the foot or around the straps of sandals.
Irritant vs. Allergic Contact Dermatitis
Irritant contact dermatitis is a direct skin reaction to something harsh — like strong detergents or too much friction. It is not an immune reaction.
Allergic contact dermatitis is an immune response to a specific allergen. It may not appear on the first exposure but flares with repeated contact.
How to Treat Contact Dermatitis on Feet
Identify and eliminate the trigger. Switch to natural-fiber socks, hypoallergenic soaps, and fragrance-free products.
A mild hydrocortisone cream can reduce inflammation. Severe cases may need a prescription corticosteroid.
Sunburn on Feet — A Seasonal Cause of Sudden Peeling
Sunburn is a surprisingly common and often overlooked cause of peeling feet, particularly in summer. Many people carefully apply sunscreen to their face, arms, and legs — but forget the tops of their feet.
The result is red, tender, warm skin that starts to peel within a few days of the initial burn.
Who Is Most at Risk?
Anyone wearing sandals, flip-flops, or no shoes outdoors is at risk. The tops of the feet receive direct sun exposure that is easy to underestimate.
How to Treat and Prevent Sunburn on Feet
Apply a broad-spectrum sunscreen of SPF 30 or higher to the tops of your feet whenever wearing open shoes outdoors. A spray sunscreen makes it easier to reach the spaces between toes.
If sunburn has already occurred, keep the skin moisturized with aloe vera gel or a gentle lotion. Do not peel the skin manually — let it shed naturally.
Dehydration — The Overlooked Internal Cause
Your skin needs adequate internal hydration to stay healthy. If you are not drinking enough water, the skin barrier weakens and peeling can develop — including on the feet.
Dehydration-related peeling tends to appear as general dullness and flaking across the foot rather than in one targeted area.
Other Signs Your Skin May Be Dehydrated
You may notice dry lips, fatigue, and headache alongside the peeling skin. The skin on your hands may look similar.
Drinking more water and eating water-rich foods can improve skin hydration from the inside out. Topical moisturizers help from the outside.
How to Tell If Your Peeling Feet Are From a Fungal Infection or Something Else
This is one of the most common questions people ask. Here is a simple comparison:
| Feature | Fungal Infection | Dry Skin | Eczema | Psoriasis |
|---|---|---|---|---|
| Location | Between toes, soles | Heels, soles | Anywhere on foot | Soles, edges |
| Itch intensity | Moderate to intense | Mild | Intense | Moderate |
| Odor | Often present | Rare | Rare | Rare |
| Blisters | Possible | No | Yes (dyshidrotic) | No |
| Scale color | White/red | White/gray | Red | Silvery white |
| Responds to antifungal | Yes | No | No | No |
| Contagious | Yes | No | No | No |
If antifungal cream has not worked in 2 to 4 weeks, the cause is almost certainly not fungal.
Red Flag Symptoms — When to See a Doctor Immediately

Most cases of peeling feet are mild and respond to home treatment. But some signs mean you need prompt medical attention.
See a doctor right away if you notice:
- Spreading redness, warmth, or swelling that suggests infection spreading to deeper tissue
- Pus, open sores, or oozing from the affected area
- Fever alongside foot symptoms
- Severe pain when walking
- Peeling in a person with diabetes — even minor foot infections can become serious
- Symptoms that do not improve after 2 to 4 weeks of appropriate home treatment
- A rash that keeps coming back after treatment
Practical Prevention Tips for Peeling Feet
Prevention is straightforward once you know the main triggers.
Foot Hygiene Essentials
Wash your feet daily with mild soap and dry them thoroughly — especially between the toes. Moisture between the toes is where most fungal infections start.
Trim toenails regularly and keep them clean. Avoid walking barefoot in public locker rooms, showers, or pool decks.
Footwear Choices That Matter
Choose breathable shoes made from natural materials. Rotate footwear so shoes have time to dry out completely between uses.
Wear moisture-wicking or cotton socks. Change socks immediately when they become damp from sweat or activity.
Moisturizing Routine That Works
Apply a cream or ointment moisturizer every night before bed. Pull on a pair of cotton socks right after to lock in the moisture.
Look for fragrance-free formulas. Ingredients like urea, lactic acid, shea butter, and glycerin work well for dry, cracked foot skin.
| Ingredient | Best For | How It Works |
|---|---|---|
| Urea (10–25%) | Thick calluses, heels | Exfoliates and hydrates |
| Lactic acid | Dry, flaky skin | Gently removes dead cells |
| Shea butter | General dryness | Seals in moisture |
| Glycerin | General dryness | Draws water into skin |
| Petroleum jelly | Very cracked skin | Barrier, seals moisture |
How Doctors Diagnose the Cause of Peeling Feet
A doctor or podiatrist can usually identify the cause by looking at the pattern and location of peeling and asking about symptoms.
If a fungal infection is suspected, a small skin scraping is taken. It is treated with a potassium hydroxide (KOH) solution that dissolves skin cells so fungal elements are visible under a microscope. Results are typically available the next day.
In some cases, a fungal culture is sent to the lab to identify the exact type of fungus. This takes about three weeks but is useful for recurrent or treatment-resistant cases.
For suspected eczema or psoriasis, a dermatologist may perform a skin biopsy to confirm the diagnosis.
Treatment Summary by Cause
| Cause | First-Line Treatment | When to Escalate |
|---|---|---|
| Athlete’s Foot | OTC antifungal cream (2–4 weeks) | Oral antifungal if no improvement |
| Dry Skin | Daily thick moisturizer, cooler showers | Dermatologist if no improvement |
| Eczema | Fragrance-free moisturizer, mild steroids | Prescription topicals, biologics |
| Psoriasis | Prescription topicals | Phototherapy, oral/injectable biologics |
| Hyperhidrosis | Breathable footwear, antifungal powder | Prescription antiperspirant |
| Contact Dermatitis | Eliminate trigger, hydrocortisone | Patch testing, prescription steroids |
| Sunburn | Aloe, moisturizer, SPF prevention | Medical care if blistering is severe |
| Dehydration | More water, topical moisturizer | Rule out underlying health conditions |
Frequently Asked Questions (FAQs)
Is peeling feet always a sign of a fungal infection?
No. Peeling feet can be caused by dry skin, eczema, psoriasis, sunburn, or excessive sweating. Fungal infection is common but not the only explanation.
How do I know if my peeling feet are from athlete’s foot?
Athlete’s foot usually causes peeling between the toes with itching, burning, and often a foul odor. Dry skin peeling tends to be on the heels and soles with no odor.
Can I use antifungal cream if I’m not sure what’s causing the peeling?
You can try it if symptoms suggest athlete’s foot, but if there is no improvement after 2 to 4 weeks, see a doctor as the cause may not be fungal.
How long does it take for athlete’s foot to clear up?
With consistent OTC antifungal treatment, most cases improve within 2 to 4 weeks. Severe or widespread cases may need oral antifungals prescribed by a doctor.
Can peeling feet spread to other parts of the body?
If the cause is athlete’s foot, the fungus can spread to toenails, the groin (jock itch), and hands if you scratch your feet and touch those areas.
Should I peel the skin off my feet myself?
No. Pulling or picking at peeling skin can break the skin barrier, cause pain, and create an entry point for bacterial infection.
Can dehydration really cause my feet to peel?
Yes. Poor internal hydration weakens the skin barrier, leading to dryness and peeling. Drink enough water and use a moisturizer to address both causes.
Are people with diabetes at higher risk for foot-peeling complications?
Yes. Diabetes affects circulation and immune response, making even minor foot skin issues more likely to become serious infections. Any peeling in a diabetic foot needs prompt attention.
Can children get peeling feet from fungal infection?
Yes, though it is less common in young children. Athlete’s foot can affect children, especially those who use communal showers in schools or sports facilities.
Is it safe to go swimming if my feet are peeling from athlete’s foot?
Avoid barefoot contact with pool decks and locker room floors. The fungus spreads easily in those environments. Wear pool shoes and cover affected skin where possible.
Conclusion
Why are my feet peeling is a question with multiple answers — and finding the right one changes everything about treatment.
Athlete’s foot is the most common fungal culprit, but dry skin, eczema, psoriasis, contact dermatitis, hyperhidrosis, sunburn, and dehydration are all legitimate causes that need different approaches.
The key is paying attention to where the peeling appears, what the skin looks and feels like, and whether there is itching, odor, or blistering.
Most cases respond well to home treatment when you catch them early and use the right remedy for the right cause.
If your symptoms are severe, spreading, painful, or you have diabetes, do not wait — see a doctor or podiatrist.
For everyone else, consistent foot hygiene, moisture control, breathable footwear, and the correct topical treatment will have your feet healthy and smooth again in weeks.
Your feet carry you everywhere. They deserve consistent attention and care year-round, not just when something goes wrong.